Health
Vol.5 No.8B(2013), Article ID:35854,8 pages DOI:10.4236/health.2013.58A2006
Sleep disordered breathing in coronary heart disease patients with mild and moderate heart failure
![]()
Behavioral Medicine Institute of the Lithuanian University of Health Sciences, Palanga, Lithuania; *Corresponding Author: giedvar@ktl.mii.lt
Copyright © 2013 Giedrius Varoneckas et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received 7 June 2013; revised 7 July 2013; accepted 31 July 2013
Keywords: Sleep; Sleep Apnoea; Oxygen Desaturation; Coronary Heart Disease; Heart Failure
ABSTRACT
The purpose of the study was to investigate the relationship between sleep disordered breathing (SDB) and degree of heart failure (HF) in patients with coronary heart disease (CHD). A total of 3017 patients (77.4% men and 22.6% women) were included in the study. Clinical examination and echocardiography for evaluation of HF using NYHA functional classification and sleep polysomnography were performed. The study demonstrated that SDB is more common in CHD patients with higher NYHA functional class. The prevalence of central sleep apneas against obstructive apneas was observed in patients with mild and moderate HF. The number of central apneas was strongly related to the severity of heart failure. More frequent appearance of central sleep apneas is predominantly due to instability of ventilatory control systems during sleep because of impaired cardiac function in HF patients. Sleep architecture was more disturbed in CHD patients with higher NYHA functional class. A gradual increase of stage 1 and wakefulness after sleep onset and a decrease of sleep stages 3-4 and REM sleep as well as a diminution of sleep efficiency with worsening of NYHA functional class were observed. We suggest that both SDB and disturbed sleep variables independently significantly correlate with manifestation of HF.
1. INTRODUCTION
Sleep disordered breathing (SDB) is a common chronic disorder with a major impact on morbidity and mortality in the general population [1,2]. Moderate to severe sleep apnoea was reported to be present in 5.7% [3]. Other studies found the prevalence of moderate sleep apnoea to be between 1% and 14%, thus it is reasonable to assume that 1 in 5 adults has at least mild sleep apnoea, and 1 in 15 adults has at least moderate sleep apnoea [4].
SDB is recognized as an independent risk factor for cardiovascular impairment [5]. Hypertension, coronary heart disease (CHD), diabetes, heart rhythm and conduction abnormalities, cerebrovascular disease, and heart failure (HF) have all been linked to this syndrome [6-8]. On the other hand, CHD is a major risk factor for HF which is increasingly becoming a health concern worldwide, since it contributes to increased morbidity and mortality. It has been reported that sleep disordered breathing (SDB) is experienced by approximately half of the patients with HF [9-12].
SDB is classified mainly as either obstructive sleep apnoea (OSA) or central sleep apnoea (CSA). The former is characterized by repetitive collapse of the upper airway, whereas the latter is due to periodic loss of ventilatory drive [9]. In contrast to OSA, it is likely that CSA is a consequence rather than a cause of heart failure (HF). CSA is more frequent among HF patients and related to HF severity [9,10]. CSA may promote disease progression and mortality in HF patients [11,12]. While OSA is a cardiovascular risk factor per se [13-16], CSA appears to be a marker of HF severity [17,18].
However, the relationship between severity of SDB and incident HF has been less studied. Since the presence of SDB has a predictive value for the development of CHD and is known to be associated with established HF [19], we hypothesized that the severity of HF would also predict a degree of SDB.
Thus, the aim of the study was to specify the relationship between sleep apnoea and degree of heart failure in patients with coronary heart disease.
2. METHODS
2.1. Subjects
Consecutive patients diagnosed with CHD attending rehabilitation program at the Cardiovascular Rehabilitation Clinic of the Behaviour Medicine Institute of the Lithuanian University of Health Sciences in Palanga, Lithuania during the period from 2000 to 2006 were included in the study. A total of 3017 patients (77.4% men and 22.6% women; mean age 59.7 ± 9.9 years) were included in the study. All the patients were on standard treatment for secondary prevention of CHD according to existing guidelines.
2.2. Procedure and Instruments
The study was planned according to the declaration of Helsinki and approved by the Lithuanian Ethical Committee. The subjects of the study gave a written informed consent.
All patients had a clinical cardiovascular examination and were evaluated for demographic characteristics, for past and current CHD diagnosis and treatments. The study patients underwent two-dimensional transthoracic echocardiography on the day of the sleep study. The left ventricle ejection fraction was calculated using Simpson’s biplane methods. The definition of HF was the presence of cardiac symptoms and moderately or severely reduced ventricular systolic function. The HF was determined according to the New York Heart Association (NYHA) functional classification system which describes the impact of heart failure on a patient’s daily activities [20]. A higher class indicates more severe symptoms, limitation in physical activity, and worse health.
NYHA classification—The stages of heart failure [20].
| Class | Patient Symptoms |
| Class I (No impact) | No limitation of physical activity. Ordinary physical activity does not cause undue fatigue, palpitation, or dyspnea (shortness of breath). |
| Class II (Mild) | Slight limitation of physical activity. Comfortable at rest, but ordinary physical activity results in fatigue, palpitation, or dyspnea. |
| Class III (Moderate) | Marked limitation of physical activity. Comfortable at rest, but less than ordinary activity causes fatigue, palpitation, or dyspnea. |
| Class IV (Severe) | Unable to carry out any physical activity without discomfort. Symptoms of cardiac insufficiency at rest. If any physical activity is undertaken, discomfort is increased. |
Sleep data were recorded using standard polysomnography. Electrooculography, electroencephalography, chin electromyography, nasal flow, thoracic and abdominal respiration, and finger pulse oximetry were recorded using Alice-4 model polysomnograph (Respironics). The records were scored with the Rechtshaffen and Kales criteria [21]. The sleep architecture was examined by the following parameters: Total sleep time, sleep latency, wakefulness after sleep onset, time spent in sleep stage 1, stage 2, slow-wave sleep (stage 3 and stage 4 combined), and REM sleep in absolute and relative values. The percentage of sleep efficiency and sleep onset latency were chosen as objective indices of sleep efficiency. The percentage of sleep efficiency was computed as the ratio of total sleep time to time spent in bed multiplied by 100.)
