Advances in Aging Research
Vol. 1 No. 2 (2012) , Article ID: 21861 , 9 pages DOI:10.4236/aar.2012.12002
“What are you interested in?”—A survey on 601 nursing homes residents activities interests
![]()
1Centre Mémoire de Ressources et de Recherche CHU de Nice, Nice, France
2Nursing Home CCAS Ancien Combattant, Nice, France
3Nursing Home Villa Helios, Nice, France
4Nursing Home Résidence Corniche Fleurie, Nice, France
5Nursing Home le Clos de Cimiez, Nice, France
6EA CoBTek, Université Nice-Sophia Antipolis, Nice, France; *Corresponding Author: dechamps.a@chu-nice.fr
7Department of Psychology, University of Pancasila, Jakarta, Indonesia
Received 3 May 2012; revised 3 June 2012; accepted 11 June 2012
Keywords: Dementia; Interests Choice; Institution; Engagement; Survey; Lack of Interest Introduction
ABSTRACT
Lack of engagement in activities is a common feature of nursing homes residents. As apathy is the most frequent behavioural disturbance, understanding residents’ interests is a milestone for tailored challenging interventions targeting engagement enhancement. Objective: To depict the activities interests of nursing homes residents. Method: An electronic version of the Test of Interest “TILT” which regroups 40 images of activities has been developed and adapted for the Ipad. Residents were asked to answer by yes or no to the question “are you interested by this activity”, for each activity found interesting, the patient had then to categorize it in either Work/ occupation-Personal-Leisure-Family. Population: A total of 601 residents from 19 nursing homes have completed the survey from March to May 2011. The surveyed nursing homes from the South East of France were comparable of nursing homes figures in France. Results: We interviewed 601 individuals (female, n = 484) aged 85.9 years, out of those, 56% had stayed more than one year in an institution. Nearly half of the population (45.3%) was from 80 - 89 year of age, followed by 36.1% from 90 - 99. The educational background was principally from primary school (36%) and high school (30.8%). Most of the residents were classified has having dementia (35.3%). From the 40 activities presented to each participant, “enjoying a good meal” has been found to be the most interesting activity by 83% of the population followed by “dressing up”, 75.9% and “watching TV”, 75.5%. Female participants reported more interest in place of worship, family pictures and being with grand children then males (p < 0.01). We found that the presence of “dementia” diagnosis” triggered the lack of interest compared to none demented or none cognitively impaired residents (p < 0.01). It was found that participants aged 55 - 69 were more the most interested to do video games (p < 0.05), though this may be interpreted as a positive step toward functional and cognitive rehabilitation program using virtual reality as a mean for intervention.
1. INTRODUCTION
Behavioural symptoms are core features of Alzheimer’s disease (AD) and related disorders. Irrespective of the severity of the disease, the most frequently observed behavioural symptom is apathy defined as a disorder of motivation [1] with lack of interest as one of the core clinical features [2]. Inactivity resulting from apathy syndrome is drawing concerns about functional autonomy worsening and incremental dependence costs increase as the disease progresses [3,4]. Engaging people in activities is the key component of active lifestyle program and autonomy maintenance. Engagement is defined as the act of being occupied or involved with an external stimulus [5]. However, engaging old adults in meaningful activities [6] has been found to be a challenging issue as apathy syndrome is one the most present behavioural disturbance in institution [7,8].
Although, interventions targeting explicit health benefits using tailored activities have been found to yield positive results in institutionalized old adults, there is little data regarding how engagement as a behavioural process was measured [4,6,9,10]. Personal attributes along with cognitive alteration may trigger how individuals will find meanings and interests in a specific activity [4,11].
Lack of interest and inactivity in patients with dementia and in institutionalized old adults is often seen as a common feature of the aging process; however these have been rarely targeted as main rationale for interventions. As the individuals grow older, interest and social engagement have been found to decrease in social activities [12], nonetheless a better understanding of the extent to which apathy syndrome and interest in particular can be influenced by systemic and ecological interventions is awaited to refine the theory of apathy in dementia. The lack of information regarding which activities might engage nursing homes residents is the principal cause of ill-adapted practices such as living residents sitting in corridors or in front of unspecific television programs. Accordingly, a clarification and quantification of “what” are the interests of institutionalized individuals are milestones to improved tailored interventions. This survey was designed to outline the main interests of old nursing home residents in order to improve the mapping of individuals’ incentives toward activities.
2. METHOD
2.1. Design
This study is a survey of 601 nursing home residents from 19 nursing homes from the South East of France. The surveyed nursing homes are members of the RER research and care network (Réseau EHPAD Recherche) and were volunteers.
The population recruited for this survey is representative of the French nursing home administrative status (public, private, associative). All patients from the nursing homes were considered as potential respondent. This survey is the preliminary part of a trial registered under the clinical trial identifier number NCT 01314131.
2.2. Participants
In each institution, the participant’s characteristics; such as age, sex, level of education and clinical diagnoses were collected from the medical record. Inclusion criteria were having a diagnosis of dementia according to ICD 10 criteria. Patients had to be aged 60 and older and living in institution. Patients below 60 years of age, unable to answer to basic instruction, having aphasia or severe alertness impeding all interactions were not included. Each participant gave an oral consent of his/her willingness to participate; oral consent from the career in charge of their usual care was also required. For anonymous survey, no ethical committee approval is required in France.
