Open Journal of Stomatology
Vol.06 No.11(2016), Article ID:71756,17 pages
10.4236/ojst.2016.611027
Reconsidering Co-Morbid Traits in Explanatory Models of High Dental Anxiety Using a Comparison of Psychiatric and Normal Patient Samples
Rod Moore1*, Christina Gundlev Jensen1, Line Bæk Andersen1, Inger Brødsgaard2
1Dental Anxiety Research & Treatment Center, Department of Dentistry, Aarhus University, Aarhus, Denmark
2Psychiatric Hospital in Aarhus/Risskov, Aarhus University, Aarhus, Denmark

Copyright © 2016 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY 4.0).
http://creativecommons.org/licenses/by/4.0/



Received: September 28, 2016; Accepted: October 30, 2016; Published: November 3, 2016
ABSTRACT
Explanatory models of co-morbid traits related to dental anxiety (DA) as described in the literature were tested and relative strengths analyzed in two groups of Danish adults, one with psychiatric diagnoses (n = 108) and the other healthy incoming patients at a large dental school teaching clinic (n = 151). Dental Anxiety Scale (DAS) and self-report measures representing three co-morbidity explanatory models, 1) presence of other fears; 2) anxiety sensitivity and 3) feelings of vulnerability specific to dental treatment, were collected in subscales of a 53-item questionnaire. Other items identified gender, age, education, income, avoidance behavior and dental symptoms. Frequency, chi-square, odds ratio and logistic regression analyses were performed. Results: All individuals with high DA (DAS > 13) regardless of group, demonstrated significant differences in avoidance of treatment (>2 yr.) versus lower or no anxiety. Patients with psychiatric diagnoses were three times more likely to have high DA and nearly two times more likely to have avoided dental treatment >2 yr.; 25.9% reported extreme DA, compared to 9.3% of controls. Models of high general fear levels, predisposing anxiety sensitivity and vulnerability all demonstrated significant and strong association with intensity of dental anxiety in bivariate analyses. Feelings of vulnerability were the strongest predictor of DAS high anxiety, according to logistic regression analyses. Conclusion: Co-morbidity explanatory models as represented in present trait measures appear not to be competitive, but rather explain different aspects of a vulnerability model in high dental anxiety. Higher incidence of DA and treatment avoidance in psychiatric patients requires special attention.
Keywords:
Dental Anxiety, Psychiatry, Case Comparison, Co-Morbidity, Personality Traits

1. Introduction
In the prevalence of common fears, only fear of snakes, heights, physical injuries, storms and flying have been reported more frequently than dental fear [1] [2] [3] . In a Dutch epidemiological study from 2009 [3] , dental phobia was the most common phobia (3.7%), followed by heights (3.1%) and spiders (2.7%). Fear of dental treatment was associated with female gender, rated as more severe than any other fear, and was most strongly associated with intrusive re-experiencing, compared to other phobias [3] [4] .
Dental anxiety (DA) is known as one of the most frequent reasons for avoidance of dental care and deteriorating oral health including tooth decay, periodontal disease, tooth loss and complaints of dental problems, such as toothache, difficulty chewing and bleeding gums as shown in US [5] [6] , Danish [7] [8] , Swedish [9] , and Dutch [10] studies. High DA, or in particular phobia (odontophobia, or OP) [11] ) according to DSM criteria, is a mentally handicapping or disabling type of anxiety because of its impact on functional aspects of life, such as lack of sleep, difficulty eating and work loss due to painful symptoms [7] [8] [12] and quality of life can be affected [13] . Many odontophobics hide their teeth and mouth in their daily social routine, affecting their self- image and social life [14] .
Further evidence of compromised general mental health for persons with high DA can also be inferred from studies in which successful completion of cognitive behavioral therapy for DA in patients having co-morbid mental disorders before therapy have also shown significant improvement in these disorders after therapy [13] [15] [16] . A few studies have reported on incidence of co-morbid psychological disorders in people with high DA. Roy-Byrne et al. [17] were the first to conduct a complex psychological diagnostic evaluation, using DSM-III psychiatric criteria in patients with DA. They found at least one other psychiatric disorder in 42% of Ss. A representative birth cohort study from New Zealand [18] confirmed the frequent presence of co-morbid mental disorders in participants with high DA and found co-morbid disorders in 55% more participants than in those without DA. These studies did not relate diagnostic differences to treatment outcome, but a study by Kvale et al. [16] assessed DA via DSM diagnoses and outcome for a clinical sample of DA patients. Patients with specific phobia required significantly more therapeutic time than those with no psychiatric diagnoses. Patients with multiple DSM-IV diagnoses reported significantly more severe anxiety at all treatment steps, including one-year follow-up compared to patients with no co-morbid diagnosis. Although the results confirmed previous findings regarding difficulty treating DA patients with multiple phobia [13] [15] [19] , this was the first prospective study to reveal differences in treatment outcome by psychiatric diagnoses.
Thus, the literature spanning more than 40 years suggests that 1) high DA is a remarkably severe, stable and highly prevalent dysfunctional condition with long duration, if not treated and that 2) high DA and phobia appear to have unique characteristics and explanatory models, given varying degrees of symbiotic interactions with co-morbidity reported in the literature.
From the awareness that co-morbidity is often common in DA, researchers have reported that people with psychiatric disorders are significantly more prone to poor oral health [20] [21] [22] [23] [24] , but there was little or no validated testing for intensity of DA or avoidance. Even though co-morbidity would seem to be a logical hypothesis in studying DA among psychiatric patients, only a German study by Lenk et al. [21] used standardized psychometric scales [25] to reflect on DA and avoidance behavior among 212 psychiatric patients compared with 95 healthy controls. Lenk et al. [21] found that 31% of these psychiatric patients suffered from pathologically severe DA. Only 4.2% of the healthy controls had high DA. 82% of all high DA Ss had avoided treatment to some degree. Certain types of mental disorder were especially highly associated with DA: anxiety disorders (relative risk (RR) 7.4) and depressive disorders (RR = 4.9). PTSD patients were most frequently affected (42%) (RR = 10.0).