The total number of apneas and hypopneas per hour of sleep was determined, as well as the total number of obstructive (OSA), central (CSA), and mixed sleep apneas (MSA) and hypopneas per hour. Apnoe-hypopnea index (AHI) was defined as the total number of apneas plus hypopneas per hour of sleep. OSA, CSA and MSA and hypopnea indexes were defined as the total number of respective apneas/hypopneas per hour of sleep. OSA was defined as cessation of oronasal airflow for ≥10 s in the presence of out-of-phase thoracoabdominal effort or as a fall in oronasal airflow for ≥10 s with out-of-phase thoracoabdominal movement associated with a ≥4% fall in SpO2. CSA was defined as an absence of oronasal airflow during sleep for ≥10 s associated with absent respiratory effort or any reduction in oronasal airflow for ≥10 s associated with in-phase thoracoabdominal movement and a ≥4% fall in SpO2. MSA was defined as an event which begins as CSA and develops into the obstructive form in parallel with a ≥4% fall in SpO2. A hypopnea was defined as a decrement in airflow ≥50% but <90% from baseline for ≥10 seconds and a ≥4% fall in SpO2. The oxygen desaturation index was defined as the total number of a ≥4% fall in SpO2 per hour of sleep. The average oxygen saturation value was calculated over all valid SpO2 values. The average duration of desaturation events, the maximum desaturation from baseline and maximum duration of desaturation events were also calculated.
2.3. Data Analyses
The data were analyzed with SPSS version 21.0. Descriptive statistics, ANOVA with post-hoc Bonferroni comparisons and multinomial logistic regression were performed to address the study aims if testing for normal distribution (Kolmogorov-Smirnov) passed. Quantitative variables values were expressed as mean with 95% confidence interval. The chi-squared test was used to analyze the association between the categorical variables.
Direct effects of sleep and respiratory variables between NYHA functional classes were analyzed using general linear models (GLM) adjusted by gender, age, body mass index, arterial hypertension, myocardial infarction, diabetes.
The adjusted multivariate analysis was performed with controlled covariates for gender, age, body mass index, arterial hypertension, myocardial infarction and diabetes. Sleep apnea and oxygen desaturation events per hour were initially categorized with apnea-hypopnea index (events/h) as: none (≤5.0), mild (5.1 to 15.0), moderate (15.1 to 30.0) and severe (≥30.0). Multivariate logistic regression models were used to identify odds ratios (OR) between NYHA functional class and severity apnea-hypopnea and severity oxygen desaturation levels. The adjusted odds ratios results of multinomial logistic regression provide comparison the three NYHA functional class patient groups for: 1) NYHA class II patients versus NYHA class I patients and 2) NYHA class III patients versus NYHA class I patients. Models were adjusted for covariates of gender, age, body mass index, arterial hypertension, myocardial infarction, diabetes. A value of P < 0.05 and less was considered significant for all comparisons.
3. RESULTS
3.1. Demographic Characteristics
The mean age of the 3017 patients was 59.7 (SD 9.9) years (Table 1). The patients were older in groups with higher NYHA functional class (P < 0.001). Approximately one-fourth there was women in the total group as well as in all groups with different NYHA functional class. A body mass index significantly (P < 0.001) increased in parallel with worsening of NYHA functional class reaching the highest values in patients with NYHA functional class III. A total of 2065 (68.4%) patients had myocardial infarction and 286 (9.5%) had diabetes mellitus. The patient groups with different NYHA functional class statistically significantly differ in cases of myocardial infarction, arterial hypertension and diabetes (P < 0.001). Myocardial infarction and diabetes were characteristic for NYHA class III patients; while arterial hypertension for NYHA class II patients (P < 0.001).
A higher systolic arterial blood pressure was observed in NYHA functional class III patients, as compared with NYHA class I patients (P < 0.01). There were no significant differences in diastolic arterial blood pressure values in different groups distributed according NYHA functional class. Left ventricle ejection fraction was 46.8% in the total group and a statistically significant (P < 0.001) reduction in parallel with worsening of heart failure in higher NYHA functional class groups was observed.
3.2. Sleep Variables
Sleep latency time increased in parallel with higher NYHA functional class; however a statistically significant (P < 0.001) increase was observed in NYHA functional class III patients, as compared with NYHA functional class I patients (Table 1). The total sleep time was statistically significantly decreased in NYHA functional class III patients, as compared with NYHA functional class II and NYHA functional class I patients.
A statistically significant (P < 0.001) decrease in sleep efficiency was observed in parallel with the worsening of NYHA functional class reaching 83.5% in patients with NYHA class III because of an increase (P < 0.001) of wakefulness after sleep onset up till 16.1%.
The sleep architecture was mostly disturbed in patients with NYHA functional class III (Table 1). There was observed a gradual increase (P < 0.001) of stage 1 and a gradual decrease (P < 0.001) of stages 3-4 and REM sleep with worsening of NYHA functional class. Only stage 2 did not differ among different NYHA functional class patients. The highest number of body movements was observed in NYHA functional class III patients; however statistically significant difference (P < 0.001) was only between patients of NYHA functional class III and NYHA functional class I patient groups.
General linear model analysis confirmed that the significant differences remain for all sleep variables in different NYHA functional class patients’ groups except for sleep latency time, total sleep time, stage 2 and body movements.
