Health
Vol. 4 No. 3 (2012) , Article ID: 18332 , 4 pages DOI:10.4236/health.2012.43022
Prenatal breastfeeding intervention program to increase breastfeeding duration among low income women
![]()
Department of Maternal and Child Nursing, King Saud University, Riyadh, Kingdom of Saudi Arabia; whatamleh@ksu.edu.sa
Received 26 December 2011; revised 28 January 2012; accepted 9 February 2012
Keywords: Breastfeeding; Self-Efficacy; Intervention; Low Income
ABSTRACT
Extensive research confirms the nutritional, economic, biomedical, immunological, and psychological advantages of breast milk. Despite the clear benefits of breastfeeding to mother and infant, breastfeeding rates today continue to remain below the recommended levels in the United States, most notably among low-income mothers. One factor that plays a role in breastfeeding success and may be modifiable by nursing intervention is maternal self-efficacy. This study aimed to increase the breast-feeding duration through an intervention based on Dennis’s Breastfeeding Self-Efficacy Theory. A quasiExperimental design was used to test the effect of the intervention program on duration of breastfeeding. A convenience sample of 37 low-income women was recruited from two rural prenatal clinics in the Midwest. Data were collected using the Breastfeeding Self-Efficacy Scale (BSES) and a demographic profile. Women were contacted by telephone at two and six weeks postpartum to determine if they were still breastfeeding and to complete the BSES. The women who were assigned to a breast-feeding self-efficacy intervention showed significantly greater increases in breast-feeding duration and selfefficacy than did the women in the control group. The results of this study suggest that the onehour of breastfeeding intervention program during the prenatal period may increase the duration of breastfeeding in low-income women who intend to breastfeed. This study supports the literature which found that prenatal education and postpartum support are important to the outcome of breastfeeding.
1. INTRODUCTION
Breastfeeding has long been recognized as the preferred method of feeding in the first year of life [1]. Extensive research confirms the nutritional, economic, biomedical, immunological, and psychological advantages of breast milk. Despite the clear benefits of breastfeeding to mother and infant, breastfeeding rates today continue to remain below the recommendation levels in the United States (US), most notably among low-income mothers. The decline of breastfeeding in the United States has been most marked among low-income women. It is reported that 38.9% of low-income women initiate breastfeeding in the hospital compared to 66.1% of women from middleand high-income groups [2]. In addition; rates of exclusive breastfeeding are even lower in low-income populations, minority/racial groups, and adolescents [3].
When women initiate breastfeeding, the majority of breastfed infants are weaned before they are three months of age. A number of variables have been associated with this early weaning. These variables are sometimes classified as modifiable or non-modifiable. The evidence has demonstrated the impact of non-modifiable factors, such as maternal age, parity, race/ethnicity, and economic status, on breastfeeding. Breastfeeding rates have been found to be higher among women who are Caucasian, older, with higher education, and not participating in the Women, Infants [4-9]. Modifiable factors such as maternal attitudes and self-efficacy demonstrate a positive relationship with continued breastfeeding and some evidence exists that these variables may be modifiable to impact the breastfeeding experience [10-16]. One factor that plays a role in breastfeeding duration and may be modifiable by nursing intervention is maternal self-efficacy [11,12,15]. Past studies suggest that maternal confidence in breastfeeding affects intended duration of breastfeeding and that both are predictor of breastfeeding success [12,15,17]. Specifically, woman with a higher perceived self-efficacy for breastfeeding tend to initiate breastfeeding and persist even through challenges, whereas a woman with a lower perceived self-confidence may decide not even to initiate breastfeeding or wean prematurely due to lack of confidence or effective coping skills [17-20].
The importance of breastfeeding education in supporting breastfeeding has not been clearly demonstrated in past research. Some studies identified education as a factor related to breastfeeding success [21,22], while other studies have reported nonsignificant results of education’s effect on breastfeeding success [23]. The majority of current research indicates that maternal breastfeeding confidence is positively associated with breastfeeding duration [12, 15,17]. The author suggests that maternal breastfeeding confidence plays a major role in helping mothers have a successful breastfeeding experience, leading to breastfeeding satisfaction and increase breastfeeding duration. Studies on prenatal support and education are often lacking in the provision of consistent information and technique demonstration and practice.
The nursing intervention that was used in this study is flexible enough to meet the mother needs. It includes prenatal preparation and used all four sources of information to enhance women’s self-efficacy judgment. Considering women’s early discharge from the hospital, the first two weeks after delivery are the time of professional unavailability, and many breastfeeding women are left without assistance. This intervention continued to follow the women up to six weeks postpartum to provide consistent, structured information, techniques demonstration, practice and caring supportive attitude. Education aimed to increase a women’s self-efficacy will provide more theoretically sound and empirically verifiable information on self-efficacy effect on breastfeeding behavior.
