Health
Vol.5 No.11(2013), Article ID:39459,7 pages DOI:10.4236/health.2013.511240
Preferences for behavioral therapies for chronic insomnia
![]()
1Department of Nursing, McMaster University, Hamilton, Canada; *Corresponding Author: ibrahs8@mcmaster.ca
2Department of Nursing, Ryerson University, Toronto, Canada
Copyright © 2013 Sarah Ibrahim, Souraya Sidani. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received 29 August 2013; revised 29 September 2013; accepted 15 October 2013
Keywords: Acceptability; Preference; Insomnia; Behavioural Treatment
ABSTRACT
Purpose: The purpose of this study was twofold: to examine the acceptability and preference for the two behavioral therapies, and to identify factors persons with chronic insomnia take into account when choosing treatment. Methods: The data were obtained in a large trial evaluating the effects of Stimulus Control and Sleep Restriction therapies. Prior to treatment, participants completed the treatment acceptability and preference (TAP) questionnaire, which described the Stimulus Control Therapy and the Sleep Restriction Therapy and requested participants to rate the acceptability of each treatment option before choosing one for the management of chronic insomnia. Open-ended questions were used to explore the factors that participants considered when making a choice. Results: Participants rated the Sleep Restriction Therapy as acceptable and 70.2% of participants preferred it over Stimulus Control Therapy. The factors that influenced participants’ choice related to the familiarity, previous personal experience, novelty, and suitability of the treatment. Conclusion: Persons have expressed a preference for treatments to manage chronic insomnia. Healthcare providers are in a position to provide relevant information about treatment options in order to help persons make informed treatment related decisions.
1. INTRODUCTION
Insomnia affects between 30% and 35% of the adult population [1]. Insomnia is characterized by dissatisfaction with sleep quality and quantity and complaint of having difficulty falling asleep, waking up in the middle of the night or too early in the morning [2]. Insomnia is linked to daytime symptoms such as fatigue, low energy, altered cognitive functions (i.e., concentration, memory), mood disturbance (i.e., irritability) [2] and loss of work and productivity [1]. Currently, there are two treatment modalities for managing insomnia, pharmacological (i.e., hypnotics) and behavioural. Behavioral Therapy (BT) is an effective psychological treatment for the management of insomnia. The objectives of BT are to change poor sleep habits, distorted beliefs and attitude towards sleep and to promote better sleep habits and approaches [2]. BT includes sleep restriction therapy, stimulus control therapy, sleep hygiene and education and relaxation [2-4]. Evidence from several meta-analysis [5-7] and systematic reviews [8-12] suggests BT decreases sleep onset latency and number and duration of awakenings, and improves total sleep time and sleep quality for persons with chronic insomnia. Whereas there is empirical evidence reporting on the effectiveness of BT for the management of insomnia, little is known about persons’ views regarding the acceptability and preference for behavioral treatments [13,14].
Acceptability denotes a favourable attitude towards a treatment upon careful consideration of the treatment attributes, including its perceived effectiveness, convenience, risks, and suitability [15]. Perceived acceptability influences treatment preference. Preference is the choice of treatment for the management of a health or clinical problem such as insomnia [16,17]. Assessment of patients’ preference and provision of the preferred treatment are key components of patient-centered care (PCC) and evidence-based practice [18,19].
Numerous studies have investigated patients’ preferences and its impact on initiation, adherence, satisfaction and outcome of treatment. Empirical evidence demonstrates that most (≥60%) patients express a preference for treatment [e.g. 13,18,20-22]. Treatment preferences affect the results of an intervention evaluation trial. Participants who do not receive the preferred treatment often lack the motivation to engage and adhere to treatment; they withdraw from treatment [16]. High attrition reduces the statistical power to detect significant intervention effects. In contrast, participants who receive treatment of choice are satisfied with the allocated treatment. They are motivated, engage in and adhere to treatment; this in turn improves outcome achievement [23,24].