Thus, traumatic experiences, presence of other anxiety or fears and mood disorders were often co-variant with high DA in Lenk et al.’s [21] psychiatric patient sampling. If one considers the contrast and comparability of DA co-morbidity in psychiatric vs healthy patients, one could argue that they lend themselves to theoretical discussions about possible co-morbidity explanatory models influencing DA phenomena. Some explanatory models involved in DA formation described in the literature are Learning theory [26] [27] [28] , Expectancy theory/Anxiety Sensitization [29] [30] [31] , Preparedness theory/Generalization of fears [32] and Vulnerability modelling [33] [34] [35] .
Learning theory purports that traumatic conditioning reinforces anxiety responses as “latent inhibition” [26] [27] [28] . DA is most often described as trait anxiety that reflects reinforceable conditioning of behavior whether generated by classical stimuli like pain or by repetitive negative dentist behaviors. Dental trait anxiety thus refers to a personality characteristic of persons who exhibit relatively stable anxiety reactions which include worrying and other expectational apprehensions, e.g. anxious anticipation of dental drilling or negative dentist behavior leads to avoidance of dental work. Thus, multiple clinical and epidemiological studies over many years concur that high trait DA almost always is involved some kind of traumatic dental experience [6] [7] [8] [9] [26] and as such is assumed to be a common condition for most people suffering from high DA.
Since the focus of the present study is on co-morbid psychological factors and personality traits related to DA, only the following explanatory models were investigated, since less is known about specific effects of co-morbid factors than traumatic conditioning in relation to DA.
Anxiety sensitivity―Reiss and colleagues [30] [31] and Taylor et al. [29] [36] distinguish a concept of anxiety sensitivity from trait anxiety by noting that, whereas trait anxiety predicts future anxiety generally, anxiety sensitivity predicts future fear specific to anxiety sensations based on expected beliefs that these sensations have harmful consequences in themselves. Anxiety sensitivity is also relevant to dental anxiety, since the fear of being anxious is often a part of the psychological profile of persons with extreme dental anxiety or phobia [11] .
Preparedness theory posits that there can be a generalization of fears about, and often avoidance of, several specific events or situations in a person’s life that indicate a tendency to experience fear when confronted with those or perceptually similar events or situations, e.g. other fears with dental fears [37] . Several larger studies have concluded that co-morbid other fears can impact significantly on DA and usually have gender related varying estimates of influence [2] [7] [38] [39] .
Vulnerability―Feelings of vulnerability related to anxiety traits have been characterized and studied as feelings of lack of control, unpredictability, danger and disgust according to the Cognitive Vulnerability Model described by Armfield [33] . A stimulus automatically and unconsciously triggers its respective vulnerability schema unique to each person. The schema includes perceptions of the uncontrollability and unpredictability of the stimulus-response outcome, which may relate to danger and/or disgust. Cognitive schema content is learned by individuals and is moderated by personality differences. With activation of a vulnerability schema, two parallel processes occur: 1) rapid automatic affective reaction and immediate fear responses and 2) a relatively slower cognitive appraisal, which incorporates various other personality colored evaluations, which may amplify the immediate fear response. An interpretation of the outcome feeds back into the vulnerability schema, reinforcing the moderating cognitive processes. As an example, in a large epidemiological Australian DA study [34] , Armfield et al. showed that people who perceived sitting in a dental chair as highly controllable, highly predictable and highly safe rarely had moderate to extreme DA. Approximately 50% or more of people who regarded the dental environment as being either highly uncontrollable, highly unpredictable or highly dangerous had high dental anxiety [34] .
To the authors’ knowledge, the possible co-morbidity trait explanatory models of generalization of fears, anxiety sensitivity and vulnerability for DA have not been examined in the same clinical comparison study. Theoretical comparisons about formation of high DA or OP in the form of measures representing these models could illuminate relative influence of contributing factors toward a better understanding of causality.
Present study initially aimed to investigate differences in the frequency and intensity of dental anxiety in individuals with diagnosed psychiatric disorders compared with healthy controls and to what degree they differ in avoidance of dental care and symptomatology. Then, as the main aim of the study, it was hypothesized that general anxiety, anxiety sensitivity and feelings of vulnerability would be significantly greater for psychiatric patients with high dental anxiety than for controls. Relative influence of gender, age, education and income on DA and these co-morbidity factors were also explored.
2. Materials and Methods
The project was conducted as a written survey in Danish which examined, among other things, subjects’ relationships to dentists and dental treatment based on a convenience sample. The target group for the study were subjects with mental disorders diagnosed by a doctor or psychiatrist who were actively recruited among inpatients at Horsens and Aarhus psychiatric wards (east Jutland), patients in local psychiatric ambulatory services in Aarhus and Hjørring (north Jutland), and among incoming dental patients at the Aarhus University School of Dentistry with psychiatric diagnoses. This group comprised 108 people, hereafter called Psychiatric Patient Group “PSYG”, out of a total of 259 subjects (Ss) who were surveyed from October through December 2013.