The purpose of the this study is to test the efficacy of the Breastfeeding Self-Efficacy Intervention Program (BSEIP), which is based on Dennis’s (1999) breastfeeding self-efficacy theory, to increase breastfeeding duration.
The following hypotheses will be tested:
1) Women who receive the Breastfeeding Self-Efficacy Intervention program (BSEIP) prenatally will report higher breastfeeding self-efficacy on the Breastfeeding SelfEfficacy Scale (BSES) at two and six weeks postpartum than women who do not receive the BSEIP prenatally.
2) Women who received BSEIP prenatally will breastfeed their infants significantly longer than women who do not receive the BSEIP prenatally.
2. METHOD
2.1. Design
The research design chosen for this study is a quasiexperimental with repeated measures to test the effect of a breastfeeding self-efficacy intervention program (BSEIP) on breastfeeding self-efficacy and duration. The design was selected to estimate a treatment effect by comparing two groups of individuals, one group that receives the treatment (Experimental Group), and the second group does not receive the treatment (Control Group).
2.2. Setting and Participants
The target population consisted of pregnant women who had not previously breastfed a child longer than two weeks, and were between 28 and 38 weeks of pregnancy at the time of enrollment. The women received their prenatal care either at the Warren County Health Clinic (Clinic A) or at the Middletown Regional Hospital prenatal clinic (Clinic B). Both prenatal clinics are located in the same geographic area outside a large metropolitan area in the state of Ohio, and each serves predominately low-income, non-Hispanic White women (90% White, 5% African American, 3% Hispanic, and 2% others). The majority of women served by these clinics are low-income: 75% are eligible for Medicaid. Currently, there is no breastfeeding intervention program available at either of the two clinics.
2.3. Data Collection
Demographic data was collected using a tool developed for this study by the investigator. Subjects were asked to give information on income, education, number of children, marital status, race, employment, intention to breastfeed, and pregnancy history.
Breastfeeding Self-Efficacy was measured using the Breastfeeding Self-Efficacy Scale (BSES) [18]. The BSES is a 33-item self-report instrument that assesses breastfeeding self-efficacy expectancies in new mothers [18]. The initial Cronbach’s Alpha coefficient for BSES was .96 with 73% of all corrected items total correlations ranging from 0.30 to 0.70. The BSES scores predicted which women would still be breastfeeding at six weeks postpartum (f = 9.89, P < 0.001). All items are preceded by the phrase “I can always” and anchored with a 5-point likert scale, where 1 = not at all confident and 5 = very confident. Items are summed to produce an overall score ranging from 33 to 165, with higher scores indicating higher levels of breastfeeding self-efficacy [18-20].
Breastfeeding duration was measured as the number of days from the first to last breastfeeding through the final data collection on the 42nd day. Because the six week postpartum follow-up call took place within two weeks of this time, duration of breastfeeding could be reported from 0 to more than 42 days. For the purposes of this study, the maximum breastfeeding duration was cut off at 42 days. In order to assess breastfeeding status, a specific script was designed to collect data during the follow–up telephone calls. Mothers were asked if they were still breastfeeding and depending on their answers, specific questions were asked.
2.4. Procedure
This study was approved by the University of Cincinnati Institutional Review Board. Women who agreed to participate were asked to sign the consent form, complete the demographic prenatal form and complete the BSES. The researcher maintained contact with all participants at their respective institution as their due dates drew near. All participants were contacted at two weeks following the birth of their infant by telephone or in person to determine breastfeeding status and to complete the BSES. If the mothers were still breastfeeding at two weeks postpartum, they were contacted again by telephone or in person at six weeks postpartum to determine if they were still breastfeeding, and, if not, when they stopped breastfeeding.
Subjects assigned to the Experimental Group were asked to meet the researcher two hours prior to their next prenatal appointment (after recruitment) to take part in the prenatal breastfeeding class. The BSEIP occurred during several time periods: the prenatal class and at two follow-up telephone calls—at one week and at two weeks postpartum. The nursing actions for the BSEIP included: education, assessment, encouragement/support, referral, physical assistance, and availability (by telephone or in person). Participants in the Experimental Group watched a 15-minute video about breastfeeding during the prenatal class, discussed normal physiological changes that occur during the postpartum period, and received explanations of how to evaluate milk supply and interpret infant cues.