Three studies have examined acceptability and preference of behavioral treatments for managing chronic insomnia for Veterans [15] and adults [13,14]. Findings from the studies showed participants viewed the treatments as acceptable and expressed clear preferences. Morin and colleagues [14] found that persons with chronic insomnia rated behavioral therapies as more acceptable and suitable than pharmacological ones. Specifically, they perceived the behavioral therapies to be more effective in the long term, produce fewer side effects and are beneficial in maintaining daytime functioning [14]. Vincent and Lionberg [13] replicated Morin and colleagues’ [14] study but targeted younger adults. They reported similar findings in that participants preferred BT for the management of chronic insomnia. Although most persons favor BT, Epstein and colleagues [15], found relaxation therapy and pharmacotherapy treatments to be more acceptable and preferable for managing chronic insomnia among Veterans. Pharmacotherapy was perceived to be a “quick fix” for Veterans in order to meet the demands of their arduous schedules; however, Veterans indicated pharmacotherapy to not be a desirable long term treatment for managing chronic insomnia.
Although the available evidence indicates persons with insomnia have a preference for treatment, the studies [13-15] examined preferences in the context of hypothetical scenarios. Participants were provided descriptions of the treatments and asked to rate their acceptability and preference for insomnia treatments; however, they did not receive treatment. There is the potential for discrepancies between hypothetical and actual evaluations of treatments [25], which may influence the expressed preferences. In addition, although researchers explored participants’ perceived acceptability and preference, they did not explore the factors that persons take into consideration when making a choice. Knowledge of these factors is useful in guiding the decision making process, in that pertinent information is given to the persons included in the process and the persons are encouraged to account for the factors when selecting treatment.
This study is part of a large trial that evaluated the contribution of preferences to the effectiveness of behavioral therapies for chronic insomnia. In the trial, participants were informed of the behavioral therapies for managing chronic insomnia, rated their acceptability, and indicated their choice of treatment; participants were then given the selected treatment. The specific aims of this study were to: 1) examine the perceived acceptability and preference for two behavioral therapies (Stimulus Control Therapy and Sleep Restriction Therapy; described in next section) for the management of chronic insomnia; and 2) identify the factors persons take into account when choosing treatment.
2. METHODS
2.1. Design
Data were obtained from the large trial and related to participants’ perception of the acceptability and preference for Stimulus Control Therapy (SCT) and Sleep Restriction Therapy (SRT). Treatment acceptability and preference were assessed prior to implementation of treatment and guided allocation to treatment. The data were collected in a face-to-face session. Participants completed sets of quantitative and qualitative items. Quantitative items were used to measure treatment acceptability and preference for the two behavioral therapies. Qualitative, open-ended questions were used to explore the factors that participants considered when making a choice. The two behavioral therapies demonstrated short and long-term effectiveness in reducing the severity of insomnia [26,27]. The SCT provides instructions on specific activities to do or avoid around bedtime and during the night, as well as changes to make in the bedroom (e.g. going to bed when sleepy, getting out of bed if cannot fall asleep in 15 - 20 minutes). The goal is to re-associate the bed and bedroom with sleep. The SRT uses participants’ reported sleep diaries to develop an individualized, consistent sleep-wake schedule. The goal is to consolidate sleep by restricting the amount of time physically spent in bed to be as close as possible to the total amount of sleep time.
2.2. Sample
The same eligibility criteria as those applied in the large trial were used for this study. Persons were eligible if they: 1) reported difficulty falling and or staying asleep for 30 minutes or more, for 3 nights or more per week as documented by one week of sleep diaries; 2) experienced insomnia for at least 6 weeks; 3) were 40 years of age or older; 4) were residing in the community; and 5) were able to read and write in English. Exclusion criteria for this study were 1) cognitive impairment, ascertained by a Mini-Mental State Exam (MMSE) score of <24. The behavioral interventions for managing insomnia require participants to actively change their behaviours, which may be hindered by cognitive impairment, and 2) selfreport of sleep apnea. The behavioral therapies for managing chronic insomnia are minimally effective for persons with sleep apnea.