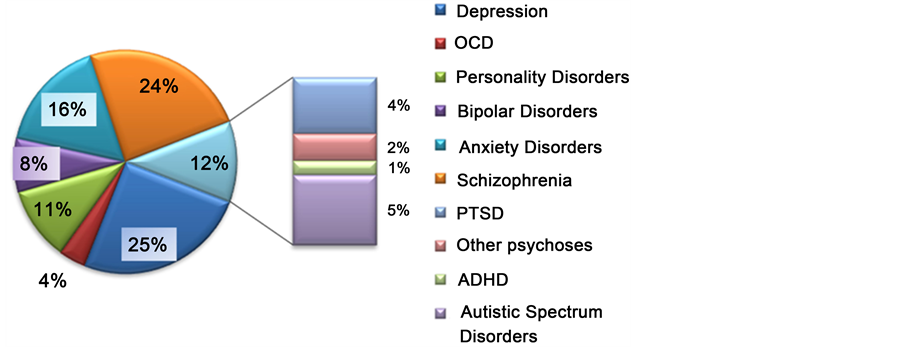
Individuals in PSYG were categorized by their psychiatric diagnoses to describe the nature of the sample. The Ss that had multiple diagnoses were categorized by their primary diagnosis (chief reason for clinical treatment seeking). There were ten primary diagnoses ranked by frequency: depression (25%), schizophrenia (24%), anxiety disorders (16%), personality disorders (11%), bipolar disorder (8%), autistic spectrum disorders other than ADHD (5%), obsessive compulsive disorder (4%), post-traumatic stress disorder (4%), psychoses other than schizophrenia (2%), and ADHD (1%). The distribution of diagnoses are shown in graph form in Figure 1.
The healthy Control Group (CTRLG) for comparison was recruited among consecutive incoming new patients from Aarhus University School of Dentistry teaching clinic. These patients were screened for self-reports of psychiatric symptoms and if there had been a prior psychiatric diagnosis made by a doctor or psychiatrist, individuals with diagnoses were excluded from the comparison group and instead were included in the PSYG. The CTRLG consisted of a total of 151 Ss.
All potential subjects from both groups were contacted by one of the authors or a well-oriented research assistant using a standard recruitment flyer in which the purpose of the project was explained. No statistics were possible for potential subjects that declined participation. Verbal and written consent were then obtained. Each participant was given a questionnaire consisting of 53 questions, which took about 10 minutes to complete. Help was always available regarding questions about the study.
2.1. Content of the Questionnaire
The first part of the questionnaire consisted of 13 questions that aimed to compare
Figure 1. Percentage distribution of psychiatric diagnoses in PSYG (n = 108).
characteristics including Ss’s age, gender, taxable income, educational level, last dental treatment, regularity of dental attendance, pain symptoms, dental problems as well as Ss’s self-reported mental status, psychiatric diagnosis and duration of diagnosed illness. The control group patients were presented the same questions as psychiatric patients regarding mental health and eventual psychiatric disorders as diagnosed by a physician or psychiatrist. Authors were present for eventual questions while all psychiatric patients filled out the questionnaires.
Ss’s anxiety about dentistry, the dependent variable, was measured using the well- documented, Dental Anxiety Scale (DAS) [40] [41] . This ordinal scale included questions about how it would feel at the thought of “going to the dentist tomorrow”, “to wait in the waiting room”, “to sit in the dentist’s chair while the dentist prepares the drill” and “to have a tooth cleaning”. DAS has a maximum score of 20, which indicates extreme anxiety and a minimum of 4 indicating no anxiety. Previous studies have determined that DAS has high validity and reliability as a measure of intensity of dental anxiety [41] . The Danish general population has a mean score of 7.5 (SD = 3.1) [11] Cutoffs for categories of intensity of dental anxiety were determined by reference to the literature on DAS in epidemiological studies [7] [41] . For analyses, “high dental anxiety” was the dichotomous DAS cutoff >13 vs. <13, [41] while DAS > 15 indicated “extreme or phobic dental anxiety”, DAS 12 - 14 was “moderate dental anxiety” and DAS <11 was “little or no anxiety” as in a previous Danish epidemiological study [7] .
As described above, the literature indicates an association between intensity of dental trait anxiety and a person’s general fearfulness, anxiety sensitivity and vulnerability, thus the study population was analyzed using ordinally scaled measures about general fear levels, anxiety sensitivity and vulnerability tests described below.
Anxiety Sensitivity Index (ASI) [30] [42] is 16 questions that assess a person’s thoughts about the social and somatic consequences of anxiety symptoms. ASI is a well- tested index with high validity that reveals a person’s fear of becoming anxious. Items measured degree of worry about “not appearing nervous”, “going crazy”, “trembling”, “feeling faint”, “staying in control of emotions”, “rapid heartbeat”, “stomach growling”, “nausea”, “having a heart attack”, “shortness of breath”, “becoming seriously ill”, “unable to keep my mind on a task”, “people can see me shaking”, “unusual body sensations”, “nervousness that can lead to mental illness” and “when I am nervous”. The questions were scored on an ordinal scale of 1 to 5, where 1 was “very little” and 5 was “really much”.
Generalization of fears-Ten questions were taken from the well documented Geer’s Fear Scale (GFS) [38] [43] a shortened FSS-II scale that considered general aspects of Ss’s fears and phobias. The items were about fears of injection needles, blood, heights, enclosed spaces, thunderstorms, snakes, insects sticking, social life, pain and death. Answers were ordinally ranked with values from 1 to 5, where 1 was “not afraid” and 5 was “terrified”.
Vulnerability-Feelings of vulnerability [34] [35] in the context of dental treatment were measured with ten items: “I’m constantly thinking that I need to go to the dentist.”, “I am worried that my teeth will fall out.”, “I feel silly that I’m so afraid of dental treatment.”, “I hide my fear of dental treatment from other people.”, ”I am reluctant to meet new people due to the condition of my teeth.” and “If I said it hurts, I do not think the dentist would stop and do something about it.”, “When I sit in the dentist’s chair, I do not think I can allow myself to interrupt treatment, even though I need a break.”, “I do not like to ask questions of the dentist.”, “I’m worried that something unpleasant will happen at the dentist, that I might not be able to prevent.”, “I do not feel I have control over what happens to me in the dentist's chair.” The first two were about loss of personal integrity, the next three about embarrassment or social anxiety [11] and the final five were about lack of control [44] and dangerousness in dental treatment situations [34] [35] . The answers were ordinally scaled with values from 1 to 5, where 1 = disagree and 5 = agree.
