Modern Research in Inflammation
Vol. 2 No. 2 (2013) , Article ID: 31112 , 7 pages DOI:10.4236/mri.2013.22003
Effect of Morinda citrifolia L. fruit juice on gingivitis/periodontitis
![]()
1Institute of Experimental and Clinical Pharmacology and Toxicology, University Clinic, Hamburg, Germany; *Corresponding Author: westendorf@uke.de
2Oro-Dentale Mikrobiologie, Labor Dres. Hauss, Kiel, Germany
Copyright © 2013 Jonas Glang et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received 25 February 2013; revised 25 March 2013; accepted 25 April 2013
Keywords: Gingivitis; Periodontitis; Morinda citrifolia L.; Noni; Bacterial inflammation; interleukin-1
ABSTRACT
The majority of the world’s population suffers from gingivitis/periodontitis. This inflammatory process is caused by several bacterial species inside the dental plaque. In vivo and in vitro experiments were set up. The patients of the in vivo group were divided into a noni and a control group. Both groups contained patients that suffered from gingivitis/periodontitis who were introduced to practice standardized, good oral hygiene. The patients in the noni group additionally used noni juice for mouth wash two times a day. The Papillae-Bleeding-Index (PBI) was evaluated comparing the status of inflammation in both groups. Bacterial probes were isolated from the patient’s gingival pouches for species identification and to carry out in vitro experiments for possible antimicrobial effects of noni juice. The Papillae-Bleeding-Index (PBI) in the noni group has “highly significantly” improved from an average of 2.25 at the beginning of the observation period (t0) to 1.01 after four weeks of noni treatment (t1), compared to a change from 2.11 at t0 to 1.95 at t1 in the control group. A comparison of the differences of the PBI-values (t0-t1) between the noni and the control group was highly significant using a t-test on a level of p = 0.01. Only small inhibition zones were observed in the agar diffusion test on agar plates coated with aerobic, anaerobic and Candida cultures isolated from the patients gingival pouches after treatment with original or neutralized noni juice in different concentrations. Weak bacteriostatic effects occurred in the agar dilution experiments with noni juice in higher concentrations (native and neutralized noni juice). The present investigation has shown that the combination of good oral hygiene and the administration of noni juice was a promising treatment for gingivitis and periodontitis. The additional treatment with noni juice significantly mitigated the gingival inflammation.
1. INTRODUCTION
Gingivitis and periodontitis are wide spread diseases in industrial countries and responsible for early loss of teeth. Hormone dependent contributing factors of gingivitis are puberty, pregnancy, diabetes or the menstrual cycle [1]. Nonspecific bacterial mass in supragingival plaque is known to induce gingival inflammation [2]. Plaque-induced diseases, such as gingivitis and periodontitis, are linked to fluctuations in the oral environment which lead to a change in the microbial composition. Gingivitis is usually caused through inadequate dental hygiene, which has taken place over a certain period of time. The gingivitis is triggered by a plaque accumulation of the bacteria. More than 500 different species of oral bacteria are known, but only some of it can cause gingival diseases [3]. Insufficient hygiene of oral cavities and teeth abets the growth of pathological bacteria which is the most prominent reason for the development of plaque induced gingivitis.
Recent experimental studies and clinical examinations have demonstrated that there are a number of gramnegative bacteria, such as Porphyromonas gingivalis, Actinobacillus actinomycetem comitans, Fusobacterium peridontium, Eikenella corrodens, Bacteroides forsythus, Campylobacter rectus and Treponema denticola, that can be considered to be pathogenic factors in periodontal diseases [4]. Campylobacter rectus and Fusobacterium nucleatum are usually found in nearly all dental plaque samples, and are significant in the formation of dental plaque [5,6]. If gingivitis remains untreated, the process can exacerbate and lead to an irreversible condition of periodontitis. This includes the loss of teeth supporting structures which finally leads to the loss of teeth. Therefore, the prevention or reduction of gingivitis is regarded to be the most effective way to eliminate the possibility of periodontitis [7].