2.3. Variables and Measures
2.3.1. Demographic and Clinical Characteristics
Demographic characteristics including age, gender, marital status, ethnic origin, education and employment status were assessed with standard questions. Clinical characteristics related to the perception of insomnia severity. This was measured with the Insomnia Severity Index (ISI). The items on the ISI captured the perception of current satisfaction with sleep pattern, level of interference with daily functioning, noticeability of sleep impairment to others, and level of distress related to insomnia. A five-point Likert scale was used; it ranged from 0 (not at all) to 4 (extremely), with a total score ranging from 0 to 28. A high score on the ISI indicates severe insomnia. The ISI has demonstrated validity and reliability [28].
2.3.2. Treatment Acceptability and Preferences
The Treatment Acceptability and Preference (TAP) was used to assess participants’ perceived acceptability and preference for the two behavioral therapies. The TAP is an adaptation of the measure developed by Sidani and colleagues [29] and used by Epstein and colleagues [15]. The TAP consists of three parts. The first part includes a description of one behavioral treatment in terms of its: purpose, goals, dose, mode of delivery, activities, schedule, effectiveness (based on available empirical findings), and risks or side effects. Following the description of the treatment is a set of items used to rate the treatment acceptability in terms of its: perceived suitability, short and long-term effectiveness, convenience of use in daily life, severity of side effects, and degree of willingness to comply with treatment. The second part contains the description and items for rating the acceptability of the other behavioral treatment. After rating the acceptability of the two treatments, participants complete the third part of the TAP which includes questions related to whether or not they have a preference and the treatment of choice. The TAP items measuring acceptability has demonstrated good internal consistency reliability in this study (Cronbach’s α > 0.80).
2.3.3. Factors Affecting Preferences
An open-ended question was asked of participants indicating a choice. The question inquired about the reasons underlying their preference for the behavioral therapy.
3. PROCEDURE
The study protocol was approved by the Research Ethics Board at Ryerson University. Eligible persons participated in a face-to-face session during which the research assistant (RA) described the purpose of the study, the data collection procedure, the two behavioural therapies under evaluation in the large trial (i.e., SCT and SRT), and procedure for treatment allocation. The RA addressed any concerns prior to obtaining participants’ consent. After obtaining consent, the RA administered the TAP measure. Specifically, the RA read the description of each behavioural therapy (SCT and SRT), the items assessing acceptability and preferences, and recorded participants’ responses. The RA then asked the open ended questions and documented participants’ reasons underlying their choice of treatment, verbatim.
Data Analysis
Descriptive statistics were used to examine the acceptability and preference for the SCT and SRT. Specifically, the mean, standard deviation and frequency distribution for each item of the TAP were reported. The qualitative data were content analyzed. They were coded and categorized into themes that reflected reasons underlying the participants’ expressed preference for treatment. Both authors, independently, read the short responses provided by participants, coded the responses, compared and contrasted the codes to identify factors that persons take into account when choosing a treatment for managing chronic insomnia. The authors then met to discuss the emergent themes from the qualitative data. Any discrepancy was resolved through consensus. The number of participants who indicated a particular factor was counted.
4. RESULTS
A total of 204 persons provided data for this study. The majority of participants were female (70.6%), White (77.0%) and older adults with a mean age of 60.40 years (SD = 10.42). About half (51.0%) were married and 49% were single, widowed, separated, or divorced. On average, participants were well-educated (mean years of education = 16.48, SD = 4.26) and employed (49.9%) either part-time or full time. Participants complained of having difficulty falling asleep (82%) and maintaining sleep (98.5%). Participants reported having insomnia for an average of 11.63 years (SD = 12.70) and rated their insomnia as moderate to severe (mean score on the ISI 17.71, SD = 4.67).