3.3. Respiratory Events
Patients had none (≤5) (n = 1796 (59.5%)), mild (5.1 to 15.0) (n = 709 (23.5%)), moderate (15.1 to 30) (n = 320 (10.6%)), and severe (>30) (n = 192 (6.4%)) (Table 1).
In total group of CHD patients the average of AHI was 8.3 event/h. Central sleep apneas (1.32 events/h) were observed more frequently (P < 0.001), as compared with obstructive (1.06 events/h) or mixed (0.45 events/h) sleep apneas. A statistically significant (P < 0.001) increase of AHI from 6.5 events/h in NYHA functional class I patients to 8.0 events/h in NYHA functional class II, and 12.1 events/h in NYHA functional class III patients was observed. The changes of number of central, obstructive or mixed sleep apneas were in the same direction as of AHI in different groups distributed according to NYHA functional class. The patients with NYHA functional class III, as compared with patients in NYHA functional class II or NYHA functional class I, demonstrated the highest number of different apneas-hypopneas (P < 0.001).
Oxygen desaturation index followed the changes of AHI in all patient groups: from 7 events/hour in NYHA functional class I patients till 7.4 events/hour in NYHA class II, and 12.4 events/h in NYHA class III patients. Statistically significant differences were observed between NYHA class III patients and NYHA class II or

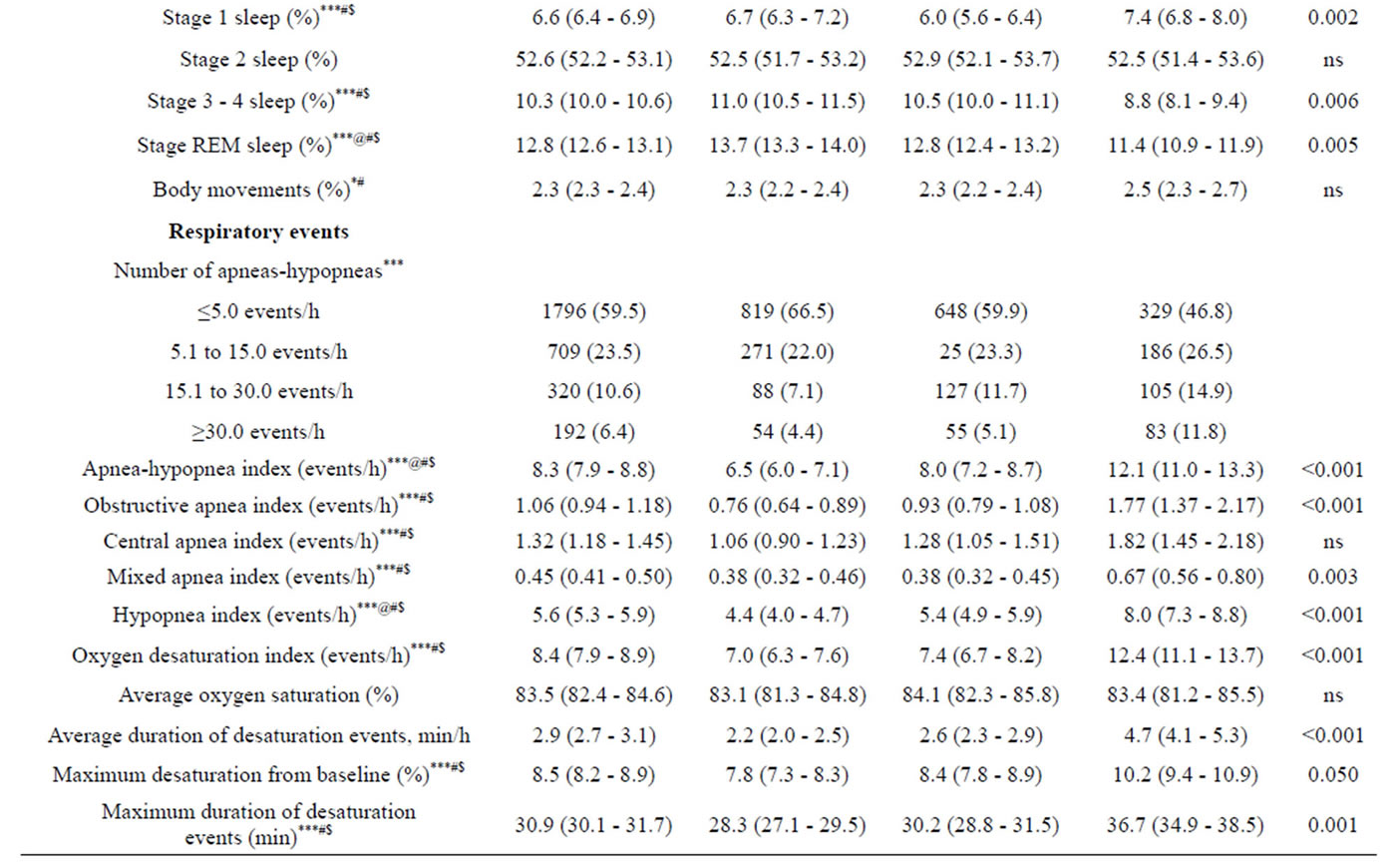
Table 1. Comparison of demographic and clinical characteristics, sleep variables and respiratory events in heart failure patients with different NYHA functional class.
All values mean (95% confidence interval)/N (%). Overall tests: *P < 0.05; **P < 0.01; ***P < 0.001. Post hoc tests (Bonferroni) P < 0.05: @I-II; #I-III; $II-III. aadjusted by gender, age, BMI, arterial hypertension, myocardial infarction, diabetes.
NYHA class I patients (P < 0.001). The average oxygen saturation was 83.5% in total group and did not differ significantly among all three patient groups. However, maximum desaturation drop from the baseline was observed in NYHA functional class III patients (10.2%), as compared with NYHA class II (8.4%, P < 0.05) and NYHA class I (7.8%, P < 0.001) patients. Maximum duration of desaturation events demonstrated the similar changes.