The bacterial infection is, however, not the only reason for an established inflammation present in gingivitis. Science now focuses more and more on the reactions of the immune system [8]. The progression of a periodontal disease is increased by the level of stimulation and activity of reactive oxygen species and proteolytic enzymes, that are released under the influence of an interaction between the host cells, especially neutrophilic granulocytes, and the bacteria [9]. The host defends itself against the bacterial invasion through the first defense barrier which is characterized by the neutrophilic leucocytes, which are specified in killing pathogenic microorganisms [10-12]. The destruction of the gingival tissue is therefore triggered by the bacterial infection itself and the progression of the inflammation which is steered by the host-immune-system. In the case of an established gingivitis, the concentration of cytokines, such as interleukin 1(IL-1), leucotrien B4(LTB4), prostaglandin E2(PGE2), thromboxan B2(TBX) und tumor necrosis factor α (TNF- α) is relatively higher, compared to healthy gingival tissue. The concentration of IL-1, LTB4, and PGE2 is again higher in individuals with an IL-1 gene polymorphism [13]. Gingival tissue with a higher IL-1 activity shows a clinical situation which is worse, compared to patients with lower IL-1 activity. The higher the activity of these cytokines, the stronger is the lesion of the gingival tissue [14]. In addition, the level of metalloproteinases (MMP) plays a role in the destruction of the gingiva as well. MMPs are highly related to gingival tissue destruction and remodeling events in periodontal disease [15,16].
Plants have always been among the common sources of medicines, either processed as traditional preparations or used to extract active principles. The large chemical diversity of secondary plant metabolites, which are mostly targeted to animal physiology, makes it a promising source for new therapeutic candidates for a great variety of diseases.
Morinda citrifolia L. (noni) is a common traditional medicinal plant of the native people of the South Pacific, who used all parts of the plant for the treatment of a broad variety of diseases, including gingivitis [17-20].
During the last 15 years numerous in vitro and in vivo investigations have been published about the biological activity of noni. In most cases a juice prepared from ripe noni fruits was used for these studies. Among many positive effects on health, current research results claim that noni juice is beneficial for antifungal effects [21], bacterial infections [22,23], inflammations [24,25], immune enhancements [26,27] and analgesic effects [28].
In the present investigation we studied the influence of a daily treatment of teeth and gingiva with a fruit juice prepared from Morinda citrifolia L. (noni).
2. MATERIALS AND METHODS
Eleven patients with moderate to severe gingivitis/periodontitis were selected for a pilot clinical study and divided into a control group and a verum group. The study was divided into an in vitro and in vivo part. In the casuistic in vivo part, the chosen patients were randomly allocated to a control (N = 5) and a noni group (N = 6). All patients were comprehensively informed about the aim and procedures of the study and written consents were received.
Five patients were in the control group, and six were in the noni group. Among the patients was also a pair of female identical twins, one in each group. Bacterial samples were taken at the beginning (t0) from each patient in both groups. Afterwards, the Papillae-Bleeding-Index (PBI) was measured according to “Saxer and Mühlemann” [29].
This index is suitable for epidemiological and experimental studies. It divides gingivitis into Grades 0 - 4, with regard to the extent of the periodontal disease. The approximal-plaque-index (API) and the plaque-index (PI) were also measured. Patients in both groups were instructed in methods to achieve proper oral hygiene (standardization of mouth hygiene). Patients in the noni group additionally had to rinse 30 ml noni juice plus 30 ml water in the mouth for 2 min with subsequent swallowing twice a day for a total duration of four weeks (standardized mouth hygiene plus noni juice treatment). Photographs of the gingival situation of the patients were taken (Figure 1). The bacteriological and inflammation status of the patients was also investigated over a period of four weeks. After termination (t1) all patients were examined again.