3. SURVEY PROCEDURE
The survey included 40 activities images and was administered using an electronic based version. The survey was developed to fit on tactile tablets such as the Ipad® from Apple. A tactile tablet was given free of charge to each nursing homes if they agreed to participate to the survey (n = 19). The electronic survey application is available online at http://cmrr-nice.fr/tests/tilt-public/. The presentation procedure for the images and the repartition of each activity into one of the 5 categories of interest was as follow. Based on the presentation of an activity, each participant was asked to indicate if the activity interested him/her or not. When the participant was interested in the activity a new screen on the Ipad® showed the categories and he/she had to categorize the activity into either Work/occupation, Personal, Leisure, Family or I don’t know [11]. For categorization understanding, the interviewer asked the patient “Are you interested by ”name of the activity”?” if no, then the next activity was presented, if yes, then the interviewer asked “Tell me if it is more related to Work, because it is or was related to your work; Personal because it is personal reasons or related to yourself and personality; Leisure because it is or was related to your leisure, Family because it is related to your family, or You don’t know?”. After the patient expressed his/her choice, the next activity was presented [11].
All data were automatically gathered on a server using automatic transfer via the 3G or Wifi system embedded in each tablet. A standardized two hours training procedure for the interviewers was developed to ensure proper use of the material.
3.1. Data Collection
The interviewer recorded participant’s characteristics; Mini Mental State Examination total score administered within 6 months prior to the survey, age, sex, level of education and in addition, when available, information regarding clinical diagnosis as referred in Table 1 [13].
3.2. Statistics
We explored possible age effect over interest distribution using distribution plots. We initially explored univariate associations between gender, educational background, cognitive functioning assessed with the Mini Mental State Examination and age categories. Severity categories using the MMSE total score were the following: normal cognition: above 26, mild cognitive impairment: 21 to 26, Moderate Cognitive Impairment: 16 to 20, Moderately Severe Cognitive Impairment: 10 to 15, and Severe Cognitive Impairment: below 10 [14].
Choice answers were categorized as follow: the absence
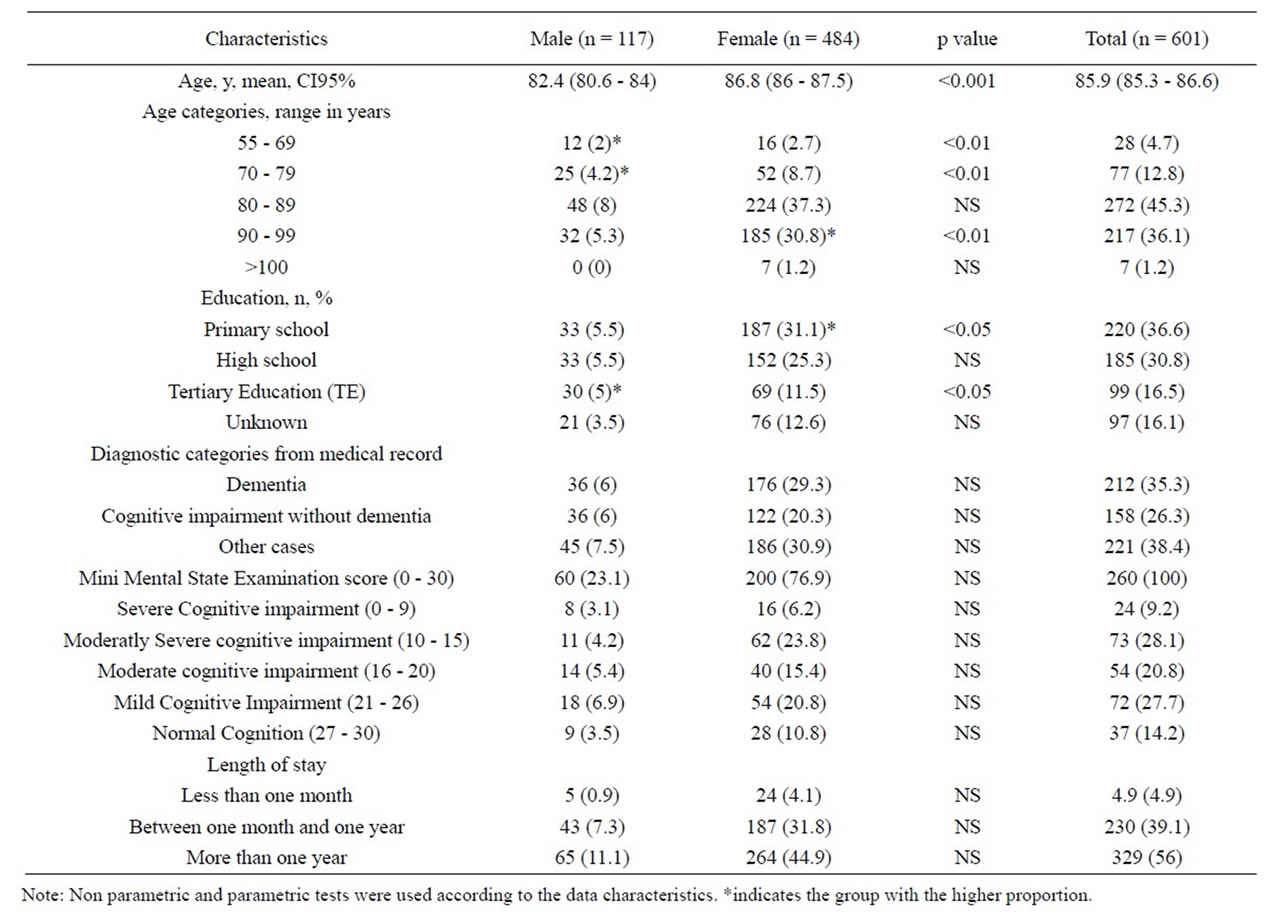
Table 1. Participants characteristics.
