Open Journal of Gastroenterology
Vol.3 No.2(2013), Article ID:31437,2 pages DOI:10.4236/ojgas.2013.32014
Transhepatic percutaneous endoscopic gastrostomy*
![]()
Oncology Unit, ICCP, Pavia, Italy
Email: #guidopoggi64@gmail.com
Copyright © 2013 Guido Poggi et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received 22 January 2013; revised 18 March 2013; accepted 28 April 2013
Keywords: PEG; PEG Complications; Liver Injury
ABSTRACT
We describe the case of a hepatic injury after the insertion of a PEG. In a cirrhotic woman affected by a locally advanced cancer of the pharynx, the PEG tube was inserted through the edge of the left lobe of the liver. The patient was treated with a conservative approach by managing abdominal pain and the PEG was removed after 4 months without complication. Hepatic injury is a rare complication of PEG placement; in order to avoid it, PEG tube should be inserted to the left of the abdominal midline and the lower edge of the liver should be defined by palpation; in cirrhotic patients, where left hepatic lobe hypertrophy is common, ultrasound guidance could have been appropriate.
1. CASE REPORT
A 56-year-old woman with a medical history of alcoholic cirrhosis was hospitalized to start a combined treatment of chemo-radiotherapy for a locally advanced cancer of the pharynx. In view of the presumed loco-regional toxicity a percutaneous endoscopic gastrostomy (PEG) was planned before starting the treatment in order to preserve enteral food intake. A few hours following the procedure, the patient complained of a progressively worsening abdominal pain. An abdominal ultrasound examination and contrast-enhanced abdominal CT found that the PEG tube had been inserted through the edge of the left lobe of the liver (Figures 1 and 2, white arrows), while the bumper had been correctly placed in the gastric cavity (Figures 1 and 2, red arrows). Blood tests showed leukocytosis and elevated liver transaminases which had been normal on admission. The pain increased progressively and was exacerbated with movements. The patient was started on
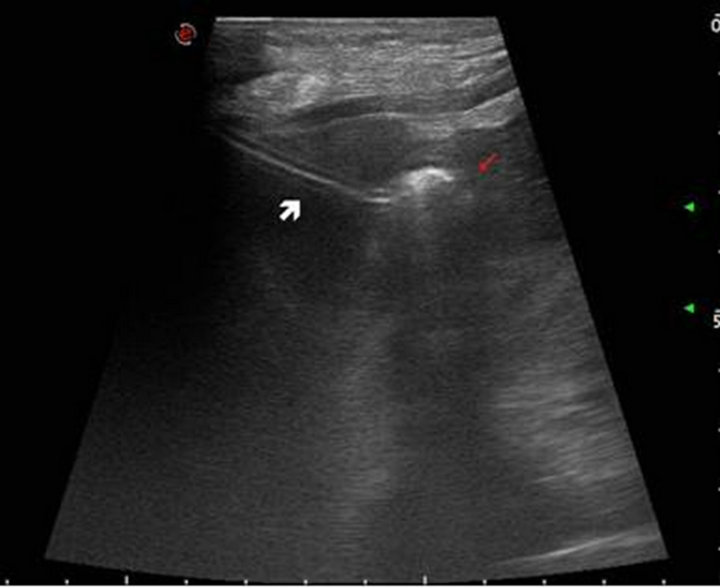
Figure 1. Abdominal ultrasound examination shows that the PEG tube is inserted through the edge of the left lobe of the liver (white arrow) while the bumper is correctly placed in the gastric cavity (red arrow).
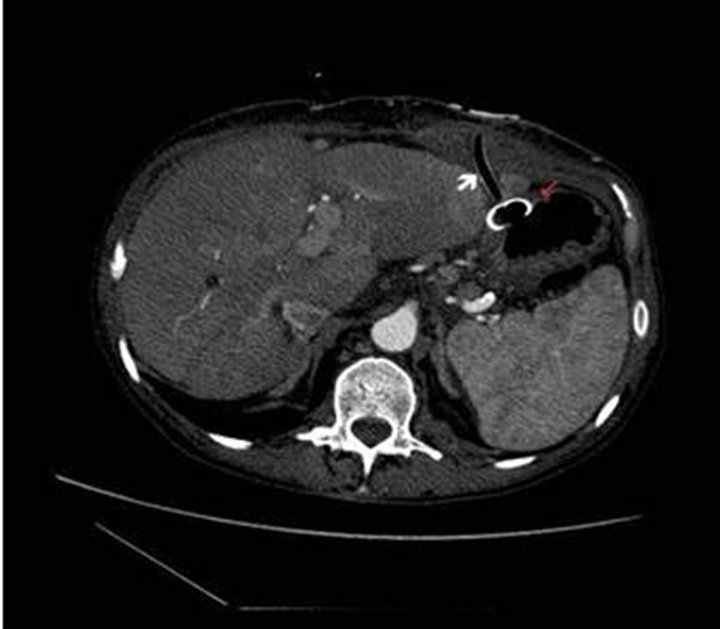
Figure 2. Contrast-enhanced abdominal CT confirms the penetration of the PEG tube through the liver (white arrow) and the placement of the bumper in the gastric cavity (red arrow).