Subjects were sent home with a written copy of the BSEIP that discussed the four steps of breastfeeding: positioning, offering the breast, effective sucking, and breaking suction. Research has demonstrated that these behaviors are important to the success and duration of breastfeeding [9,22].
2.5. Breastfeeding Self-Efficacy Intervention Program (BSEIP)
The intervention program for this study was based on the four major sources of information that provide information for cognitive processing in the development of a self-efficacy judgment, namely, performance accomplishments; vicarious experiences; verbal persuasion; and physiological responses. Nursing intervention developed to manipulate these sources of information to enhance self-efficacy judgments of women who intended to breastfeed and to promote successful breastfeeding (see Tables 1 and 2).
3. RESULTS
3.1. Sample
A convenience sample of 37 women from two prenatal clinics was recruited to take part in this study. Because of the organization of each clinic, it was decided that randomization within clinics to Control and Experimental Groups could not be done without contamination across Groups. Therefore, women recruited from Clinic A served in the Control Group, while women recruited from Clinic B served in the Experimental Group. Seventeen women attending Clinic A (Control Group) and 19 women attending Clinic B (Experimental Group) agreed to participate in this study. Informed Consent was obtained from all women by the principal investigator. Two women in the Experimental Group did not complete the postpartum data collection, two women in the Control Group did not complete any data collection postpartum. Therefore, complete data was obtained on 15 women in the Control Group and 17 women in the Experimental Group.
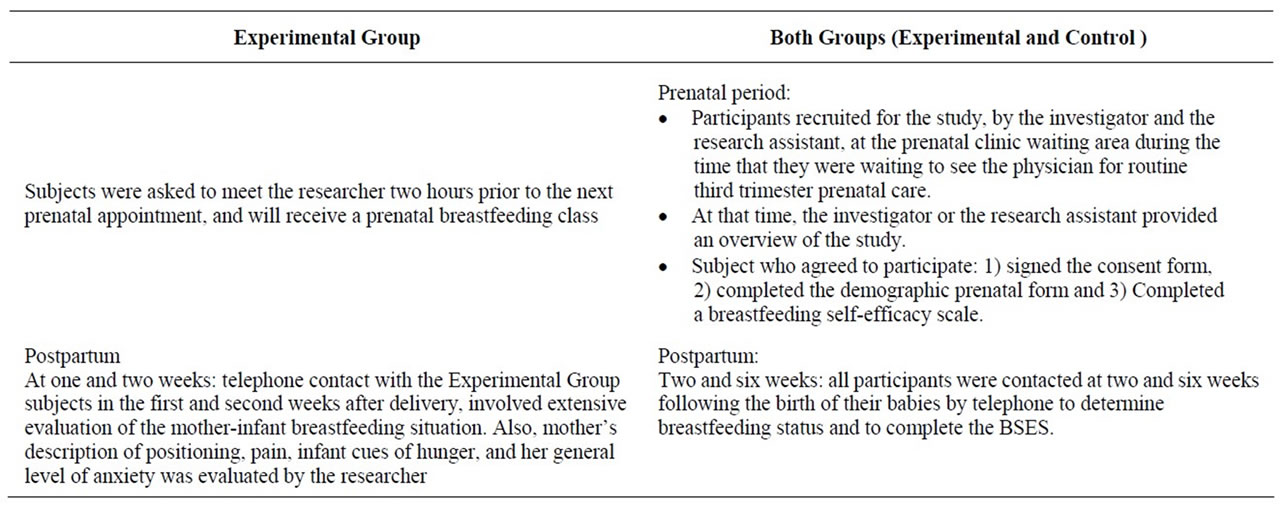
Table 1. Study procedure summary.