2.2. Statistical Methods and Data Analysis
The DAS scale was the dependent variable and other factors from the other questions and scales represent the independent variables. Frequencies of DAS scores in the two groups were first compared for differences in distribution. Given significant differences in the distribution of group DAS scores, association analyses were then conducted to attempt to explain variation by factors other than SS’s psychiatric diagnosis.Thus, questions and scales were used to build explanatory models that could contribute to better understanding of high DA among the two populations.
Reliability was assessed on subscales using Cronbach’s alpha. Validity was assessed using Spearman’s correlations, response frequencies and chi-square tests.
Distribution and association analyzes were accomplished using tables of percentage distributions including mean and median distributions, Mann-Whitney and Student’s t-tests for independent samples, Spearman’s rho correlations, 2 × 2 tables (Chi2-test with continuity correction and odds ratios) and Nonlinear Logistic Regression with Hosmer-Lemeshow estimates of fit and Nagelkirke’s R2 estimate of explained variance, all of which were computed using statistical package SPSS 21, where statistical significance was set at P ≤ 0.05. Dichotomous variable cutoffs were chosen on the basis of approximately one standard deviation over the mean score for each of the variables for the control group CTRLG, unless otherwise described or rationalized in the Results.
3. Results
3.1. Gender and Age
There was a difference in gender distribution between the two groups, with a higher proportion of men in CTRLG and a higher proportion of women in PSYG, although these were not statistically significant (Table 1). Mean age for PSYG was (41.6 yr, SD = 13.8) and was significantly lower than CTRLG (45.3 yr, SD = 16.0). Distribution percentages by age groups are tabled for convenience.
Women in the PSYG had significantly higher scores than men only on GFS (U = 1030; P = 0.017), although ASI approached significance (U = 1173; P = 0.13). Women
Table 1. Percent distributions of gender and age in the psychiatric patient group (PSYG) and the healthy control group (CTRLG).
Chi2 = 1.26; df = 1; PGender = 0.26 t = −2.01, df = 249, PAge =0.04
in CTRLG scored higher than men on DAS (U = 2195; P = 0.02) and GFS (U = 1613.5; P < 0.001).
3.2. Education and Income
There were significant differences between groups by education and income (Table 2). PSYG had a greater proportion with only a primary school education compared with CTRLG. CTRLG had a greater proportion of people with higher education. The distribution of people with technical training or high school education is more similar in the two groups. Regarding income, the proportion of people in PSYG who had an annual income of more than 240,000 kr. (10.3%) is significantly less than the CTRLG, where the distribution of income is more even (6.5 DKK = ca. 1 USD).
3.3. Avoidance of Treatment and Dental Anxiety
Avoiding regular examinations by the dentist for two years or more was not statistically significantly different between the two groups Chi2 = 5.72; df = 1; P =0.17. However PSYG Ss were almost two times (OR = 1.97 95% CI = 1.16 - 3.34) more likely to avoid treatment and were over three times more likely to have high DAS scores (>13) than CTRLG Ss Chi2 = 16.33; df = 1; P =0.000 OR = 3.10; 95% CI = 1.80 - 5.27.
3.4. Dental Symptoms and Pain
Report of dental problems by PSYG and CTRLG approached significant differences (Chi2 = 5.69; df = 2; P =0.06) but fell short. Reported pain in the last six months (Chi2 = 2.54; df = 1; P =0.11, OR = 1.55 95% CI = 0.94 - 2.54) and pain report at the time of the survey (Chi2 = 1.62; df = 2; P = 0.20, OR = 1.68 95% CI = 0.83 - 3.42) also were not statistically significant between groups, although PSYG Ss were over 1 ½ times more likely to report pain symptoms.
3.5. Dental Anxiety Scale Distributions and Dependent Variable Analyses
DAS scores were divided into 5 categories to facilitate understanding of dental anxiety characteristics (Table 3). CTRLG Ss had a mean score consistent with the general Danish population. There is a significant difference between PSYG and CTRLG in DAS scores (Table 3). Table 3 also shows that 25.9% of PSYG had extreme to phobic dental anxiety (DAS ≥ 15), and 22.1% had intense to moderate anxiety (DAS = 12 - 14). By
Table 2. Percent distributions of educational training and taxable income pr. year in psychiatric patients (PSYG) and healthy controls (CTRLG).
Chi2 = 24.0, df = 3; PEducation = 0.02 Chi2 = 24.0, df = 3; PIncome < 0.001.
Table 3. Percent distribution of clinical DAS categories and over-all scores for psychiatric patient group (PSYG) and for healthy control group (CTRLG).
t-test = 4.5; PDAS < 0.001.
comparison, only 9.3% of CTRLG had extreme to phobic anxiety, and 13.2% had intense to moderate anxiety. By contrast, 77.5% of CTRLG had no to little fear of dentistry (DAS ≤ 11), whereas only 52% of PSYG have the same low intensity of anxiety.
3.6. Feelings of Vulnerability, General Fear or Anxiety Sensitivity
There was a significant difference in median scores between the group of people with a psychiatric diagnosis and the comparison group's scores in Vulnerability Scale, GFS and ASI (Table 4).
Spearman’s rho correlations between DAS scores and corresponding scores for Vulnerability, GFS and ASI were significant for both total population and for PSYG and CTRL (Table 5, next page). Correlations for GFS are weaker than vulnerability and anxiety sensitivity in association with DAS scores for PSYG, whereas in CTRLG anxiety sensitivity had the weakest correlation with DAS scores. For both groups, the vulnerability scale had highest correlation with DAS dental anxiety.
To further explore correlation results from Table 5, the associations between a high DAS score (≥13) or extreme DAS score (≥15) and were tested with high Vulnerability, GFS, and ASI in bivariate and logistic regression model analyses. High vulnerability in this context is defined as scores of 25 and above (VUL25), high GFS as scores of 25 or more (GFS25) and high ASI as scores of 30 or more (ASI30). Odds ratios (OR) for bivariate analyses in Table 6 (next page) show that PSYG had a tendency to have high DAS scores if they exhibited high vulnerability, general fear or anxiety sensitivity compared to CTRLG.