Participants reported higher levels of acceptability for the SRT than the SCT (Table 1). They perceived the SRT to be more effective in managing insomnia in the short and long term, in reducing fatigue, and in improving daily functioning. They rated SRT as more suitable or appropriate than the SCT. The majority of participants (n = 174, 85.3%) reported having a preference whereas 30 (14.7%) expressed no preference for either of the be
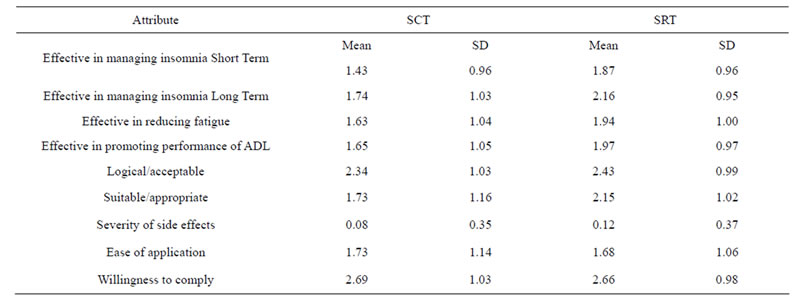
Table 1. Perceived acceptability of stimulus control therapy and sleep restriction therapy.
havioral therapies. Of those with a preference, 125 (70.2%), preferred SRT and 53 participants (29.8%) preferred SCT.
Factors Underlying Choice of Treatment
The themes that emerged from the content analysis of the short verbal responses identified factors that participants take into consideration when choosing behavioral treatments for insomnia (Table 2). Four categories of factors emerged as underlying the expressed preference for SRT. These were: 1) personal experience with the SRT: participants who learned about its effectiveness through personal or significant others’ experience, expressed a preference for the SRT; 2) previous experience with the alternative treatment (SCT): participants who believed they have applied some aspects of the SCT preferred the SRT: participants who were not aware of the SRT indicated a preference for this therapy; 3) the novelty of the SRT; and 4) perception of the SRT to be effective: participants related its effectiveness to its underlying mechanisms (i.e., promoted good sleep, consolidated sleep), way in which it was implemented, and suitability to personal needs and life.
Similar categories of factors emerged as influencing preference for SCT. These were: 1) perception of the alternative treatments’ (SRT) requirements (i.e., difficulty staying on the schedule, not wanting a sleep schedule); 2) perception of the SCT treatment (i.e., easy to implement, flexible); 3) and the novelty of the SCT treatment. An additional factor was accounted for when choosing the SCT; it had to do with the fit of the SCT instructions with participants’ needs and life circumstances.
5. DISCUSSION
Similar to other studies [13-15], the results indicated that majority of participants (85.3%) expressed distinct preference for the behavioral therapies for managing chronic insomnia. The behavioral treatment rated as most acceptable was also the one participants preferred, a finding that is consistent with those of Epstein et al. [15] and Sidani et al. [30]. Majority of participants reported higher levels of acceptability and preference for SRT (70.2%). They perceived it to be more effective in improving in the short and long term, daily functioning, and reducing fatigue than SCT. The identified factors that influenced their choice were perception of and personal experience with the treatment, previous experience with the alternative treatment, and novelty of the treatment. This implies that perceived acceptability shapes preferences for treatment. Acceptability reflects a favourable view of the treatment that is based on a systematic evaluation of its attributes including effectiveness, convenience, suitability and severity of side effects.
Participants identified additional factors that influence treatment preference. These were familiarity, personal experience, novelty, and suitability of treatment. The factors that participants considered in choosing behavioral therapies related to the characteristics of treatment. These factors are comparable to those reported by Sidani et al. [30], Zoeller et al. [31], and Lambert et al. [32]. Sidani et al. [30] found convenience was the most significant predictor of expressed preference for behavioral intervention for the management of insomnia was influenced by convenience of the treatment. Zoeller et al. [31] explored the reasons underlying patients’ preference for PTSD treatment; perceived efficacy and credibility of the treatment were commonly reported. Lambert et al. [32] results indicated that effectiveness, suitability, appropriateness, and convenience were important factors influencing treatment choice for persons with cardiac disease. The majority of participants in this study had a preference for SRT, which was not the case in Epstein et al.’s

Table 2. Factors underlying treatment preferences.