The bacterial samples taken in the in vivo part (t0 and t1), were analysed in the laboratory. The antimicrobial profile and the sensitivity of the bacteria towards noni juice were investigated. Cultures of Actinobacillus actinomycetem comitans (A.a.), Porphyromonas gingivalis (P.g.), Tannerella forsythia (T.f.), Prevotella intermedia (P.i.). Treponema denticola (T.d.), Campylobacter rectus (C.r.), Fusobacterium nucleatum (F.n.), Eikenella corrodens (E.c.), Capnocytophaga spp. (Cap.), Peptostreptococcus micros (P.m.) and Eubacterium nucleatum (E.n.) were created and used for the in vitro experiments. The cultivation of aerobic and microaerophilic pathogens was achieved by a dilution series of 100 µl of bacterial sus pensions on non-selective and selective culture media.

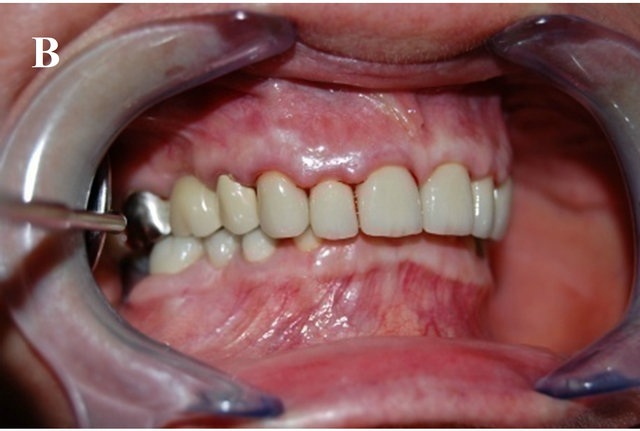
Figure 1. Gingival bleeding after PBI-probing: t0 = beginning of the experiment (A); t1 = after termination of the experiment (B).
The cultivation was carried out on blood-Agar, KimmigAgar and China-Blue-Lactose-Agar, on Trypticase-SoyBacitracin-Vancomycin agar and Chocolate agar (Oxoid, Wesel, Germany). Gram-negative anaerobes were cultured on Wilkins-Chalgren agar (MAST, Reinbek, Germany), supplementeyvitamin K1. The aerobic bacteria cultivation time was 48 hours at 37˚C. The cultivation of microaerophilic bacteria was carried out for 3 days in 5% CO2 atmosphere. The Gram-negative anaerobes were incubated for 5 days at 37˚C in an anaerobic atmosphere (AnaeroGen system, manufactured by Oxoid, Wesel, Germany). The identification and quantification of aerobic, microaerophilic and anaerobic colonies were carried out under the aid of the identification system Remel (from Oxoid, Wesel, Germany) and with the help of spottesting.
In vitro experiments were performed with aerobic and anaerobic bacteria isolated from gingival sites of the patients. Candida cultures obtained from the patient’s saliva were also examined.
2.1. Test for Minimum Inhibitory Concentration (MIC) of Noni Juice in Strains of Bacteria and Candida
The testing of bacteria (aerobic and anaerobic) and Candida were performed with acidic native and neutralized noni juices. The neutralization was performed with a phosphate buffer (from Immuchrom GmbH, 1 molar, pH 7.4). For the experiments with the aerobic and anaerobic bacteria, aliquot dilutions of the noni juice with 0.9% NaCl were prepared in descending manner. The following concentrations were used (noni juice:NaCl): 1:2, 1:4, 1:8, 1:16, 1:32, 1:64. The influence of noni juice on the growth of the bacteria was investigated by replating an aliquot of the individual wells on an agar plate and incubation for 18 h for aerobic and 96 h for anaerobic bacteria at 37˚C.
2.2. Agar Diffusion Test with Noni Juice
Both, the native and the neutralized juices were applied to the aerobic and anaerobic bacteria, and Candida strain using the “filter plate” method. The facultative anaerobic strains were spread on DST agar using an inoculum of 0.5 OD. Filter plates with a diameter of 5 mm were soaked with fresh native noni juice in different volumes and placed on the prepared culture media. As a positive control, another plate was treated with ciprofloxacin. This test was also conducted with noni juice of pH 7. The anaerobic strains of the patients were spread on Schaedler agar using an inoculum of 1.0 OD, and the Candida strains were spread on Kimmig agar using an inoculum of 2.0 OD. Both were then treated similarly to the aerobic bacteria.