of interest or refusal as opposed to interest which was further divided in five categories namely: Work, Family, Leisure, Personal and I don’t know. All variables associated with each category were entered into a multivariate model and used the Wald statistic for dichotomised variables (i.e., each activity) and descendant method for linear regression for continuous variables to identify potential candidates for removal.
To assess the validity of the final model, we compared it with the results of a bootstrapped stepwise model, in which all possible covariates were entered. Model fit was assessed with Hosmer-Lemeshow goodness-of-fit tests. Results are presented according to gender, diagnosis or cognitive status or education weight role. Use either SI (MKS) or CGS as primary units. (SI units are encouraged.) English units may be used as secondary units (in parentheses). An exception would be the use of English units as identifiers in trade, such as “3.5-inch disk drive”.
4. RESULTS
Overall data were entered by psychologist (60%, n = 362) followed by physician or geriatrician (27%, n = 164) and assistant nurse (9%, n = 57), the rest (4%, n = 18) was recorded by activity leaders or other.
After discrepancy analyses we found that two nursing homes did not indicate the education level thus creating an “artificial” difference for the “unknown educational background” category (n = 74). We therefore in analyses comparing the category “Education” have eliminated the “unknown educational background” response thus reducing by 97 the observed population. No difference was found between these residents (n = 97) with unknown educational background and the rest of the population in cognitive and other descriptive data.
A total of 601 residents aged 85.9 ± 8.2 participated in this survey (Table 1).
Based on age distribution of plots for interest, we further divided age into the 5 following age categories: 55 - 69; 70 - 79; 80 - 89; 90 - 99 and above 100. Participants’ descriptive data and interests are shown in Table 1. Most of the participants were aged between 80 and 99 years of age (68.1%) and had primary education (31.1%) with a diagnosis of dementia (29.3%).
Of the 40 activities (Table 2) presented to each participant, “enjoying a good meal” was found the most in-
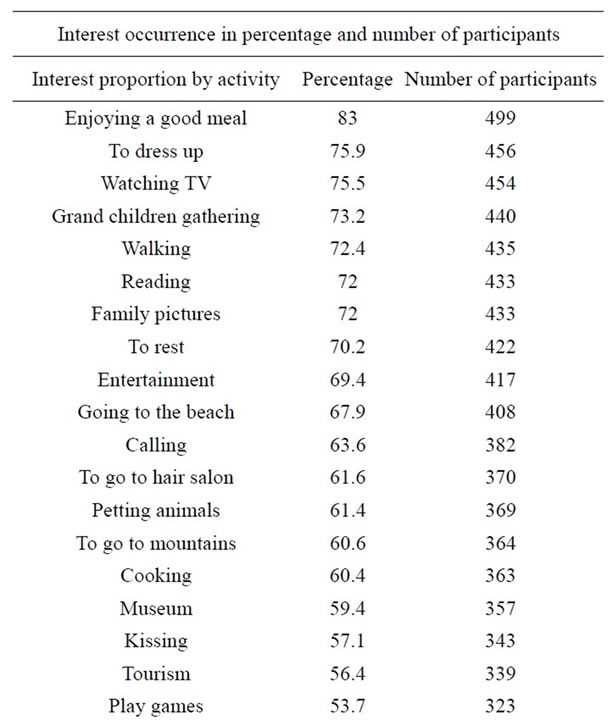

Table 2. Participants interests.
teresting by 83% of the population. Activities such as “watching TV”, “walking” and “reading” along with “to rest” were found to interest more than 70% of the population.
The predictive factors of interest are shown in Table 3. Residents aged between 70 - 79 years of age and above 100 years of age with dementia reported more “Not interested” than their non-demented counterparts.
Individuals with premorbid tertiary education level and severe cognitive impairment showed fewer interests on average than the less cognitively altered residents (Table 3, all p ≤ 0.01). The most prevalent activities of interest such as enjoying a good meal or watching TV were not predict by any of the data collected (Table 4).
We found that participants reporting religious interest had more active interests (n = 318, df = 1, β = 0.26, F = 43, p < 0.000; mean interest difference of 4.9, 95%CI [3.4 - 6.4] and less lack of interest (n = 318, df = 1, β = –0.4, F = 109, p < 0.000, with mean lack of interest difference of –5.4, 95%CI [–6.4 - –4.3]) compared to their counterparts not interested by religion.
4.1. Discussion
The major result of this survey was the acceptability of the method that has been used. None of the resident refused to give his/her point of view. Showing pictures and asking questions using an electronic tablet were well accepted by the residents with or without dementia and the involved professional caregivers. This positive feedback is important as lack of interaction and stimulation are relatively frequent in nursing home and the use of interactive technology can be integrated as an adjunct to therapeutic activities.