[15] study. Differences in the personal and clinical characteristics of the target populations explain the inconsistent finding. This study participants were older women who had insomnia for an average of 11 years. In contrast, Epstein et al. [15] included soldiers returning from war, most being young men; they may have developed insomnia following their traumatic experience and the resulting anxiety, which may have contributed to their choice of treatment. Older women with chronic insomnia participating in this study may have had the opportunity to try alternative treatments, including SCT as suggested by their responses to the open-ended questions. Prior experience with a treatment has been found to affect preferences in that persons who carry out a treatment and find it ineffective tend to select another treatment. This observation is supported by the results of Awad et al. (2000) [33] and Miranda (2004) [23]. Awad et al. [33] reported that participants not satisfied with their current treatment for edentulism (i.e., loss of teeth) selected the alternative treatment offered in the study. Miranda’s [23] results revealed that participants chose the therapy with which they were not familiar and have not applied previously.
The study has some limitations. The sample consisted primarily of White female and older adults experiencing severe levels of insomnia. In order to enhance the generalizability, the study should be replicated with persons with diverse personal, socio-cultural and clinical characteristics. Persons of diverse background may have a different perception of the treatment attributes and options and may consider a variety of factors when choosing treatment.
The findings provide evidence indicating that participants have preferences for specific behavioral therapies for the management of chronic insomnia. Participants were able o distinguish between the treatments and to evaluate them relative to characteristics prior to choosing one. Findings of this study highlight the importance of providing persons with insomnia relevant information about each treatment and assisting them in considering the treatment characteristics identified in this study to help them make informed decisions and choose treatment. Healthcare providers and researchers planning to elicit patients’ treatment preferences can follow a systematic process in this endeavor. The process involves 1) presenting balanced descriptions of the treatment explaining the goal, components, activities, mode of delivery, dose, benefits or effectiveness and side effects in simple lay terms, 2) requesting persons to read the information carefully, 3) counseling them to rate each treatment for its perceived effectiveness, convenience, appropriateness, severity of side effects and suitability to their life condition, and 4) asking them to indicate which they prefer to have in order to successfully manage the health or clinical problem.
6. CONCLUSION
This study’s findings indicated that persons have preferences for different behavioural treatments for managing chronic insomnia. The majority of patients rated the SRT to be acceptable and expressed preference for this behavioural treatment. Familiarity, personal experience, novelty, and suitability of treatment were factors taken into consideration when selecting treatment. The results of this study highlight the importance of presenting treatment information and discussing treatment characteristics to facilitate treatment selection.
7. ACKNOWLEDGEMENTS
Funding received from the Canadian Institutes of Health Research.
REFERENCES
- Bain, K.T. (2006) Management of chronic insomnia in elderly persons. The American Journal of Geriatric Pharmacotherapy, 4, 168-192. http://dx.doi.org/10.1016/j.amjopharm.2006.06.006
- Morin, C. and Benca, R. (2012) Chronic insomnia. The Lancet, 379, 1129-1141. http://dx.doi.org/10.1016/S0140-6736(11)60750-2
- Morin, C.M. and Espie, C.A. (2003) Insomnia: A clinical guide to assessment and treatment. Kluwer Academic/ Plenum, New York.
- Edinger, J.D. and Carney, C.E. (2008) Overcoming insomnia: A cognitive-behavioral therapy approach-therapist guide. Oxford University Press, New York.
- Murtagh, D.R. and Greenwood, K.M. (1995) Identifying effective psychological treatments for insomnia: A metaanalysis. Journal of Consulting and Clinical Psychology, 63, 79-89. http://dx.doi.org/10.1037/0022-006X.63.1.79
- Morin, C.M., Culbert, J.P. and Schwartz, S.M. (1994) Nonpharmacological interventions for insomnia: A meta-analysis of treatment efficacy. American Journal of Psychiatry, 151, 1172-1180.