Logistic regression models for DAS ≥ 13 vs. DAS < 13 in each group were initially loaded with all theoretically relevant independent variables described in the bivariate and correlation analyses above for age, gender, education, income, vulnerability, general
Table 4. Medians, means and SD vulnerability, Geer’s fear scale and anxiety sensitivity index for psychiatric patient group (PSYG) and for healthy control group (CTRLG).
PVulnerability = 0.001 PGFS< 0.001 PASI < 0.001.
Table 5. Cronbach’s reliability for each test and spearman’s correlations between test of vulnerability, Geer’s fear scale and anxiety sensitivity index scores N = 259 and by the psychiatric patient group (PSYG) and the healthy control group (CTRLG).
*P < 0.001.
Table 6. DAS analyses of dichotomous variables for vulnerability, Geer’s Fear Scale and Anxiety Sensitivity Index in the Psychiatric Patient Group (PSYG) and the healthy Control Group (CTRLG). Some frequencies show less than the total number of Ss due to missing data.
*P < 0.001.
fears and anxiety sensitivity. Logistic regression analysis was accomplished by Backward Step Wald statistical elimination for each group. Final models thus reflect both best theoretical and statistically significant results and best fit as seen in Table 7 below.
4. Discussion
The main aim of the present study was to investigate co-morbidity explanatory models of high DA using two samples with contrasting psychological profiles, subjects with diagnosed psychiatric disorders compared to a group without diagnosed psychiatric disorders. Results revealed a significant difference in the intensity and qualities of dental
Table 7. Final logistic regression models DAS > 13 vs. DAS < 13 for Psychiatric Patients (PSYG) and Healthy Controls (CTRLG).
Coding of dichotomous variables: DAS13 (DAS > 13 vs. DAS < 13) 0 = low; 1 = high, AGE42: 0 = <42 yr; 1 => 42yr, GENDR F: 0 = men; 1 = women, Low EDU: 0 => grade school; 1 = grade school, VUL25 (Vulnerability): 0 = low; 1 = high, GFS25 (General Fear) 0 = low; 1 = high, ASI30 (Anxiety Sensitivity) 0 = low; 1 = high.
anxiety between these groups. Table 3 indicates that scores of CTRLG fall under the qualitative category of “little anxiety”, clinical intensity of DA when mean DAS scores are around 7 or 8 and thereby similar to the Danish adult population at large [7] . The mean dental anxiety level of the PSYG group in the present study however shifts to the qualitative category “some anxiety” on average (Table 3), which is a clinically meaningful difference. These results and explanatory associations with results follow after a discussion of sampling.
4.1. Sampling Discussions
The demographic variables of subjects in this study by group are not in all respects equivalent. PSYG had more women and significantly lower ages, lower income and lower education than CTRLG Ss in bivariate analyses. One must be careful not to assume generalizability of present results to the entire Danish adult population or to all psychiatric patients in Denmark, given the relatively small sample size and exclusion of some psychiatric diagnoses. Also, there was no clinical examination component to this study to assess oral or mental health of Ss. Only self-reported symptoms and treatment avoidance were used. Thus, current results should be interpreted with some caution.
However, even though there was a higher proportion of women in the psychiatric diagnosed group in this convenience sample, one can argue that this may likely be representative for this group of patients in Denmark, since some diagnoses are reported as frequently or more frequently in women than men [45] including depression, schizophrenia, anxiety and personality disorder diagnoses,the four most frequent of the 10 primary diagnoses in the present study. It should also be pointed out that present study diagnoses do not include drug abuse, a major male diagnostic category. Generally it is also known that women to a larger degree than men are less reluctant to reveal their psychological situation and seek treatment for mental illness. Additionally, women are reported to be more reactive than men under mental stress [45] . Some studies also indicate that this may be a reason for more frequent DA among women than men [11] . These important sample descriptives support potential reliability of a comparison of the present groups. The logistic analyses have also controlled for gender, age, education and income in the final logistic models and thus resulted in a nuanced comparative picture of dental anxiety characteristics with good fit for each of the two groups.
Avoidance of dental treatment and report of pain or dental problems by psychiatric patients was not significantly greater than for the control group in spite of that PSYG Ss were almost two times more likely to avoid treatment and were over three times more likely to have high DAS scores than CTRLG Ss. One caveat about CTRLG is that only dental treatment-seeking patients who initiated contact with the Aarhus university dental clinics were recruited into the study for control comparisons, thereby excluding individuals who may have been avoiding dental treatment and had higher anxiety levels that prevented them from seeking dental care. On the other hand, Aarhus University School of Dentistry has a reputation within the community for accepting anxious patients for treatment, since student dental care is more conducive to a slower tempo and educational-explanatory treatment. Psychiatric patients were, for the most part, not seeking dental care. However, percentages of dental symptoms and pain report in CTRLG appear similar to an epidemiological study of the general Danish adult population [7] and thus seem plausible as a normative comparison group.
4.2. Meaningfulness of the Study
Feelings of vulnerability have been characterized and studied as lack of control, unpredictability, danger and disgust according to the Cognitive Vulnerability Model described by Armfield [33] . In the present study, vulnerability was similarly characterized as lack of control and trust and experiences of embarrassment and dangerousness at the dentist. Results showed that perceived vulnerability was found to be the strongest predictor of high dental anxiety of all the independent variables tested for Ss both with and without a psychiatric diagnosis, also in logistic regression (LR) analyses. High vulnerability PSYG subjects were 22 times more likely (Table 7) to experience high DA, while high vulnerability CTLG subjects were 11.8 times more likely to have high DA. Therefore these results confirm Armfield et al. and Edmunds and Buchanan [34] [35] about the theoretical aspects of vulnerability that impact on fear of dentistry, for both subjects with and without psychiatric diagnoses, although the association was nearly twice as potent and three times as prevalent for Ss with psychiatric diagnoses.
Thus, clinicians need to be aware not only of their patients’ level and nature of their anxiety but also their perceptions of uncontrollability, unpredictability and dangerousness in the dental environment.