2.3. Agar Dilution Test with Noni Juice
Agar dilution tests of aerobic and anaerobic bacteria were performed using native and neutralized noni juice. Holes with a diameter of 3 mm were punched into the agar of the cultures using a sharp tip. Native or neutralized noni juice was filled into these wells.
2.4. Agar Diffusion Test with Noni Concentrate (6-Fold versus Native Noni Juice)
Aerobic and anaerobic microorganisms were investigated in this experiment. Filter plates according to previous experiments were placed on the agar plates and supplemented with different volumes (20, 40, 60 µl) of noni concentrate. A fourth “blank plate” which served as a control was placed on the culture as well.
Particular attention was given to a selected aerobic spore (Bacillus species), with special sensitivity to antimicrobial agents. Experiments were carried out in the same way with anaerobic germs and Candida.
2.5. Agar Dilution Test with Untreated versus pH Neutralized Noni Concentrate
These Experiments were conducted with aerobic and anaerobic bacteria and Candida using noni concentrate. The experiments were focussed on the strains Pseudomonas aeruginosa, Citrobacter freundii, Stenotrophomona smaltophilia, and Klebsiella oxytoca. Noni concentrate (native or neutralized) was filled into the wells of the culture plates and incubated as described. The experiments were repeated with the anaerobic bacterial strains, as well as Candida strains using the appropriate agar plates and the procedure given above.
3. RESULTS
3.1. In Vivo Experiments
Clear differences in gingival inflammation were detected in the control group after introduction of a hygiene standard at the beginning compared to four weeks later (Table 1 and Figure 2). In the noni group, these differences were, however, much clearer. The Papillae-Bleeding-Index (PBI) in the noni group has “highly significantly” improved from an average of 2.25 at the beginning of the observation period (t0) to 1.01 after four weeks of noni treatment (t1), compared to a change from 2.11 at t0 to 1.95 at t1 in the control group (Table 2). Acomparison of the differences of the PBI-values (t0-t1) between the noni and the control group were highly sig nificant using a t-test on a level of p = 0.01. The indices
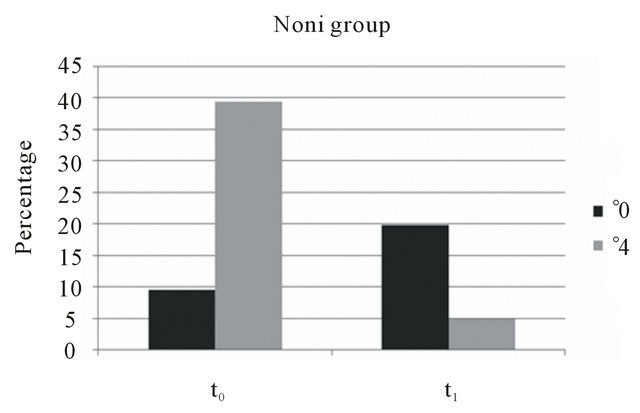
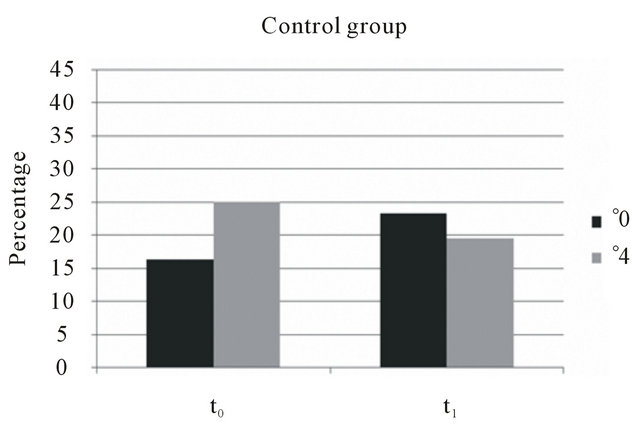
Figure 2. Mean percentage distribution of ˚0 and ˚4 PBI levels in the noni and control group.t0 is the output measurement, t1 is the final measurement. ˚0 describes an inflammation, nonbleeding, healthy gingiva. ˚4 describes a maximum of inflamed, bleeding, diseased gingival (B).