The second major result concerns the first ranked interest: “enjoying a good meal”. As participation restriction increases as the disease worsen, basic gustatory pleasure turn out to be a major issue for residents, hence refinement in the preparation and presentation of the food are needed in order to provide enjoyment and interest during meal times in each nursing homes. Furthermore, our results showed that for the activities showing high interest prevalence there was little if no impact of the disease characteristic, gender or educational background. Interestingly we did not found any univariate age-related reduction of interest in our population (Figure 1), thus contrasting with some recent data [15].
In this survey more than 50% of the participants were interested in religious activities. Our results echoes recent data from a French survey involving 1000 participants showing that 30% of the population recognized religion has important in their life [16]. Data from the United States showed that the interest for religious activities increases as the people get older [16]. While our results did not show any age related effect other worship interest, we found that female participants with tertiary and primary education background had more interest in religiosity than their male counterparts. Interestingly, religiousness has been found to be related with better psychological health, furthermore, more spiritual or religious individuals were found to be the most cooperative when interviewed [17]. Others have found that relig-
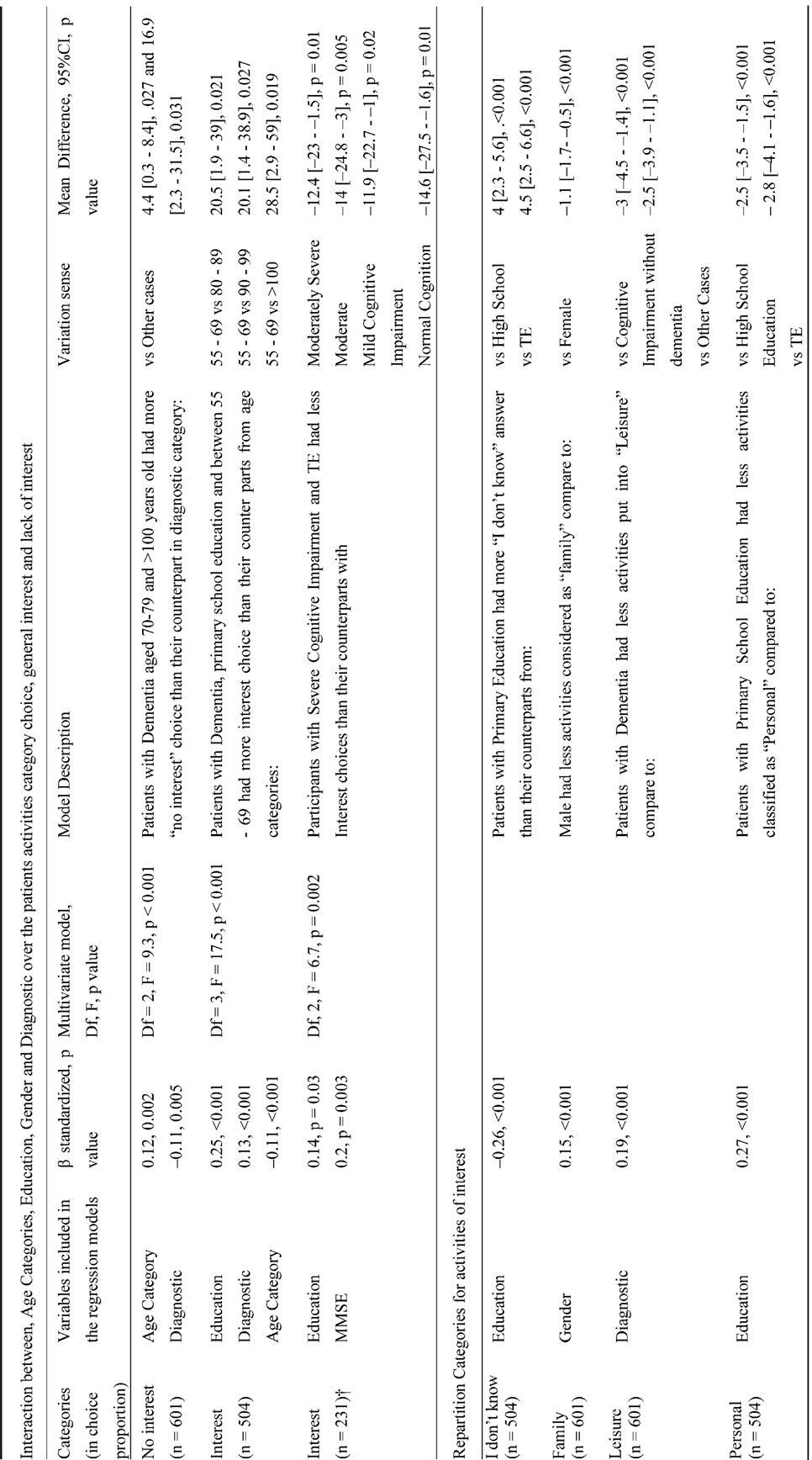
Note: Only significant interactions are integrated in this table. Multiple comparisons p values are adjusted using Bonferroni adjustment. Diagnostic: Dementia, Cognitive Impairment without dementia, other cases; Education: Primary School, High School Level, Tertiary Education: TR; Age Category: 50-69; 70-79;80-89;90-99;>100 No variable was selected in the model including Work category.
† The MMSE was not introduced in the first analysis due to co linearity effect with Diagnosis.