- Smith, M.T., Perlis, M.L., Park, A., Smith, M.S., Pennington, J., Giles, D.E. and Buysse, D.J. (2002) Comparative meta-analysis of pharmacotherapy and behavior therapy for persistent insomnia. American Journal of Psychiatry, 159, 5-11. http://dx.doi.org/10.1176/appi.ajp.159.1.5
- Morin, C.M., Hauri, P.J., Espie, C.A., Spielman, A.J., Buysse, D.J. and Bootzin, R.R. (1999) Nonpharmacologic treatment of chronic insomnia. An American academy of sleep medicine review. Sleep, 22, 1134-1156.
- Irwin, M.R., Cole, J.C. and Nicassio, P.M. (2006) Comparative meta-analysis of behavioral interventions for insomnia and their efficacy in middle-aged adults and in older adults 55+ years of age. Health Psychology, 25, 3- 14. http://dx.doi.org/10.1037/0278-6133.25.1.3
- McCurry, S.M., Logsdon, R.G., Teri, L., and Vitiello, M.V. (2007) Evidence-based psychological treatments for insomnia in older adults. Psychology and Aging, 22, 18-27. http://dx.doi.org/10.1037/0882-7974.22.1.18
- Morin, C.M., Bootzin, R.R., Buysse, D.J., Edinger, J.D., Espie, C.A. and Lichstein, K.L. (2006) Psychological and behavioral treatment of insomnia: Update of the recent evidence (1998-2004). Sleep, 29, 1398-1414.
- Morgenthaler, T., Kramer, M., Alessi, C., Friedman, L. and Boehlecke, B. (2006) Practice parameters for the psychological and behavioral treatment of insomnia: An update. Sleep, 29, 1415-1419.
- Vincent, N. and Lionberg, C. (2001) Treatment preference and patient satisfaction in chronic insomnia. Journal of Sleep and Sleep Disorders Research, 24, 411-417.
- Morin, C.M., Gaulier, B., Barry, T. and Kowatch, R.A. (1992) Patients’ acceptance of psychological and pharmacological therapies for insomnia. Sleep, 15, 302-305.
- Epstein, D.R., Babcock-Parziale, J.L., Haynes, P.L. and Herb, C.A. (2012) Insomnia treatment acceptability and preferences for male Iraq and Afghanistan combat Veterans and their healthcare providers. Journal of Rehabilitation Research and Development, 49, 867-878. http://dx.doi.org/10.1682/JRRD.2011.06.0114
- Corrigan, P.W. and Salzer, M.S. (2003) The conflict between random assignment and treatment preference: Implications for internal validity. Evaluation and Program Planning, 26, 109-121. http://dx.doi.org/10.1016/S0149-7189(03)00014-4
- Sidani, S., Epstein, D. and Miranda, J. (2006) Eliciting patient treatment preferences: A strategy to integrative evidence-based and patient-centered care. Worldviews on Evidence Based Nursing, 3, 116-123. http://dx.doi.org/10.1111/j.1741-6787.2006.00060.x
- Swift, J.K., Callahan, J.L. and Vollmer, B.M. (2011) Preferences. Journal of Clinical Psychology, 67, 155-165. http://dx.doi.org/10.1002/jclp.20759
- Sidani, S. and Braden, C.J. (2011) Design, evaluation, and translation of nursing interventions. Wiley-Blackwell, Ames, IA.