API and PI showed a slight improvement. In the control group an improvement was measurable also, even this was less pronounced. No significant differences were observable in the noni treatment versus the control group comparing the bacterial status of the gingival pouches at the beginning with that of the final examination, neither in quantity nor quality.
3.2. In Vitro Experiments with Aerobic and Anaerobic Bacteria and Candida
An overview of the results of the in vitro experiments is shown in Tables 3 and 4. A complete inhibition of bacterial growth, either aerobic or anaerobic, was ob served at noni juice dilutions of 1:2 and 1:4. No measureable inhibition could be observed after treatment of the Candida cultures. Only small inhibition zones were observed on plates coated with aerobic, anaerobic and Candida cultures in the agar diffusion test with original or neutralized noni juice. Weak bacteriostatic effects occurred also in the agar dilution experiments with noni juice (native and neutralized).
In contrast, extensive inhibition zones resulted in the agar diffusion test, if bacterial or Candida cultures were treated with noni concentrate. The inhibition zones were smaller when neutralized noni concentrate was used.
4. DISCUSSION
The aim of the present study was to investigate the possible positive effect of noni juice on patients with gingivitis/periodontitis. Although a clinical improvement could be observed during four weeks after performance of a standard hygiene protocol only, the results weremore pronounced after additional treatment with noni
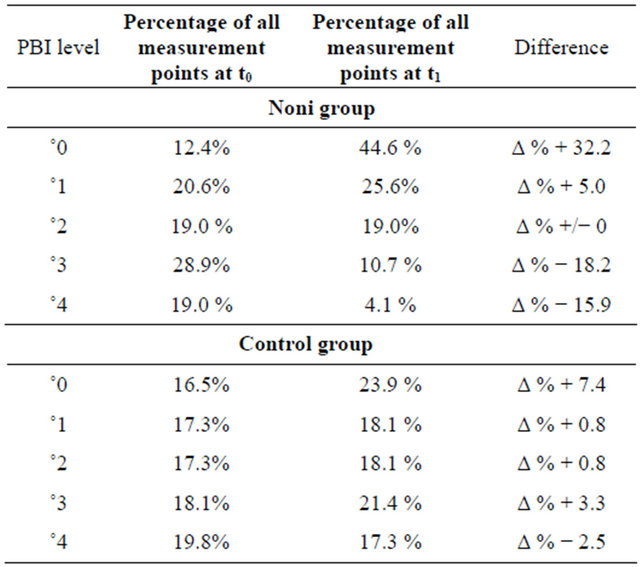
Table 1. Papillae-Bleeding-Indices (PBI) of the control and noni group before (t0) and after treatment (t1).
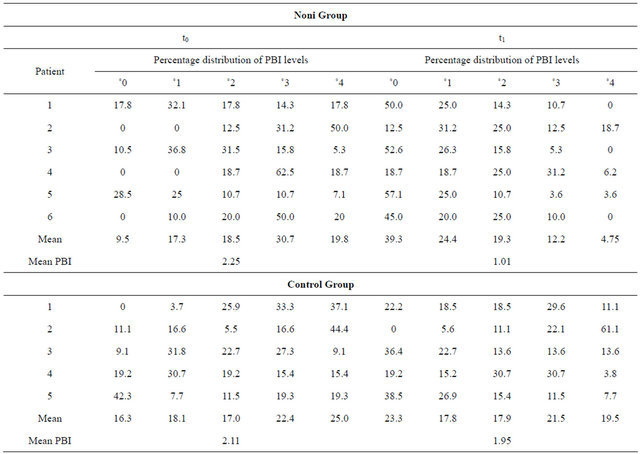
Table 2. Development of the papillae-bleeding-indices in the noni and control group. t0 is the output measurement, t1 is the final measurement.