Table 3. Predictive factors of Interest and Categories repartition.
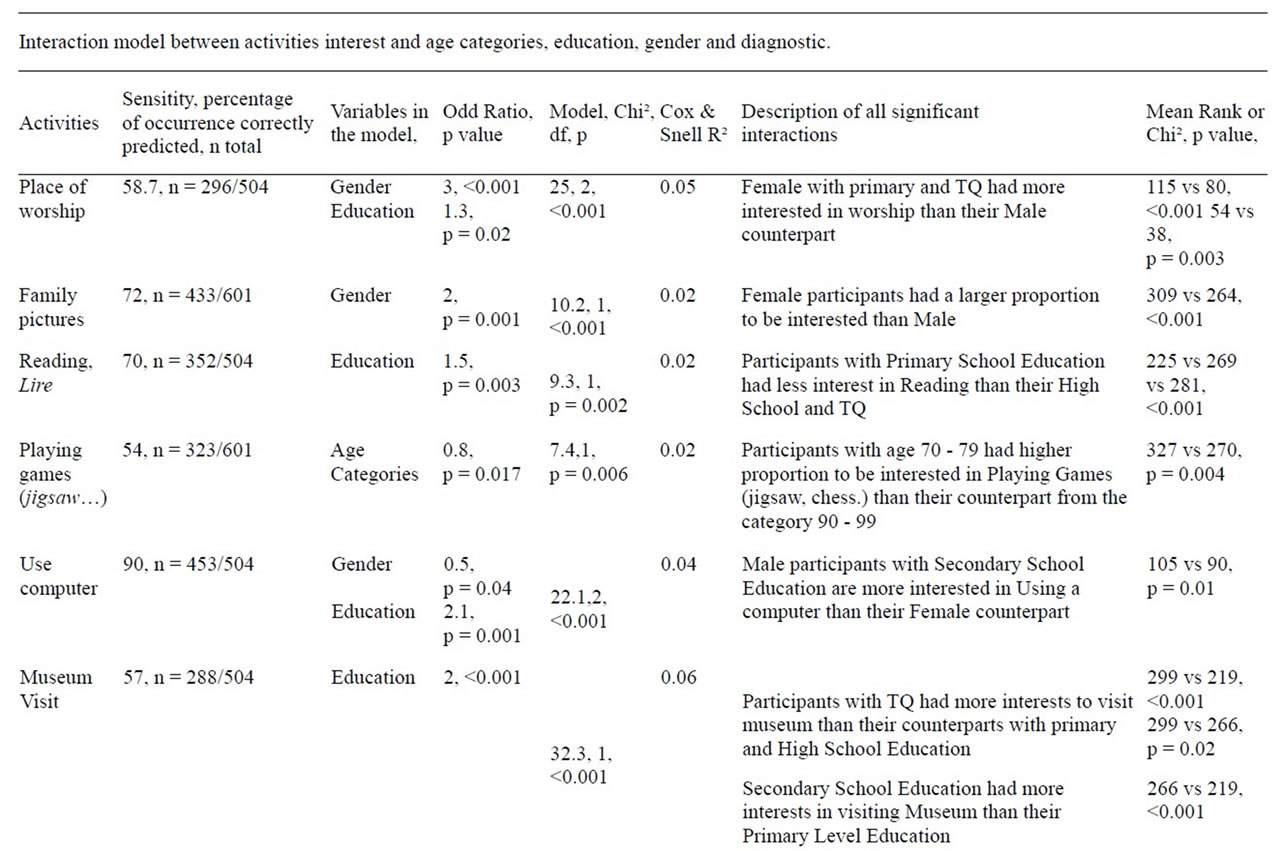