- Lin, P., Campbell, D.G., Chaney, E.F., Liu, C., Heagerty, P., Felker, B.L. and Hedrick, S.C. (2005) The influence of patient preference on depression treatment in primary care. Annals of Behavioral Medicine, 30, 164-173. http://dx.doi.org/10.1207/s15324796abm3002_9
- Mergl, R., Henkel, V., Allgaier, A.K., Kramer, D., Hautzinger, M., Kohen, R., Coyne, J. and Hegerl, U. (2011) Are treatment preferences relevant in response to serotonergic antidepressants and cognitive-behavioral therapy in depressed primary care patients? Results from a randomized controlled trial including a patients’ choice arm. Psychotherapy and Psychosomatics, 80, 39-47. http://dx.doi.org/10.1159/000318772
- Swift, J.K. and Callahan, J.L. (2009) The impact of client treatment preferences on outcome: A meta-analysis. Journal of Clinical Psychology, 65, 368-381. http://dx.doi.org/10.1002/jclp.20553
- Miranda, J. (2004) An exploration of participants’ treatment preferences in a partial RCT. Canadian Journal of Nursing Research, 41, 276-290.
- Sidani, S., Miranda, J., Epstein, D. and Fox, M. (2009) Influence of treatment preferences on validity: A review. Canadian Journal of Nursing Research, 41, 52-67.
- Jansen, S.J.T., Stiggelbout, A.M., Wakker, P.P., Nooij, M.A., Noordijk, E.M. and Kievit, J. (2000) Unstable preferences: A shift in valuation or an effect of the elicitation procedure? Medical Decision Making, 20, 62-71. http://dx.doi.org/10.1177/0272989X0002000108
- Irwin, M.R., Cole, J. and Nicassio, P.M. (2006) Comparative analysis of behavioral interventions for insomnia and their efficacy in middle-aged adults and older adults 55 + years of age. Health Psychology, 25, 3-14. http://dx.doi.org/10.1037/0278-6133.25.1.3
- Morin, C.M., Bootain, R.R., Buysse, D.J., Edinger, J.D., Espie, C.A. and Lichstein, K.L. (2006) Psychological and behavioral treatment of insomnia: Update of the recent evidence (1998-2004). Sleep, 29, 1398-1414.
- Bastien, C.H., Vallieres, A. and Morin, C.M. (2001) Validation of the insomnia severity index as an outcome measure for insomnia research. Sleep Medicine, 2, 297- 307. http://dx.doi.org/10.1016/S1389-9457(00)00065-4
- Sidani, S., Epstein, D.R., Bootzin, R.R., Moritz, P. and Miranda, J. (2009) Assessment of preferences for treatment: Validation of a measure. Research in Nursing and Health, 32, 419-431. http://dx.doi.org/10.1002/nur.20329
- Sidani, S., Miranda, J, Epstein, D.R., Bootzin, R.R., Cousins, J. and Moritz, P. (2009) Relationships between personal beliefs and treatment acceptability, and preferences for behavioral treatments. Behavior Research and Therapy, 47, 823-829. http://dx.doi.org/10.1016/j.brat.2009.06.009
- Zoeller, L.A., Feeny, N.C., Cochran, B. and Pruitt, L. (2003) Treatment choice for PTSD. Behaviour Research and Therapy, 41, 879-886. http://dx.doi.org/10.1016/S0005-7967(02)00100-6
- Lambert, N., Rowe, G., Bowling, A., Ebrahim, S., Laurence, M., Dalrymple, J. and Thomson, R. (2004) Reasons underpinning patients’ preferences for various angina treatments. Health Expectations, 6, 246-256. http://dx.doi.org/10.1111/j.1369-7625.2004.00282.x
- Awad, M.A., Shapiro, S.H., Lund, J.P. and Feine, J.S. (2000) Determinants of patients’ treatment preferences in a clinical trial. Community Dentistry and Oral Epidemiology, 28, 119-125. http://dx.doi.org/10.1034/j.1600-0528.2000.028002119.x
NOTE LIST OF ABBREVIATIONS
BT: Behavioral Treatment PCC: Patient Centered Care SCT: Stimulus Control Therapy SRT: Sleep Restriction Therapy TAP: Treatment Acceptability and Preference RA: Research Assistant