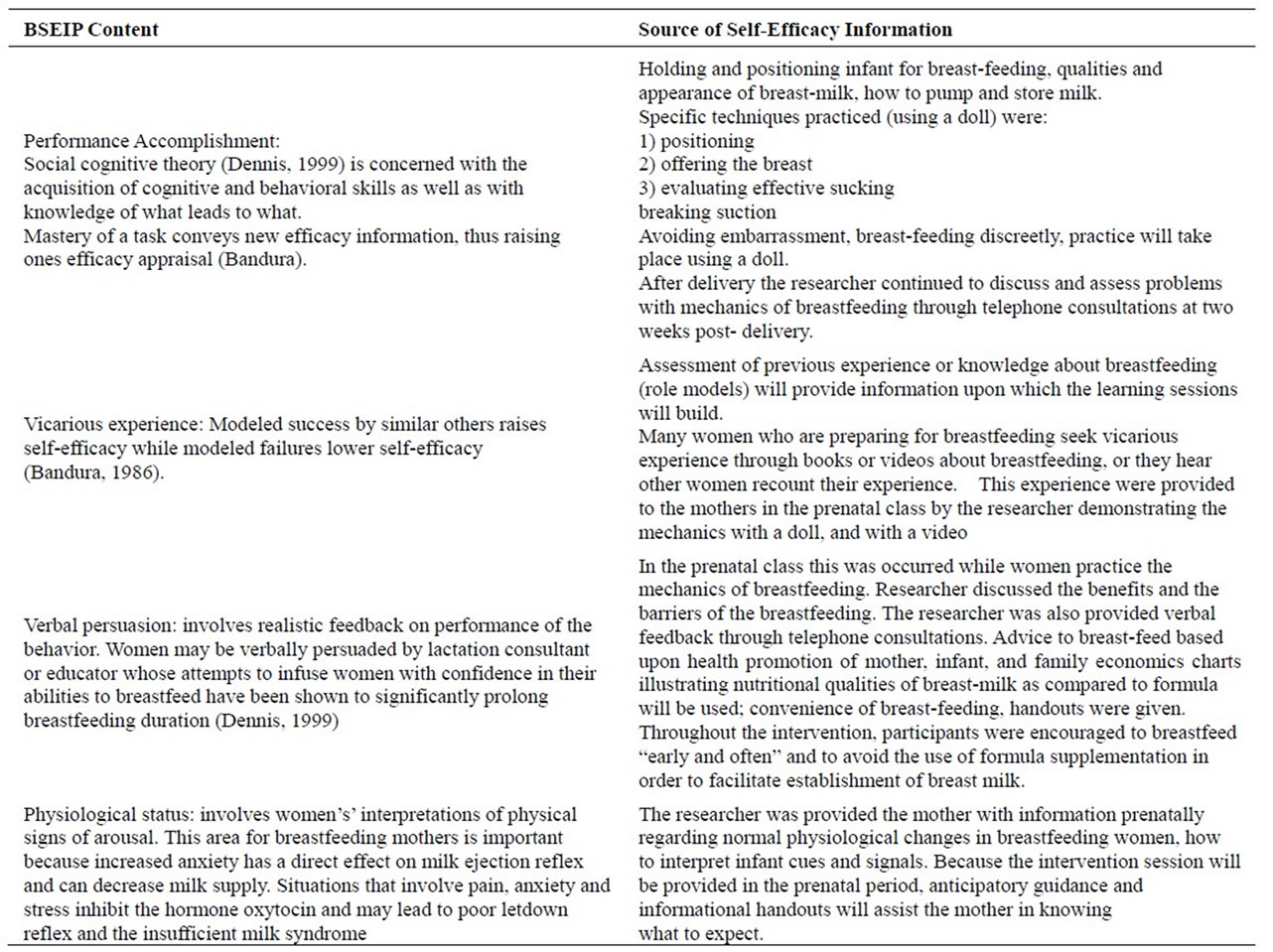
Table 2. BSEIP content, source of self-efficacy information.
3.2. Demographics Characteristics
The demographic characteristics of each Group are reported in Table 3. There were no statistically significant differences between the two groups. All of the women in the Control Group and 13 of the 18 (72%) women in the Experimental Group were non-Hispanic White. Although not statistically significant, more women in the Control Group than in the Experimental Group were primapara (80% versus 53.7%, respectively; t(30) = –2.345, p = 0.026); women in the Experimental Group tended to have higher incomes than women in the Control Group (see Table 4).
3.3. Hypotheses Testing
The mean BSES score was 108.33 (SD = 30.29) and 108.52 (SD = 28.27) for the Control and Experimental Group, respectively [t(30) = –1.09, p = 0.95].
Hypothesis 1: Independent t-tests revealed that women who received the intervention reported a significantly higher BSES score at Time 2 ( two weeks postpartum) and Time 3 ( 6 weeks postpartum) than women who did not receive the intervention; t(30) = –2.33 (p = 0.026) and t(30) = –3.97 (p = 0.00) at Time 2 and Time 3, respectively. Table 4 provides the means, ranges, and standard deviations for BSES scores at Time 1, Time 2, and Time 3. As noted in Table 4, there was also a positive significant improvement in the BSES score of the women in the Experimental Group from Time 1 (M = 108.3) to Time 2 (M = 135.9) and Time 3 (M = 143.7).