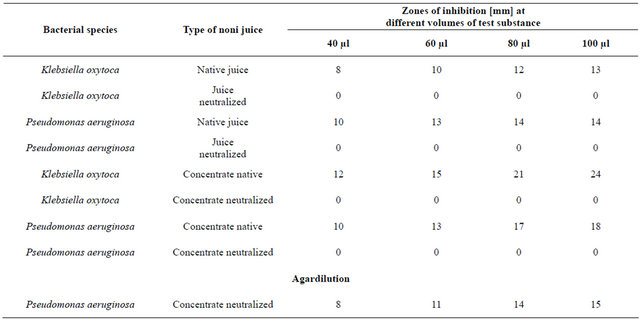
Table 3. Inhibition zones of the growth of a variety of aerobic bacterial species, isolated from patients gingival pouches, resulting from incubation with different noni preparations at different concentrations.

Table 4. Inhibition zones of the growth of a variety of anaerobic bacterial species, isolated from patients gingival pouches, resulting from incubation with different noni preparations at different concentrations.
juice (locally and systemically). The reason for the ef fect caused by noni juice could be either a reduction of the bacterial situation of the gingiva and/or of the inflammation associated with gingivitis/periodontitis. Direct inhibition of bacterial growth by noni juice was very limited.
Only a moderate effect of noni juice could be demonstrated in the in vitro experiments performed with aerobic and anaerobic bacteria, isolated from gingival sites of the patients. This effect was almost completely abolished after neutralization of the acidic noni juice. The toxic effect of noni juice on microorganisms is therefore most probably due to the low pH-value rather than to compounds with antimicrobial activity. Antimicrobial activity independently of the pH-value could however be obtained with a six-fold concentrated noni juice. The investigation of the bacterial composition in the oral cavity of the patients did not change, neither qualitatively nor quantitatively, during the treatment phase with noni juice. Nevertheless, significant improvements in the clinical situation of patients after four weeks of noni treatment versus controls were observed (Figure 1).
In the absence of a strong antibacterial effect, the beneficial effect of noni juice on gingivitis/periodontitis is most probably a result of its well known anti-inflammatory activity. Anti-inflammatory effects of noni juice were reported in several publications. Mechanisms responsible for these effects were the inhibition of cytokines, such as COX-2, TNF-α, IL-1α (β), IL-8 and IL-6 [25,28] and receptor antagonism of bradykinin, an important trigger of inflammation [26]. As a result of the possible modulation of the host immune response, a reepithelialisation may take place under the influence of noni juice, as the inflammatory signals are attenuated. Inflammatory signalling molecules such as PGE2, IL-1β and TNF-α are inhibited by noni juice [30]. There is also sufficient evidence for the inhibition of the activity of Metalloproteinases (MMP-9) under the influence of noni juice [28].
The fact that the inflammation and not the quantity or quality of the bacterial influence was altered by noni juice is furthermore supported by the results with the identical twins. Both had a roughly equal not plaque induced gingivitis. However, the reduction of inflammatory events of the twin in the noni group was far clearer compared to her sister in the control group.
The use of other drugs to inhibit inflammation, such as NSAID or the administration of Low Dose Doxycycline for the reduction of MMP activity or the use of bisphosphonates to inhibit the activity of the osteoclasts in context with periodontal diseases may be rethought. Not least because of serious side effects that the mentioned drugs may cause. The administration of NSAIDs could be reduced because an inhibition of inflammation is also supported by noni juice, which is free of side effects. The activity of MMPs, which are largely responsible for the degradation of the periodontium, can be reduced by noni juice as well [28]. Further investigations are warranted to confirm these preliminary findings.