An analysis of respiratory variables in CHD patients’ groups when adjusting for gender, age, body mass index, arterial hypertension, myocardial infarction, and diabetes demonstrated that statistically significant differences of variables in different NYHA functional class groups remain the same, except the number of central apneas and average oxygen saturation.
3.4. Relation between Respiratory Events and Heart Failure
Multivariate logistic regression analysis adjusted for all covariates revealed that patients with NYHA functional class II had 1.41 (95% CI = 1.04 - 1.91) times increased odds of having moderate AHI (between 15.1 to 30.0 events per hour) (Table 2). Patients with NYHA functional class III demonstrated the highest odds for moderate (OR = 1.81; 95% CI = 1.29 - 2.53) and severe (OR = 2.19; 95% CI = 1.47 - 3.27) AHI. Oxygen desaturation index was associated with increased odds for severe desaturation (OR = 1.24; 95% CI = 1.24 - 2.63) for all covariates only in NYHA functional class III (Table 3).
4. DISCUSSION
SDB represents one of the major public health problems affecting many individuals worldwide. The prevalence of SDB in the general community was defined by large epidemiological studies. The prevalence ranged from 9% in men and 4% in women (602 subjects, aged
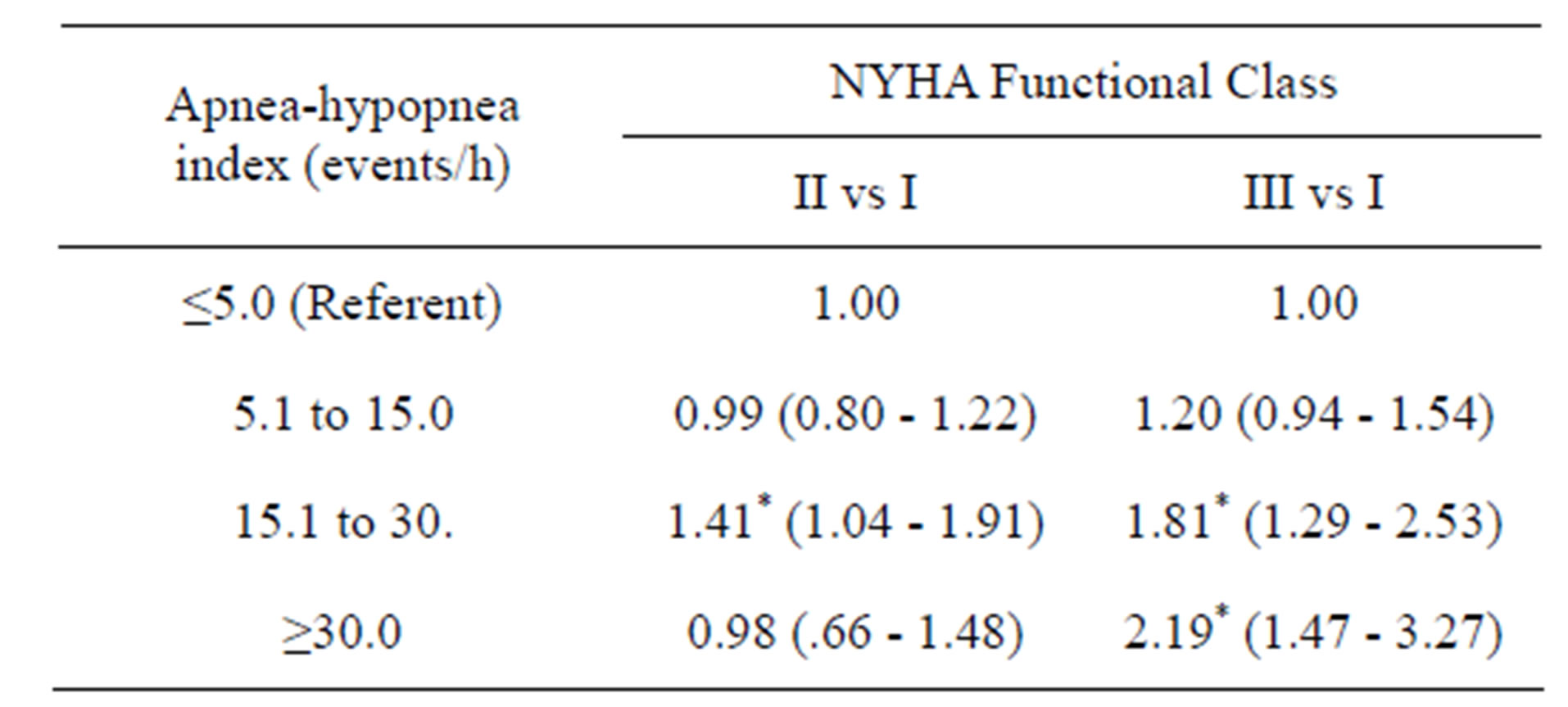
Table 2. Multinomial logistic regression of NYHA functional class patients’groups by sleep apnea events.
*P < 0.05. Results: adjusted odds ratio (95% confidence interval), R2 = 0.18. Multinomial logistic regression was used, considering I NYHA Functional class as the reference category. Model adjusted for gender, age, BMI, arterial hypertension, myocardial infarction, diabetes.