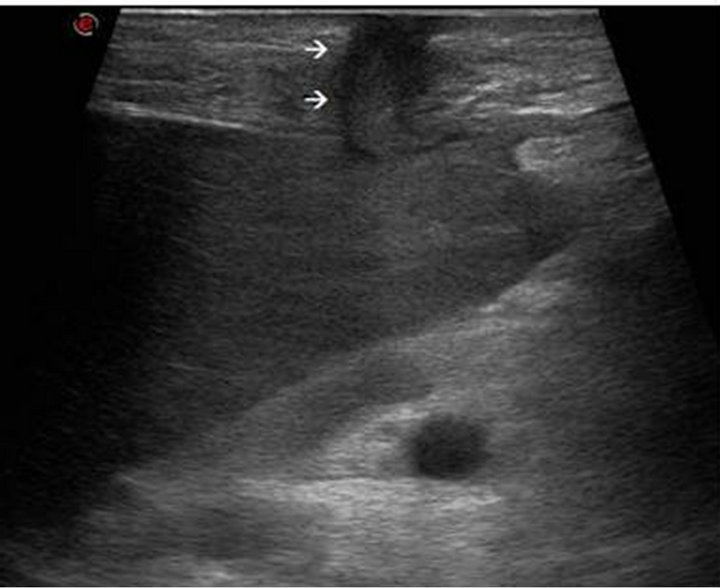
Figure 3. Ultrasound examination shows that tissues around the PEG-tube formed a gastro-cutaneous fistula crossing the liver (arrows).
broad-spectrum antibiotic therapy and opioids with complete resolution of pain in a few days. During chemoradiotherapy enteral nutrition was started through the PEG without any problems. After 4 months of therapy the patient obtained complete response of the oncologic disease and the PEG was endoscopically removed without any complications
2. DISCUSSION
PEG is the modality of choice for long-term enteral access for patients who are unable to maintain sufficient oral intake. Contraindications to PEG placement include pharyngeal or esophageal obstruction, major coagulopathy, abdominal wall abnormalities and the presence of prior abdominal surgery involving stomach and splenic flexure of the colon. Although generally safe, PEG placement can be associated with many potential complications like pneumoperitoneum, entero-cutaneous fistula, small bowel or colon injury, splenic or hepatic injury, intra or retro-peritoneal bleeding and abdominal wall bleeding [1].
Hepatic injury is a rare complication; in Literature there are few cases and most of them were treated with a conservative approach, based on clinical observation and abdominal pain management [2,3]. This complication can be avoided by using a correct technique: the liver should be palpated before the procedure and the tube insertion site should generally be to the left of the abdominal midline and verified with transillumination.
In our patient, transillumination was carried out properly and the tube was inserted without difficulty. It remains unclear how the liver parenchyma was perforated. Considering the presence of hepatomegaly, ultrasound guidance during the procedure could have been appropriate. Because of the absence of hemorrhage or major liver injury, we treated the patient with a conservative approach. Tissues around the PEG-tube formed a gastro-cutaneous fistula crossing the liver (Figure 3; arrows) that prevented extravasation of gastric contents and air into the peritoneal cavity and allowed the removal of PEG-tube without any complications.
In conclusion, transhepatic PEG placement is a rare, but potentially life-threatening complication; left hepatic lobe hypertrophy is common to be found in cirrhotic patients which means ultrasound guidance could have been appropriate.
REFERENCES
- Schrag, S.P., Sharma, R., Jaik, N.P., et al. (2007) Complications related to percutaneous endoscopic gastrostomy (PEG) tubes. A comprehensive clinical review. Journal of Gastrointestinal and Liver Diseases, 16, 407-418.
- Burke, D.T. and Geller, A.I. (2009) Peritonitis secondary to the migration of a trans-hepatically-placed percutaneous endoscopic gastrostomy tube: A case report. Archives of Physical Medicine and Rehabilitation, 90, 354-357. doi:10.1016/j.apmr.2008.06.038
- Gubler, C., Wildi, S.M. and Bauerfeind, P. (2005) Liver injury during PEG tube placement: Report of two cases. Gastrointestinal Endoscopy, 61, 346-348. doi:10.1016/S0016-5107(04)02584-2
NOTES
*No author has conflict of interest to disclose. The study did not have any financial support.
#Corresponding author.