Geer’s Fear Scale was used in the study to measure the general fear level among Ss and is one of several factors known to be predictive of dental anxiety, especially in women [7] [38] [43] . General fear level can reveal the extent to which one views the world as dangerous and threatening or how the person processes situations such as in the dentist's chair, but a high GFS score alone is not synonymous with DA. Women in the PSYG had significantly higher scores than men only on GFS while women in CTRLG scored higher than men on both DAS and GFS, which is similar to the general Danish adult population [7] . In final LR models, a high GFS significantly predicted that CTLG subjects were three times more likely to have high DA. High GFS scores among PSYG were also nearly three times more likely to have high DA, but the relationship failed to reach significance (Table 7). Thus, it is apparent from Table 7 that associations between high DA and high GFS scores were not as strong as high vulnerability scores and high DA, but general fears contributed meaningfully to the final theoretical model and significantly so for patients without psychiatric diagnoses.
Subjects’ anxiety sensitivity was measured using ASI. One of the key predictive values of the concept of anxiety sensitivity is that it is a risk factor for developing panic attacks and other anxiety or phobic disorders [36] , which could include DA. Individuals with a high ASI are more likely to react more strongly to anxiety-provoking stimuli including the situation in the dentist’s chair. In the present study, it was expected that people with high ASI scores would be at greater risk of developing high DA. There were significant correlations between the intensity of DAS and ASI-scores, which is particularly strong among Ss with a psychiatric diagnosis compared to Ss without (Table 5, Table 6). Subjects with psychiatric diagnoses also had significantly higher ASI scores than healthy subjects (Table 5, Table 6). Although bivariate analyses showed that PSYG with high ASI had nearly four to six times greater probability to experience high DA compared to CTRLG, ASI did not figure in to the final best fit logistic regression explanatory models for high DA for either group. This seems apparent because of the overwhelming explanatory value of vulnerability and general fear especially with gender, as in the final LR models. Theoretically, it is known that general fear levels and anxiety sensitivity overlap [30] [36] . If one is afraid of being afraid, one is more likely to have a greater number of fears. It can be that conceptual nuances of the two were less meaningful for this sample, especially in the statistical elimination process of building final explanatory models.
Thus, the final logistic regression analytic models appear to indicate that there are similar yet separate components to consider when comparing the characteristics of high DA patients with psychiatric diagnoses and those without. Both groups require special strategies to decrease vulnerability by improving patient control in the dental clinical environment and this appears to be necessary even more frequently for dental anxiety patients with psychiatric diagnoses. Cognitive behavioral desensitization with slow, deliberate, step by step, non-obligatory self-confidence building experiences in the dental chair have always been a part of the therapeutic process for reducing high DA. The dental clinician’s ability to provide patients with an internal sense of social and procedural control with the use of task specific verbal contracts is of primary importance during this process. This appears to be especially so for the patient with exceptionally vulnerable feelings and differing degrees of anxiety sensitivity and other fears.
Empowering patients, in general, is a challenging task for dental personnel and requires more time assigned to individual dental treatment needs and more importantly an understanding of the mindset required in providing tolerant, patient, trustworthy care that will decrease patient feelings of vulnerability and effects of concomitant anxiety sensitivity and other fears. Thus, more training in optimal anxiety management for dental professionals may also be necessary, especially when they become involved with patients with psychiatric diagnoses.
5. Conclusions
Present study used a well-described convenience sample to assess the incidence of high DA in subjects with psychiatric diagnoses. A higher frequency of high DA was noted for subjects with diagnosed psychiatric disorders, compared to a group without diagnosed psychiatric disorders.
Results showed that the intensity of DA among subjects was associated with factors such as age, gender, education, income, feelings of vulnerability at the dentist, presence of other general fears and anxiety sensitivity. Strength of high DA associations with feelings of vulnerability, presence of other general fears and anxiety sensitivity were stronger for subjects with psychiatric diagnoses. In particular, feelings of vulnerability were concluded from LR analyses to be the strongest predictor of high DA for both groups, but especially for psychiatric patients. Thus, co-morbidity explanatory models as represented in present trait measures appear not to be competitive, but rather explain different aspects of a vulnerability model in dental anxiety. Since anxiety is known as one of the biggest reasons for the avoidance of dental treatment and degenerating oral health, this study provides valuable information about the need for increased awareness about the prevention and treatment of high dental anxiety, especially among patients with psychiatric diagnoses as a risk group. Present study findings also suggest that strategies for treatment of people with high dental anxiety require exceptional patience and attentiveness of the therapist to combat feelings of vulnerability.
Cite this paper
Moore, R., Jensen, C.G., Andersen, L.B. and Brødsgaard, I. (2016) Reconsidering Co-Morbid Traits in Explanatory Models of High Dental Anxiety Using a Comparison of Psychiatric and Normal Patient Samples. Open Journal of Stomatology, 6, 211-227. http://dx.doi.org/10.4236/ojst.2016.611027
References
- 1. Agras, S., Sylvester, D. and Oliveau, D. (1969) The Epidemiology of Common Fears and Phobia. Comprehensive Psychiatry, 10, 151-156.
http://dx.doi.org/10.1016/0010-440X(69)90022-4 - 2. Fiset, L., Milgrom, P., Weinstein, P. and Melnick, S. (1989) Common Fears and Their Relationship to Dental Fear and Utilization of the Dentists. Anesthesia Progress, 36, 258-264
- 3. Oosterink, F.M.D., de Jongh, A. and Hoogstraten, J. (2009) Prevalence of Dental Fear and Phobia Relative to Other Fear and Phobia Subtypes. European Journal of Oral Sciences, 117, 135-143.
http://dx.doi.org/10.1111/j.1600-0722.2008.00602.x - 4. Oosterink, F.M.D., de Jongh, A. and Aartman, I.H. (2009) Negative Events and Their Potential risk of Precipitating Pathological Forms of Dental Anxiety. Journal of Anxiety Disorders, 23, 451-457.