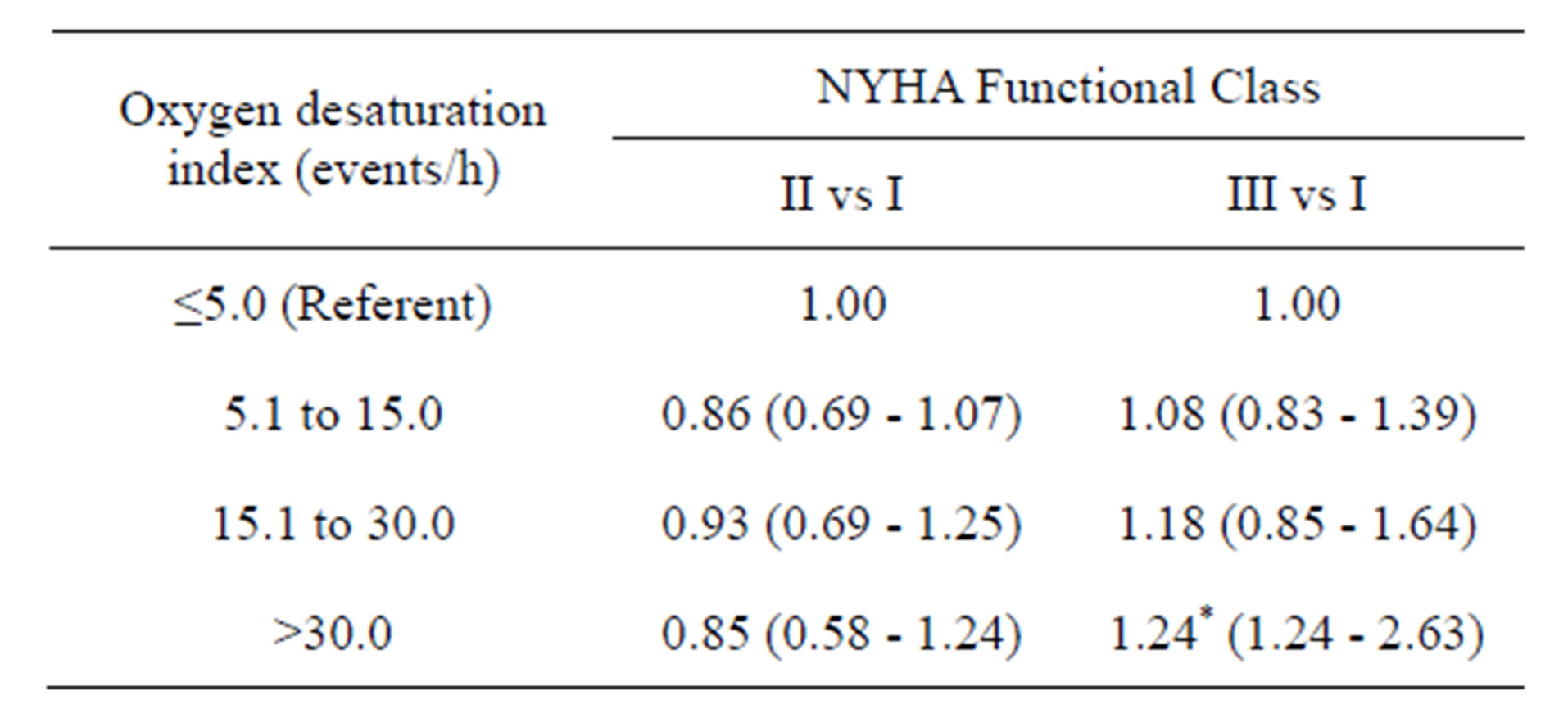
Table 3. Multinomial logistic regression of NYHA functional class patients’ groups by oxygen desaturation events.
*P < 0.05. Results: adjusted odds ratio (95% confidence interval), R2 = 0.18. Multinomial logistic regression was used, considering I NYHA Functional class as the reference category. Model adjusted for gender, age, body mass index, arterial hypertension, myocardial infarction, diabetes.
30 - 60 years, AHI ≥ 15) in the Wisconsin Sleep Study Cohort [3] to 3.3% in men (741 subjects, aged 20 - 100 years, AHI ≥ 10) [22] and 1.2% in women (1000 subjects, aged 20 - 100 years, AHI ≥ 10) [23] in the Southern Pennsylvanian Study Cohort. In the large Sleep Heart Health Study, the overall prevalence rate was 18% (5615 subjects, 53% female, AHI ≥ 15), with 2:1 male predominance (prevalence of 25% in men and 11% in women) and men with severe obstructive sleep apnea have a 58% higher adjusted risk of incident HF than men without OSA [24].
SDB may be considered as a public health problem because of clinical consequences for the patient as sleep apnea syndrome is an increasingly common chronic condition that affects many diseases as CHD, hypertension, diabetes etc [6-10,25]. This is in line with our results showing that patients with higher NYHA functional class have more cases of myocardial infarction and diabetes as well as more apneas-hypopneas.
Mechanisms by which SDB may aggravate CHD include sympathetic nervous system activation that results from intermittent hypoxemia and hypercapnia during sleep, repeated episodes of hypoxemia and reoxygenation evoke hypoxic and oxidative stress which is the main factor causing systemic inflammation, endothelial dysfunction, increased production of vasoactive substances, and insulin resistance, with resultant hypertension, hyperlipidemia, and diabetes mediating the cardiovascular consequences [26,27].
The major effect of SDB on cardiovascular function is an intermittent hypoxia during sleep activating negative molecular mechanisms, sympathetic activity and increasing arterial blood pressure [28,29]; however, statistically significant increase of systolic arterial pressure is observed only in NYHA functional class III patients displaying moderate HF; while diastolic blood pressure values remain the same in all patient groups. We speculate that other mechanisms, but not elevated arterial blood pressure, may play the main role in pathogenesis of SDB in HF patients.