5. CONCLUSION
The present investigation has shown that the combination of good oral hygiene together with local and systemic treatment with noni juice is a promising tool for the treatment of gingivitis and periodontitis.
6. ACKNOWLEDGEMENTS
The study was supported by a grant from Tahitian Noni International Inc., Provo, Utah, USA. This company provided also noni juice and noni concentrate that were used in this study. We thank Joachim Gordon Justus Glang for providing the facility and equipment for the clinical investigations.
REFERENCES
- Löe, H. and Silness, J. (1963) Periodontal disease in Pregnancy. I. Prevalence and severity. Acta Odontologica Scandinavica, 21, 533-551. doi:10.3109/00016356309011240
- Raber-Durlacher, J.E., Leene, W., Palmer-Bouva, C.C., et al. (1993) Experimental gingivitis during pregnancy and post-partum: Immunohistochemical aspects. Journal of Periodontology, 64, 211-218. doi:10.1902/jop.1993.64.3.211
- Socransky, S.S., Haffajee, A.D., Cugini, M.A., et al. (1998) Complexes in subgingival plaque. Journal of Clinical Periodontology, 25, 134-144. doi:10.1111/j.1600-051X.1998.tb02419.x
- Ihara, H., Miura, T., Kato, T., et al. (2003) Detection of Campylobacter rectus in periodontitis sites by monoclonal antibodies. Journal of Periodontal Research, 38, 64-72. doi:10.1034/j.1600-0765.2003.01627.x
- Darveau, R.P., Tanner, A. and Page, R.C. (1997) The microbial challenge in periodontitis. Journal of Periodontology, 14, 12-32. doi:10.1111/j.1600-0757.1997.tb00190.x
- Dzink, J.L., Tanner, A.G.R., Haffajee, A.D., et al. (1995) Gram-negative species associated with active destructive periodontal lesions. Journal of Clinical Periodontology, 12, 648-659. doi:10.1111/j.1600-051X.1985.tb00936.x
- Marsh, P.D. (1995) Microbial ecology of dental plaque and its significance in health and disease. Advances in Dental Research, 8, 263-271.
- Lindhe, J., Karring, T. and Lang, N.P. (1999) Anatomy of the parodontium. Clinical parodontology and implantology. Quintessenz, Berlin, Chicago, London, Paris, Tokio, Barcelona, Moskau, Prag, Sao Paulo, Sofia, Warschau.
- Sheikhi, M., Gustafsson, A. and Jarstrand, C. (2000) Cytokine, élastase and oxygene radical release by Fusobacteium nucleatum—activated leucocytes: A possible pathogenic factor in periodontitis. Journal of Clinical Periodontology, 27, 756-762. doi:10.1034/j.1600-051x.2000.027010758.x
- Seymour, G.J. (1991) Importance to the host response in the peridontum. Journal of Clinical Periodontology, 18, 421-426. doi:10.1111/j.1600-051X.1991.tb02310.x
- Witko-Sarsat, V., Rieu, P., Descamps-Latscha, B., et al. (2000) Neutrophils: Molecules, functions and pathophysiological aspects. Laboratory Investigation, 80, 617-653. doi:10.1038/labinvest.3780067
- Follin, P., Wyman, M.P., Dewald, B., et al. (1991) Human neutrophil migration into skin chamber is associated with production of NAP-1/IL-8 and Ca5. European Journal of Haematology, 47, 71-76. doi:10.1111/j.1600-0609.1991.tb00564.x
- Heasman, P.A., Collins, J.G. and Offenbacher, S. (1993) Changes in cervicular fluid levels of interleukin-1 beta, leucotriene B4, prostaglandin E2, thromboxane B2 and tumor necrosis factor alpha in experimental gingivitis in humans. Journal of Periodontal Research, 28, 241-247. doi:10.1111/j.1600-0765.1993.tb02090.x
- Dewhirst, F.E., Moss, D.E. and Offenbacher, S. (1983) Levels of prostaglandin E2, thromboxane, and prostacyclin in periodontal tissues. Journal of Periodontal Research, 18, 156-163. doi:10.1111/j.1600-0765.1983.tb00348.x
- Dahan, M., Nawrocki, B., Elkaim, R., et al. (2001) Expression of matrix metalloproteinases in healthy and diseased gingiva. Journal of Clinical Periodontology, 28, 128-136. doi:10.1034/j.1600-051x.2001.028002128.x
- Heath, J.K., Gowen, M., Meikle, M.C., et al. (1982) Human gingival tissues in culture synthesize three metalloproteinases and a metalloproteinase inhibitor. Journal of Periodontal Research, 17, 183-190. doi:10.1111/j.1600-0765.1982.tb01143.x
- Stewart, M. (1972) Noni: The lore of the Hawaiian medicinal plants. Bulletin of the Pacific Tropical Garden, 2, 37-39.