http://dx.doi.org/10.1016/j.janxdis.2008.09.002 - 5. Doerr, P.A., Lang, W.P., Nyquist, L.V. and Ronis, D.L. (1998) Factors Associated with Dental Anxiety. Journal of the American Dental Association, 129, 1111-1119.
http://dx.doi.org/10.14219/jada.archive.1998.0386 - 6. Milgrom, P., Fiset, L., Melnick, S. and Weinstein, P. (1988) The Prevalence and Practice Management Consequences of Dental Fear in a Major US City. Journal of the American Dental Association, 116, 641-647.
http://dx.doi.org/10.14219/jada.archive.1988.0030 - 7. Moore, R., Birn, H., Kirkegaard, E., Brødsgaard, I. and Scheutz, F. (1993) Prevalence and Characteristics of Dental Anxiety in Danish Adults. Community Dentistry and Oral Epidemiology, 21, 292-296.
http://dx.doi.org/10.1111/j.1600-0528.1993.tb00777.x - 8. Moore, R., Brødsgaard, I. and Birn, H. (1991) Manifestations, Acquisition and Diagnostic Categories of Dental Fear in a Self-Referred Population. Behaviour Research and Therapy, 29, 51-60.
http://dx.doi.org/10.1016/S0005-7967(09)80007-7 - 9. Hakeberg, M., Berggren, U. and Carlsson, S.G. (1992) Prevalence of Dental Anxiety in a Adult Population in a Major Urban Area in Sweden. Community Dentistry and Oral Epidemiology, 20, 97-101.
http://dx.doi.org/10.1111/j.1600-0528.1992.tb00686.x - 10. Stouthard, M.E. and Hoogstraten, J. (1990) Prevalence of Dental Anxiety in the Netherlands. Community Dentistry and Oral Epidemiology, 18, 139-142.
http://dx.doi.org/10.1111/j.1600-0528.1990.tb00039.x - 11. Moore, R. (2006) Psychosocial Aspects of Dental Anxiety and Clinical Pain Phenomena. Doctor of Odontology Dissertation, Fællestrykkeriet for Sundhedsvidenskab, Aarhus University, Aarhus.
http://dx.doi.org/10.13140/RG.2.1.4063.0248 - 12. Berggren, U. (1993) Psychosocial Effects Associated with Dental Fear in Adult Dental Patients with Avoidance Behaviours. Psychology & Health, 8, 185-196.
http://dx.doi.org/10.1080/08870449308403178 - 13. Berggren, U. and Carlsson, S.G. (1986) Qualitative and Quantitative Effects of Treatment for Dental Fear and Avoidance. Anesthesia Progress, 33, 9-13.
- 14. Moore, R., Brødsgaard, I. and Rosenberg, N. (2004) The Contribution of Embarrassment to Phobic Dental Anxiety: A Qualitative Research Study. BMC Psychiatry, 4, 10.
http://dx.doi.org/10.1186/1471-244x-4-10 - 15. Moore, R., Brødsgaard, I., Berggren, U. and Carlsson, S.G. (1991) Generalization of Effects of Dental Fear Treatment in a Self-Referred Population of Odontophobics. Journal of Behavior Therapy and Experimental Psychiatry, 22, 243-253.
http://dx.doi.org/10.1016/0005-7916(91)90040-C - 16. Kvale, G., Raadal, M., Vika, M., Johnsen, B. H., Skaret, E., Vatnelid, H. and Oiama, I. (2002) Treatment of Dental Anxiety Disorders. Outcome Related to DSM-IV Diagnoses. European Journal of Oral Sciences, 110, 69-74.
http://dx.doi.org/10.1034/j.1600-0722.2002.11204.x - 17. Roy-Byrne, P.P., Milgrom, P., Tay, K.-M., Weinstein, P. and Katon, W. (1994) Psychopathology and Psychiatric Diagnosis in Subjects with Dental Phobia. Journal of Anxiety Disorders, 8, 19-31.
http://dx.doi.org/10.1016/0887-6185(94)90020-5 - 18. Locker, D., Poulton, R. and Thomson, W.M. (2001) Psychological Disorders and Dental Anxiety in a Young Adult Population. Community Dentistry and Oral Epidemiology, 29, 456-463.
http://dx.doi.org/10.1034/j.1600-0528.2001.290607.x - 19. Berggren, U., Hakeberg, M. and Carlsson, S.G. (2000) Relaxation vs. Cognitively Oriented Therapies for Dental Fear. Journal of Dental Research, 79, 1645-1651.
http://dx.doi.org/10.1177/00220345000790090201 - 20. Teng, P.R., Su, J.M., Chang, W.H. and Lai, T.J. (2011) Oral Health of Psychiatric Inpatients: A Survey of Central Taiwan Hospitals. General Hospital Psychiatry, 33, 253-259.
http://dx.doi.org/10.1016/j.genhosppsych.2011.03.001 - 21. Lenk, M., Berth, H., Joraschky, P., Petrowski, K., Weidner, K. and Hannig, C. (2013) Fear of Dental Treatment—An Under Recognized Symptom in People with Impaired Mental Health. Deutsches Ärzteblatt International, 110, 517-523.
http://dx.doi.org/10.3238/arztebl.2013.0517 - 22. Hede, B. and Petersen, P.E. (1992) Self-Assessment of Dental Health among Danish Noninstitutionalized Psychiatric Patients. Special Care in Dentistry, 12, 33-36.
http://dx.doi.org/10.1111/j.1754-4505.1992.tb00405.x - 23. Hede, B. (1995) Dental Health Behavior and Self-Reported Dental Health Problems among Hospitalized Psychiatric Patients in Denmark. Acta Odontologica Scandinavica, 53, 35-40.
http://dx.doi.org/10.3109/00016359509005942 - 24. Angelillo, I.F., Nobile, C.G.A., Pavia, M., DeFazio, P., Puca, M. and Amati, A. (1995) Dental Health and Treatment Needs in Institutionalized Psychiatric Patients in Italy. Community Dentistry and Oral Epidemiology, 23, 360-364.