The two main types of SDB, obstructive and central sleep apneas, are determined by different mechanisms. In obstructive sleep apnea, there is primarily a failure to maintain airway patency resulting in obstruction, while OSA is predominantly due to the instability of ventilatory control systems, accentuated when feedback loops become abnormal, as in HF. This explains why central sleep apneas are more frequent in HF patients. The most important pathophysiological mechanisms responsible for central sleep apneas in HF [30] are a hypocapnia-induced apnoeic threshold during sleep [30], in combination with enhanced central chemoreceptor sensitivity [31] and elevated pulmonary capillary wedge pressure [32].
In our study we found a prevalence of central sleep apneas over obstructive apneas in patients with worsening of NYHA functional class. The reason for higher rates of central sleep apneas may be explained by higher rate of HF in those patients. The higher proportion of CHD, myocardial infarction, reduced left ventricle ejection fraction and lower rates of arterial hypertension in NYHA class II and class III patient groups confirm that central sleep apneas may be associated with primarily ischemic versus hypertensive etiology of HF. The reduction of left ventricle ejection fraction and an increase of number of central apneas with the worsening of HF support this explanation. The previous findings also demonstrate that patients with systolic dysfunction had signifycant central sleep apneas [33,34]. Other studies have documented a high prevalence of OSA in patients with systolic [10,35-38.] as well as diastolic [39] HF. Therefore, alterations in cardiac function during sleep may influence apnea type in HF patients.
Pathophysiological studies demonstrated that in patients with HF, the shift from OSA to CSA is associated with a reduction in carbon dioxide partial pressure (pCO2) related to an overnight deterioration in cardiac function because of the concurrent lengthening of circulation time [40,41]. Further studies confirmed that the characteristics of sleep apnea can change in HF patients with obstructive or central sleep apnea when periodic breathing happens because of modifications in wake and sleep pCO2, the length of periodic breathing cycle, lung to finger circulation time, and possibly by impaired heart function [42]. Circulation time increases in HF patients due to reduced cardiac output and results in delay in central chemoreceptor sensing of alterations in arterial pCO2 [43]. These changes are associated with an alteration in apnea type and lead to appearance of central apneas.
There is evidence of an association between sleep disturbances and CHD [44], and OSA has been demonstrated to increase the risk of CHD [5]. Sleep disturbances [45,46.] and SDB [10,47] are associated with manifest HF. The sleep variables in our study a significantly differ among the patient groups with different NYHA functional class; being mostly disturbed in NYHA class III patients displaying moderate HF. We have found statistically significantly increased stage 1 and wakefulness after sleep onset and significantly decreased stages 3-4 and REM sleep without statistically significant modifications in total sleep time in patients with higher NYHA class. Therefore we suggest that both SDB and disturbed sleep variables independently significantly correlate with manifestation of HF.
5. CONCLUSIONS
The study demonstrated that SDB is more common in CHD patients with higher NYHA functional class. The prevalence of central sleep apneas against obstructive was observed in patients with mild and moderate HF. The number of central sleep apneas was strongly related to the severity of HF.
Disturbed sleep architecture was observed in CHD patients with higher NYHA functional class. A gradual increase of stage 1 and wakefulness after sleep onset and a decrease of sleep stages 3-4 and REM sleep as well as a diminution of sleep efficiency with worsening of HF were observed.
6. ACKNOWLEDGEMENTS
This research was funded by a grant (LIG-03/2012) from the Research Council of Lithuania. This research was performed in cooperation with the Behavioral Medicine Institute of the Lithuanian University of Health Sciences.
REFERENCES
- Young, T., Finn, L., Peppard, P.E., Szklo-Coxe, M., Austin, D., Nieto, F.J., Stubbs, R. and Hla, K.M. (2008) Sleep disordered breathing and mortality: Eighteen-year follow-up of the wisconsin sleep cohort. Sleep, 31, 1071- 1078.
- Punjabi, N.M., Caffo, B.S., Goodwin, J.L., Gottlieb, D.J., Newman, A.B., O’Connor, G.T., Rapoport, D.M., Redline, S., Resnick, H.E., Robbins, J.A., Shahar, E., Unruh, M.L. and Samet J.M. (2009) Sleep-disordered breathing and mortality: A prospective cohort study. PLOS Medicine, 6, E1000132. doi:10.1371/journal.pmed.1000132
- Young, T., Palta, M., Dempsey, J., Skatrud, J., Weber, S. and Badr, S. (1993) The occurrence of sleep-disordered breathing among middle-aged adults. The New England Journal of Medicine, 328, 1230-1235. doi:10.1056/NEJM199304293281704
- Young, T., Peppard, P.E. and Gottlieb, D.J. (2002) Epidemiology of obstructive sleep apnea: A population health perspective. American Journal of Respiratory and Critical Care Medicine, 165, 1217-1239. doi:10.1164/rccm.2109080
- Marin, J.M., Carrizo, S.J., Vicente, E. and Agusti, A.G.N. (2005) Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: An observational study. The Lancet, 365, 1046-1053.