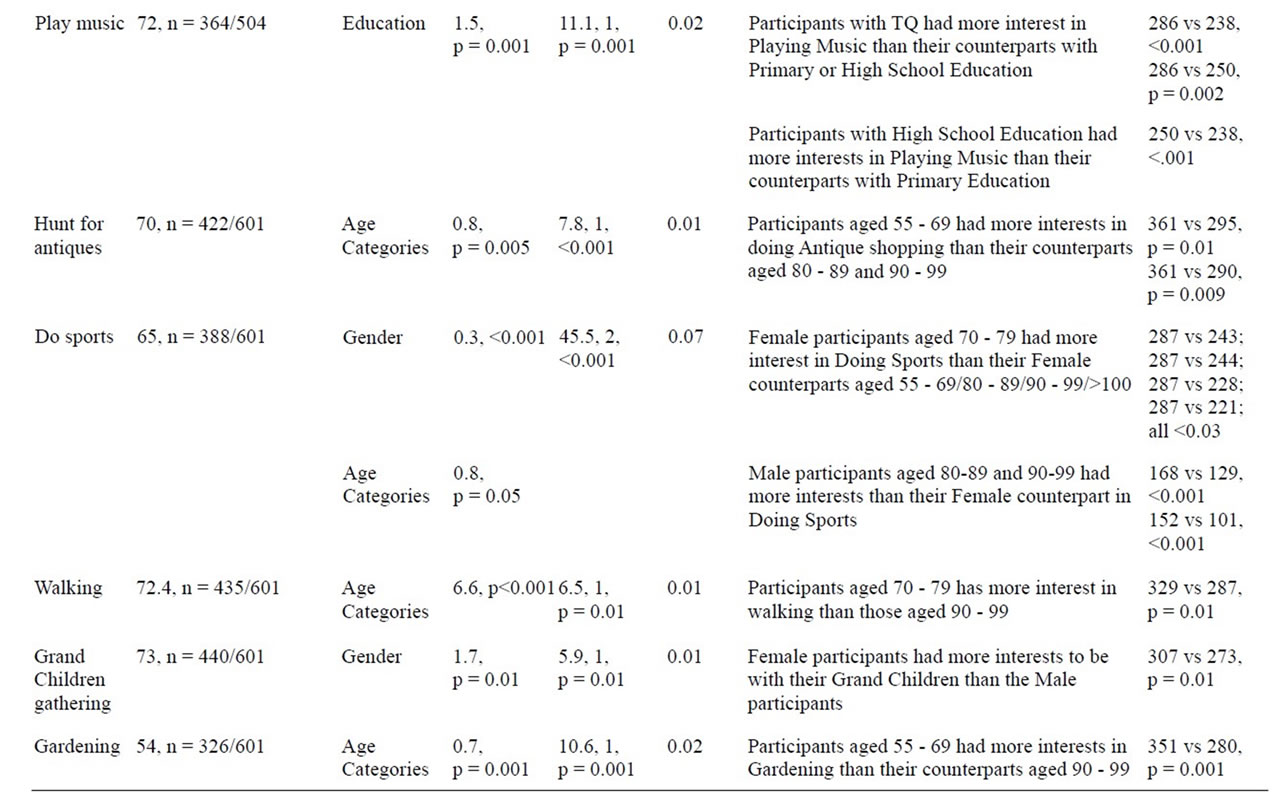
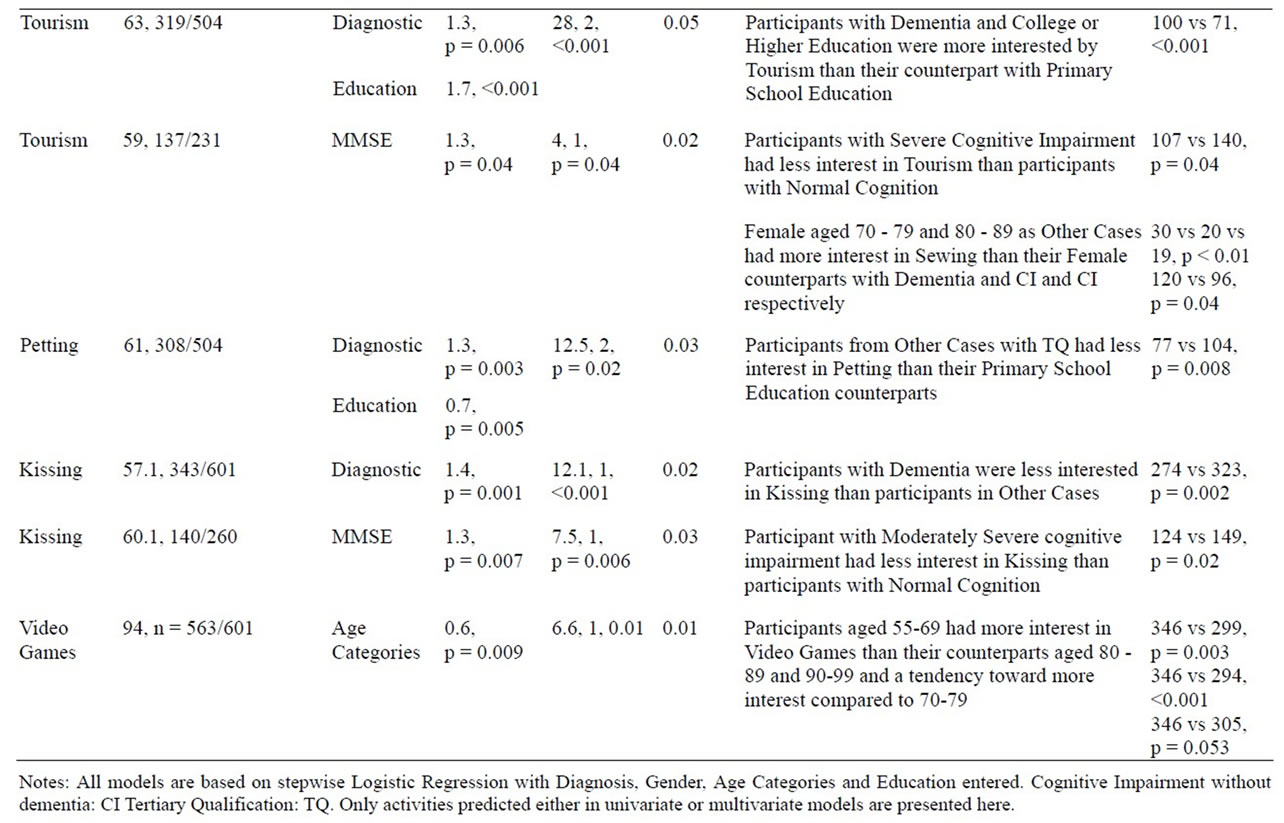
Table 4. Predictive factors of interest by activity.