http://dx.doi.org/10.1111/j.1600-0528.1995.tb00263.x - 25. Enkling, N., Marwinski, G. and Johren, P. (2006) Dental Anxiety in a Representative Sample of Residents of a Large German City. Clinical Oral Investigations, 10, 84-91.
http://dx.doi.org/10.1007/s00784-006-0035-6 - 26. Davey, G.C. (1989) Dental Phobias and Anxieties: Evidence for Conditioning Processes in the Acquisition and Modulation of a Learned Fear. Behaviour Research and Therapy, 27, 51-58.
http://dx.doi.org/10.1016/0005-7967(89)90119-8 - 27. De Jongh, A. (1995) Dental Anxiety: A Cognitive Perspective. Doctoral Dissertation, Ridderprint, Amsterdam.
- 28. deJongh, A., Fransen, J., Oosterink-Wubbe, F. and Aartman, I. (2006) Psychological Trauma Exposure and Trauma Symptoms among Individuals with High and Low Levels of Dental Anxiety. European Journal of Oral Sciences, 114, 286-292.
http://dx.doi.org/10.1111/j.1600-0722.2006.00384.x - 29. Taylor, S., Koch, W.J. and McNally, R.J. (1992) How Does Anxiety Sensitivity Vary across the Anxiety Disorders? Journal of Anxiety Disorders, 6, 249-259.
http://dx.doi.org/10.1016/0887-6185(92)90037-8 - 30. Reiss, S., Peterson, R.A., Gursky, D.M. and McNally, R.J. (1986) Anxiety Sensitivity, Anxiety Frequency and Prediction of Fearfulness. Behaviour Research and Therapy, 24, 1-8.
http://dx.doi.org/10.1016/0005-7967(86)90143-9 - 31. Reiss, S. (1997) Trait Anxiety: It’s Not What You Think It Is. Journal of Anxiety Disorders, 11, 201-214.
http://dx.doi.org/10.1016/S0887-6185(97)00006-6 - 32. Seligman, M. (1971) Phobias and Preparedness. Behaviour Therapy, 2, 307-320.
http://dx.doi.org/10.1016/S0005-7894(71)80064-3 - 33. Armfield, J.M. (2006) Cognitive Vulnerability: A Model of the Etiology of Fear. Clinical Psychology Review, 26, 746-768.
http://dx.doi.org/10.1016/j.cpr.2006.03.007 - 34. Armfield, J.M., Slade, G.D. and Spencer, A.J. (2008) Cognitive Vulnerability and Dental Fear. BMC Oral Health, 8, 2.
http://dx.doi.org/10.1186/1472-6831-8-2 - 35. Edmunds, R. and Buchanan, H. (2012) Cognitive Vulnerability and the Aetiology and Maintenance of Dental Anxiety. Community Dentistry and Oral Epidemiology, 40, 17-25.
http://dx.doi.org/10.1111/j.1600-0528.2011.00636.x - 36. Taylor, S. (1995) Anxiety Sensitivity: Theoretical Perspectives and Recent Findings. Behaviour Research and Therapy, 33, 243-258.
http://dx.doi.org/10.1016/0005-7967(94)00063-P - 37. Seligman, M. (1970) On the Generality of the Laws of Learning. Psychological Review, 77, 406-418.
http://dx.doi.org/10.1037/h0029790 - 38. Berggren, U. (1992) General and Specific Fears in Referred and Self-Referred Adult Patients with Extreme Dental Anxiety. Behaviour Research and Therapy, 30, 395-401.
http://dx.doi.org/10.1016/0005-7967(92)90051-H - 39. Stenebrand, A., Wide Boman, U. and Hakeberg, M. (2013) General Fearfulness, Attitudes to Dental Care, and Dental Anxiety in Adolescents. European Journal of Oral Sciences, 121, 252-257.
http://dx.doi.org/10.1111/eos.12031 - 40. Corah, N.L. (1969) Development of a Dental Anxiety Scale. Journal of Dental Research, 48, 596.
http://dx.doi.org/10.1177/00220345690480041801 - 41. Corah, N.L., Gale, E.N. and Illing, S.J. (1978) Assessment of a Dental Anxiety Scale. Journal of the American Dental Association, 97, 816-819.
http://dx.doi.org/10.14219/jada.archive.1978.0394 - 42. Vujanovic, A.A., Arrindell, W.A., Bernstein, A., Norton, P.J. and Zvolensky, M.J. (2007) Sixteen-Item Anxiety Sensitivity Index-Confirmatory Factor Analytic Evidence, Internal Consistency, and Construct Validity in a Young Adult Sample from the Netherlands. Assessment, 14, 129-143.
http://dx.doi.org/10.1177/1073191106295053 - 43. Moore, R., Berggren, U. and Carlsson, S.G. (1991) Reliability and Clinical Usefulness of Psychometric Measures in a Self-Referred Population of Odontophobics. Community Dentistry and Oral Epidemiology, 19, 347-351.
http://dx.doi.org/10.1111/j.1600-0528.1991.tb00185.x - 44. Logan, H.L. and Baron, R.S. (1987) Perceived Control and Dental Fear. Journal of Dental Research, 66, 345-345.
- 45. Kruse, M. and Helweg-Larsen, K. (2004) Gender Differences In disease and Health—An Exposure of Areas of Illness Where Women and Men Differ and of Gender Differences in Risk Factors for Disease and the Response to Disease Symptoms [Kønsforskelle i sygdom og sundhed—En afdækning af sygdomsområder hvor kvinder og mænd skiller sig særligt ud, af kønsforskelle i risikofaktorer for sygdom og i reaktionen på sygdomssymptomer]. Report Ministry of Equality, Copenhagen, 44-45.
http://www.si-folkesundhed.dk/upload/konsforskelle_rapport.pdf