- Kiely, J.L. and McNicholas, W.T. (2000) Cardiovascular risk factors in patients with obstructive sleep apnoea syndrome. European Respiratory Journal, 16, 128-133. doi:10.1034/j.1399-3003.2000.16a23.x
- Parish, J.M. and Somers V.K. (2004) Obstructive sleep apnea and cardiovascular disease. Mayo Clinic Proceedings, 79, 1036-1046. doi:10.4065/79.8.1036
- Sánchez-de-la-Torre, M., Campos-Rodriguez, F. and Barbé, F. (2013) Obstructive sleep apnoea and cardiovascular disease. The Lancet Respiratory Medicine, 1, 61-72. doi:10.1016/S2213-2600(12)70051-6
- Bradley, T.D. and Floras, J.S. (2003) Sleep apnea and heart failure: Part II: Central sleep apnea. Circulation, 107, 1822-1826. doi:10.1161/01.CIR.0000061758.05044.64
- Javaheri, S., Parker, T.J., Liming, J.D., Corbette, W.S., Nishiyama, H., Wexler, L. and Roselle, G.A. (1998) Sleep apnea in 81 ambulatory male patients with stable heart failure: Types and their prevalences, consequences, and presentations. Circulation, 97, 2154-2159. doi:10.1161/01.CIR.97.21.2154
- Sin, D.D., Logan, A.G., Fitzgerald, F.S., Liu, P.O. and Bradley, T.D. (2000) Effects of continuous positive airway pressure on cardiovascular outcomes in heart failure patients with and without cheyne-stokes respiration. Circulation, 102, 61-66. doi:10.1161/01.CIR.102.1.61
- Lanfranchi, P.A., Braghiroli, A., Bosimini, E., Mazzuero, G., Colombo, R.M.S., Donner, C.F. and Giannuzzi, P. (1999) Prognostic value of nocturnal cheyne-stokes respiration in chronic heart failure. Circulation, 99, 1435- 1440. doi:10.1161/01.CIR.99.11.1435
- Peker, Y., Hedner, J., Norum, J., Kraiczi, H. and Carlson, J. (2002) Increased incidence of cardiovascular disease in middle-aged men with obstructive sleep apnoea. American Journal of Respiratory and Critical Care Medicine, 166, 159-165. doi:10.1164/rccm.2105124
- Gami, A., Howard, D., Olson, E. and Somers, V. (2005) Day-night pattern of sudden death in obstructive sleep apnoea. The New England Journal of Medicine, 352, 1206-1214. doi:10.1056/NEJMoa041832
- Coughlin, S., Mawdsley, L., Mugarza, J., Calverley, P. and Wilding, J. (2004) Obstructive sleep apnoea is independently associated with an increased prevalence of metabolic syndrome. European Heart Journal, 25, 735- 741. doi:10.1016/j.ehj.2004.02.021
- Milleron, O., Pilliere, R., Foucher, A., de Roquefeuil, F., Aegerter, P., Jondeau, G., Raffestin, B.G. and Dubourg O. (2004) Benefits of obstructive sleep apnoea treatment in coronary artery disease: A long-term follow-up study. European Heart Journal, 25, 728-734. doi:10.1016/j.ehj.2004.02.008
- Lanfranchi, P., Somers, V., Braghiroli, A., Corra, U., Eleuteri, E. and Giannuzzi, P. (2003) Central sleep apnoea in left ventricular dysfunction. Prevalence and implications for arrhythmic risk. Circulation, 107, 727-732. doi:10.1161/01.CIR.0000049641.11675.EE
- Hanly, P. and Zuberi-Khokhar, N. (1996) Increased mortality associated with cheyne-stokes respiration in patients with congestive heart failure. American Journal of Respiratory and Critical Care Medicine, 153, 272-276. doi:10.1164/ajrccm.153.1.8542128
- McNicholas, W.T, Bonsigore, M.R. and Management Committee of EU COST ACTION B26. (2007) Sleep apnoea as an independent risk factor for cardiovascular disease: Current evidence, basic mechanisms and research priorities. European Respiratory Journal, 29, 156- 178. doi:10.1183/09031936.00027406
- The Criteria Committee of the New York Heart Association (1994) Functional capacity and objective assessment. In: Dolgin M., Ed., Nomenclature and Criteria for Diagnosis of Diseases of the Heart and Great Vessels. 9th Edition, Little, Brown and Company, Boston, 253-255.
- Rechtschaffen, A. and Kales, A. (1968) A manual of standardized terminology, techniques and scoring systems for sleep stages of human subjects. Publication No. 204, National Institute of Health, Washington.
- Bixler, E.O., Vgontzas, A.N., Ten Have, T., Tyson, K. and Kales, A. (1998) Effects of age on sleep apnea in men: I. Prevalence and severity. American Journal of Respiratory and Critical Care Medicine, 157, 144-148. doi:10.1164/ajrccm.157.1.9706079
- Bixler, E.O., Vgontzas, A.N., Lin, H.M., Ten Have, T., Rein, J., Vela-Bueno, A. and Kales, A. (2001) Prevalence of sleep-disordered breathing in women: Effects of gender. American Journal of Respiratory and Critical Care Medicine, 163, 608-613. doi:10.1164/ajrccm.163.3.9911064
- Young, T., Shahar, E., Nieto, F.J., Redline, S., Newman, A.B., Gottlieb, D.J., Walsleben, J.A., Finn, L., Enright, P., Samet, J.M. and Sleep Heart Health Study Research Group (2002) Predictors of sleepdisordered breathing in community-dwelling adults: The sleep heart health study. Archives of Internal Medicine, 162, 893-900. doi:10.1001/archinte.162.8.893
- Jaffe, L.M., Kjekshus, J. and Gottlieb, S.S. (2013) Importance and management of chronic sleep apnoea in cardiology. European Heart Journal, 34, 809-815. doi:10.1093/eurheartj/ehs046
- Somers, V.K., White, D.P., Amin, R., Abraham, W.T., Costa, F., Culebras, A., Daniels, S., Floras, J.S., Hunt, C.E., Olson, L.J., Pickering, T.G., Russell, R., Woo, M. and Young, T. (2008) Sleep apnea and cardiovascular disease: An American Heart Association/American College of Cardiology Foundation scientific statement. Circulation, 118, 1080-1111. doi:10.1161/CIRCULATIONAHA.107.189420
- McNicholas, W.T. (2009) Chronic obstructive pulmonary disease and obstructive sleep apnea: Overlaps in pathophysiology, systemic inflammation, and cardiovascular disease. American Journal of Respiratory and Critical Care Medicine, 180, 692-700. doi:10.1164/rccm.200903-0347PP
- Peppard, P.E., Young, T., Palta, M., Skatrud, J. (2000) Prospective study of the association between sleep-disordered breathing and hypertension. The New England Journal of Medicine, 342, 1378-1384. doi:10.1056/NEJM200005113421901
- Punjabi, N.M., Sorkin, J.D., Katzel, L., Goldberg, A., Schwartz, A. and Smith, P.L. (2002) Sleep-disordered breathing and insulin resistance in middle aged and overweight men. American Journal of Respiratory and Critical Care Medicine, 165, 677-682. doi:10.1164/ajrccm.165.5.2104087
- Javaheri, S. (2005) Central sleep apnea in congestive heart failure: Prevalence, mechanisms, impact, and therapeutic options. Seminars in Respiratory and Critical Care Medicine, 26, 44-55. doi:10.1055/s-2005-864206
- Javaheri, S. (1999) A mechanism of central sleep apnea in patients with heart failure. The New England Journal of Medicine, 341, 949-954. doi:10.1056/NEJM199909233411304
- Solin, P., Bergin, P., Richardson, M., Kaye, D.M., Walters, E.H. and Naughton, M.T. (1999) Influence of pulmonary capillary wedge pressure on central apnea in heart failure. Circulation, 99, 1574-1579. doi:10.1161/01.CIR.99.12.1574
- Redeker, N.S., Muench, U., Zucker, M.J., Walsleben, J., Gilbert, M., Freudenberger, R., Chen, M., Campbell, D., Blank, L., Berkowitz, R., Adams, L. and Rapoport, D.M. (2010) Sleep disordered breathing, daytime symptoms, and functional performance in stable heart failure. Sleep, 33, 551-560.