- Parsons, C. (1981) Sickness experience and language: Aspects of Tongan and western accounting. Ph.D. Thesis, University of Waikato, Hamilton.
- Dittmar, A. (1993) Morinda citrifolia L. use in indigenous Samoan medicine. Journal of Herbs, spices and Medicinal Plants, 1, 77-92. doi:10.1300/J044v01n03_08
- Singh, Y.N., Ikahihifo, T., Panuve, M., et al. (1984) Folk medicine in Tonga. A study on the use of herbal medicines for obstetric and gynaecological conditions and disorders. Journal of Ethnopharmacology, 12, 305-329. doi:10.1016/0378-8741(84)90060-6
- Bancree, S. (2006) An extract of Morinda citrifolia L. interferes with the serum-induced formation of filamenttous structures in Candida albicans and inhibits germination of Aspergillus nidulans. The American Journal of Chinese Medicine, 34, 503-509. doi:10.1142/S0192415X0600403X
- Locher, C.P., Burch, M.T., Mower, H.F., et al. (1995) Anti-microbial activity and anti-complement activity of extracts obtained from selected Hawaiian medicinal plants. Journal of Ethnopharmacology, 49, 23-32. doi:10.1016/0378-8741(95)01299-0
- Leach, A.J. (1988) Antibacterial activity of some medicinal plants of Papua New Guinea. Science in New Guinea, 14, 1-7.
- McKoy, M.L.G., Thomas, E.A. and Simon O.R. (2002) Preliminary investigation of the anti-inflammatory properties of an aqueous extract from Morinda citrifolia L. (noni). Pharmacological Society, 45, 76-78.
- Kim, H.J., Jang, S.I., Kim, Y.J., et al. (2004) Scopoletin suppresses pro-inflammatory cytokines and PGE2 from LPS-stimulated cell line, RAW 264.7 cells. Fitoterapia, 75, 261-266. doi:10.1016/j.fitote.2003.12.021
- Hirazumi, A., Furusawa, E., Chou, S.C., et al. (1996) Immunomodulation contributes to the anticancer activity of Morinda citrifolia L. (noni) fruit juice. Proceedings of the Western Pharmacology Society, 39, 7-9.
- Hokama, Y. (1993) The effect of noni fruit extract (Morinda citrifolia L., Indian mulberry) on thymocytes of BALB/c mouse. The FASEB Journal, 7, A866.
- Basar, S., Uhlenhut, K., Westendorf, J., et al. (2009) Analgesic and anti-inflammatory activity of Morinda citrifolia L. (noni) fruit. Phytotherapy Research, 24, 38-42. doi:10.1002/ptr.2863
- Saxer, U.P. and Mühlemann, H.P. (1975) Motivation and education. SSO Schweiz Monatsschr Zahnheilkd, 85, 905-919.
- Xu, J., Mc Sloy, A.C., Anderson, B.K., et al. (2006) Tahitian Noni® equine essentialsTM: A novel anti-inflammatory and a COX-2 inhibitor which regulates LPS-induced inflammatory mediator expression in equine neonatal monocytes. Journal of Veterinary Internal Medicine, 20, 756.