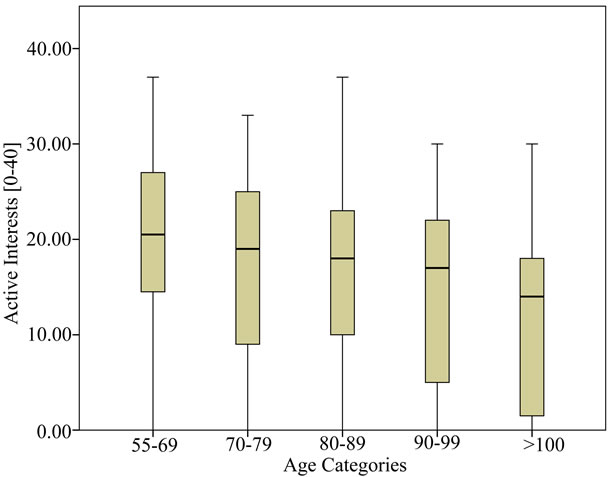
Figure 1. Relation between age and active interests.
iousness is also a key component of coping strategies to manage pain in the later age [18]. As functional dependence increases and social interactions tend to reduce due to institutionalisation, religiousness and spirituality can become coping strategies not only to cope with functional impairment but also to create alternative social activities and produce a feeling of affiliation to a community. However, there is little data available regarding such interactions in institutionalized old adults; thus, clinical investigations are needed to corroborate potential benefits of religiousness over participation, perceived and clinical physical health status [16,19]. Furthermore, the investigation of any potential protective effects of religiousness over lack of interest and apathy symptoms should be made.
Regarding physical activity items of the activities, walking interest prediction was coherent with recent data regarding physical activity and sports from a 16-year follow-up population of elderly residents [20]. The authors found that participants aged 64 - 74 at the survey’s baseline had walking interest/practice of 39.4% and 42.3% for male and female respectively while 16 years later these percentages were 32.8 and 34.8 respectively. Similarly, we found that female participants aged 70 - 79 showed more interests in sports than their older female counterpart, thus corroborating recent data showing that doing physical activity (sport) several times per week to the point of perspiring and heavy breathing interested 18.5% of the population aged 64 - 74 and then dropped to 3.8% for the age category 80 - 90 [20]. We found that men aged 80 - 90 were more interested in sports than female of the same age thus confirming recent results for the same age category [20]. Overall, our results concede the observed increase lack of interest for sport and physical activity over the years. Possible explanation may come from poor perceive health status and the lack of promotion of active lifestyle program [4]. Though more than 70% of the surveyed population was interested in walking, program targeted enjoyable and innovative approach to physical activity are needed as poor health associated with the aging process might decrease the interest for physical activities. As interventional studies need informed consent as mandatory requirement for ethical issue, it can be argued that these studies involving old adults may fall short to recruit the participants who will benefit the more of such approaches as lack of interests and apathy may preclude any positive answers to study participation [6]. All of the above may trigger negative consequences on behavioural compliance to healthy lifestyle program including physical activity as the older patients are the hardest to involve in physical activity programs. Future studies and ethical groups should focus on ethical and design issues regarding the large portion of institutionalized old patients who often do not consent to participate in interventional studies.
We found that taking care of a pet was found interesting by more than 60% of our surveyed population, yet, people with higher educational level and described as other cases (no dementia or cognitive impairment) were the less interested by petting animals compared to their counterparts with lower educational background. In a recent study, taking care of a pet was found to induce positive psychosocial benefits in a population of non-demented institutionalized old adults with primary education level [21]. As frequently seen in nursing homes, pets are used independently of their ecological potential benefits. As a limited number of individuals may be strongly motivated by the presence of an animal, the use of such “therapy” should be better supervised as interest may vary depending on the species or the animal category. This potential mismatch between animal and interests of old institutionalized adults might bring attention the recent rapid expansion of robotic pets as interventional tools for dementia patients [22]. Though such approaches may be yield some psychosocial benefits, a better description of the patient’s interest is awaited to quantify how pet therapy can improve general or psychological health from institutionalized old adults.
For intimate and emotional activities such as kissing we found that participants with dementia had significantly less interest in kissing than their counterpart designed as other cases. In clinical practice it is often reported by careers that hugs and kisses are found to reduce fear and behavioural disturbances of some patients with dementia. Interestingly, the published data covering this issue are scarce and inconsistent.
The mains limitations of this survey relied in the static figure of the population interests and the limited number of clinical characteristics of the population. Nonetheless the data we reported are consistent with recent works and data from interventional studies. Our strength resided in the representative sample of old adult residents thus giving a general tendency of the French institutionalized old adult interests. Furthermore, we believe that our observations strengthen the only related work in this domain by broadening the number of observations [12].
5. CONCLUSION
In summary, understanding individuals’ interests may guide intervention parameters to improve engagement and potential benefits; additionally, identifying parameters of lack of interest will not only add to the understanding of apathy syndrome but clear the way to tailored intervention for individuals who are often not included in interventional studies.
6. ACKNOWLEDGEMENTS
This study was supported by a grant from the Fondation de Coopération Scientifique, Plan Alzheimer 2008 - 2012, and by the IA and ARMEP association.
![]()
![]()
REFERENCES
- Marin, R.S. (1990) Differential diagnosis and classification of apathy. The American Journal of Psychiatry, 147, 22-30.