- Ferrier, K., Campbell, A., Yee, B., Richards, M., O’Meeghan, T., Weatherall, M. and Neill, A. (2005) Sleep-disordered breathing occurs frequently in stable outpatients with congestive heart failure. Chest, 128, 2116-2122. doi:10.1378/chest.128.4.2116
- Javaheri, S. (1996) Central sleep apnea-hypopnea syndrome in heart failure: Prevalence, impact, and treatment. Sleep, 19, S229-S231.
- Javaheri, S. (2006) Sleep disorders in systolic heart failure: A prospective study of 100 male patients. The final report. International Journal of Cardiology, 106, 21-28. doi:10.1016/j.ijcard.2004.12.068
- Sin, D.D., Fitzgerald, F., Parker, J.D., Newton, G., Floras, J.S. and Bradley, T.D. (1999) Risk factors for central and obstructive sleep apnea in 450 men and women with congestive heart failure. American Journal of Respiratory and Critical Care Medicine, 160, 1101-1106. doi:10.1164/ajrccm.160.4.9903020
- Wang, H., Parker, J.D., Newton, G.E., Floras, J.S., Mak, S., Chiu, K.L., Ruttanaumpawan, P., Tomlinson, G. and Bradley, T.D. (2007) Influence of obstructive sleep apnea on mortality in patients with heart failure. Journal of the American College of Cardiology, 49, 1625-1631. doi:10.1016/j.jacc.2006.12.046
- Arias, M.A., Garcia-Rio, F., Alonso-Fernandez, A., Mediano, O., Martinez, I. and Villamor, J. (2005) Obstructive sleep apnea syndrome affects left ventricular diastolic function: Effects of nasal continuous positive airway pressure in men. Circulation, 112, 375-383. doi:10.1161/CIRCULATIONAHA.104.501841
- Tkacova, R., Niroumand, M., Lorenzi-Filho, G. and Bradley, T.D. (2001) Overnight shift from obstructive to central apneas in patients with heart failure: Role of PCO2 and circulatory delay. Circulation, 103, 238-243. doi:10.1161/01.CIR.103.2.238
- Tkacova, R., Wang, H. and Bradley, T.D. (2006) Nightto-night alterations in sleep apnea type in patients with heart failure. Journal of Sleep Research, 15, 321-328. doi:10.1111/j.1365-2869.2006.00528.x
- Wang, H.Q., Chen, G., Li, J., Hao, S.M., Pang, J.N., Gu, X.S. and Fu, X.H. (2009) Changes of the characteristics of sleep apnea in heart failure patients and the associated factors [Article in Chinese]. ZhonghuaJie He He Hu Xi Zazhi, 32, 598-602.
- Hall, M.J., Xie, A., Rutherford, R., Ando, S., Floras, J.S. and Bradley, T.D. (1996) Cycle length of periodic breathing in patients with and without heart failure. American Journal of Respiratory and Critical Care Medicine, 154, 376-381. doi:10.1164/ajrccm.154.2.8756809
- Schwartz, S.W., Cornoni-Huntley, J., Cole, S.R., Hays, J.C., Blazerm, D.G. and Schocken, D.D. (1998) Are sleep complaints an independent risk factor for myocardial infarction? Annals of Epidemiology, 8, 384-392. doi:10.1016/S1047-2797(97)00238-X
- Katz, D.A. and McHorney, C.A. (1998) Clinical correlates of insomnia in patients with chronic illness. Archives of Internal Medicine, 158, 1099-1107. doi:10.1001/archinte.158.10.1099
- Erickson, V.S., Westlake, C.A., Dracup, K.A., Woo, M.A. and Hage, A. (2003) Sleep disturbance symptoms in patients with heart failure. AACN Clinical Issues, 14, 477- 487. doi:10.1097/00044067-200311000-00009
- Shahar, E., Whitney, C.W., Redline, S., Lee, E.T., Newman, A.B., Nieto, F.J., O’Connor, G.T., Boland, L.L., Schwartz, J.E. and Samet, J.M. (2001) Sleep-disordered breathing and cardiovascular disease: Cross-sectional results of the sleep heart health study. American Journal of Respiratory and Critical Care Medicine, 163, 19-25. doi:10.1164/ajrccm.163.1.2001008