- Robert, P., Berr, C., Volteau, M., et al. (2008) Importance of lack of interest in patients with mild cognitive impairment. The American Journal of Geriatric Psychiatry, 16, 770-776.
- Cohen-Mansfield, J., Marx, M.S., Dakheel-Ali, M., Regier, N.G. and Thein, K. (2010) Can persons with dementia be engaged with stimuli? The American Journal of Geriatric Psychiatry, 18, 351-362.
- Dechamps, A., Diolez, P., Thiaudiere, E., et al. (2010) Effects of exercise programs to prevent decline in healthrelated quality of life in highly deconditioned institutionalized elderly persons: A randomized controlled trial. Archives of Internal Medicine, 170, 162-169. doi:10.1001/archinternmed.2009.489
- Cohen-Mansfield, J., Dakheel-Ali, M. and Marx, M.S. (2009) Engagement in persons with dementia: The concept and its measurement. The American Journal of Geriatric Psychiatry, 17, 299-307.
- Dechamps, A., Alban, R., Jen, J., Decamps, A., Traissac, T. and Dehail, P. (2010) Individualized Cognition-Action intervention to prevent behavioral disturbances and functional decline in institutionalized older adults: A randomized pilot trial. International Journal of Geriatric Psychiatry, 25, 850-860. doi:10.1002/gps.2427
- Dechamps, A., Jutand, M.A., Onifade, C., Richard-Harston, S. and Bourdel-Marchasson, I. (2008) Co-occurrence of neuropsychiatric syndromes in demented and psychotic institutionalized elderly. International Journal of Geriatric Psychiatry, 23, 1182-1190. doi:10.1002/gps.2052
- Ishii, S., Weintraub, N. and Mervis, J.R. (2009) Apathy: A common psychiatric syndrome in the elderly. Journal of the American Medical Directors Association, 10, 381- 393. doi:10.1016/j.jamda.2009.03.007
- Deudon, A., Maubourguet, N., Gervais, X., et al. (2009) Non-pharmacological management of behavioural symptoms in nursing homes. International Journal of Geriatric Psychiatry, 24, 1386-1395. doi:10.1002/gps.2275
- Vernooij-Dassen, M., Vasse, E., Zuidema, S., CohenMansfield, J. and Moyle, W. (2010) Psychosocial interventions for dementia patients in long-term care. International Psychogeriatrics, 22, 1121-1128.
- Cohen-Mansfield, J., Thein, K., Dakheel-Ali, M. and Marx, M.S. (2010) The underlying meaning of stimuli: Impact on engagement of persons with dementia. Psychiatry Research, 177, 216-222. doi:10.1016/j.psychres.2009.02.010
- Sharp, E.S., Reynolds, C.A., Pedersen, N.L. and Gatz, M. (2010) Cognitive engagement and cognitive aging: Is openness protective? Psychology and Aging, 25, 60-73. doi:10.1037/a0018748
- Le Duff, N., Gonfrier, S., Lafay, P., Texier, P., Schuck, S., Padrier, C. and Robert, Ph. (2010) The 2008-2012 French Alzheimer plan. Description of the Alzheimer Information System (AIS) and first results. Revue de Gériatrie, 35, 575-585.
- Dechamps, A., Fasotti, L., Jungheim, J., Leone, E., Dood, E., Allioux, A., et al. (2011) Effects of different learning methods for instrumental activities of daily living in patients with Alzheimer’s dementia: A pilot study. American Journal of Alzheimer’s Disease and Other Dementias, 26, 273-281. doi:10.1177/1533317511404394
- Volkow, N.D., Logan, J., Fowler, J.S., Wang, G.J., Gur, R.C., Wong, C., et al. (2000) Association between agerelated decline in brain dopamine activity and impairment in frontal and cingulate metabolism. The American Journal of Psychiatry, 157, 75-80.
- Crabtree, S. (2010) Gallup global report. http://www.gallup.com/poll/142727/religiosity-highest-world-poorest-nations/default.aspx
- Koenig, H.G. (2004) Religion, spirituality, and medicine: research findings and implications for clinical practice. Southern Medical Journal, 97, 1194-1200. doi:10.1097/01.SMJ.0000146489.21837.CE
- Dunn, K.S. and Horgas, A.L. (2004) Religious and nonreligious coping in older adults experiencing chronic pain. Pain Management Nursing, 5, 19-28.
- Rippentrop, E.A., Altmaier, E.M., Chen, J.J., Found, E.M. and Keffala, V.J. (2005) The relationship between religion/spirituality and physical health, mental health, and pain in a chronic pain population. Pain, 116, 311-321. doi:10.1016/j.pain.2005.05.008
- Paivi, M., Mirja, H. and Terttu, P. (2010) Changes in physical activity involvement and attitude to physical activity in a 16-year follow-up study among the elderly. Journal of Aging Research, 2010, 174290.
- Colombo, G., Buono, M.D., Smania, K., Raviola, R. and De Leo, D. (2006) Pet therapy and institutionalized elderly: A study on 144 cognitively unimpaired subjects. Archives of Gerontology and Geriatrics, 42, 207-216. doi:10.1016/j.archger.2005.06.011
- Shibata, T. and Wada, K. (2011) Robot therapy: A new approach for mental healthcare of the elderly—A minireview. Gerontology, 57, 378-386. doi:10.1159/000319015