Hypothesis 2: Breastfeeding duration was determined by follow up telephone calls at six week postpartum. When asked at the prenatal visit, all mothers (in both experimental and control groups) intended to at least initiate breastfeeding in the postpartum period; 64% of the women in the Experimental Group and 53% of women in the Control Group intended to breastfeed more than six weeks.
The analysis revealed a statistically difference between the Control and Experimental Group (t(30) = –3.02, p = 0.003) on number of days the women breastfed. Women in the Experimental Group demonstrated a significant increase in the breastfeeding duration than did women in the Control Group.

Table 3. Sociodemographic characteristics of subjects by Group.
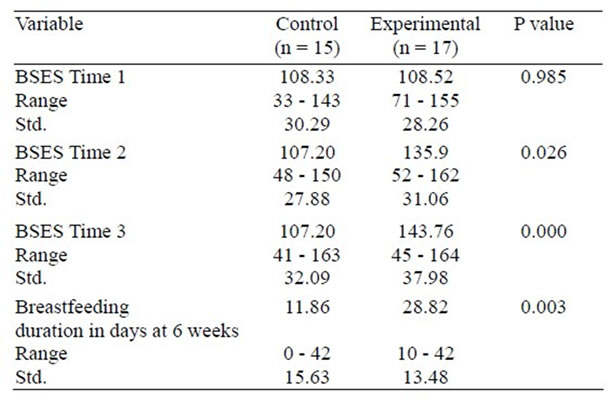
Table 4. Mean BSES score by Time and Group and mean breastfeeding duration by Group at Time 3.
4. RESULTS
The relationship between breastfeeding self-efficacy at Time 1 for the total sample was found to be positive and not significant (r = –0.054). There was, a significant relationship between breast-feeding self-efficacy and breastfeeding duration (r = 0.531, p = 0.01; and, r = 0.370, p = 0.05) at Time 2 and Time 3, respectively. Maternal breastfeeding self-efficacy during the prenatal period (BSES Time 1) was not related to breastfeeding duration in this study. In contrast, however, breastfeeding self-efficacy at 2- and 6-weeks postpartum was significantly related to breastfeeding duration.
The literature on breastfeeding provides strong support for the development of this intervention, and the results of this study were congruent with findings of earlier studies [13,15,17,22]. Encouraging early and frequent mother contact for breastfeeding [5], and support through telephone contact in the early postnatal period [15,18].
Both hypotheses in this study were supported. Mothers who received the intervention had higher BSES scores postpartum and breastfed for significantly longer than mothers who did not receive the intervention. These results support Dennis’ (1999) BFSE Theory and provide empirical support for the manipulation of self-efficacy to affect breastfeeding behavior. The results examined from the Experimental Group supported the BFSE Theory in a number of ways. First, high self-efficacy scores predicted the continuation and maintenance of breastfeeding behavior regardless of obstacles [17,18]; in this case the obstacle was defined by the fact that all women received formula samples in the hospital and no women in the Experimental Group received lactation consultation. Second, the high breastfeeding duration rate demonstrated by the Experimental Group, as compared to the Control Group, suggests that the intervention, including prenatal information and postpartum follow-up, enhanced breastfeeding self-efficacy and duration in a group of low-income women. Third, BFSE Theory states that the enactive attainment and verbal persuasion will enhance self-efficacy [18]. Verbal persuasion was evident in the actual practice of the breastfeeding and support from the researcher and research assistant. Results showed an increase of breastfeeding self-efficacy score from pre-test (before the treatment) to post-test (2 weeks postpartum).
The sample in this study was composed of mainly non-Hispanic White, low income women, a group that has a historically low rate of breastfeeding. The 6-week continuation rate was 43.81% for our sample, compared to the national 6-week continuation rate of 32.2 [2]. Of the 36 participants who enrolled in the study, one infant developed a medical condition and was unable to continue, three women were lost to follow-up at 2- or 6-weeks postpartum. The strong support provided to the women in both groups may have made them feel more committed to continuing participating in the study. Another factor that might have contributed to the continuation of breastfeeding in this sample was the women’s prenatal intention to breastfeed.
The results of this study are consistent with the research which has documented the effects of follow up and support on breastfeeding outcomes and has found that nursing support during the first two weeks postpartum period can have the greatest positive effect on the breastfeeding outcome [17,23]. Fewer women Experimental Group were primaparous (43.7%) as compared to women in the Control Group (80%). This may have contributed to the higher BSES scores reported by the Experimental Group at Time 2 and 3.
5. CONCLUSIONS
The results of this study suggest that the BSEIP, which incorporated the four principle sources of information from the Breastfeeding Self-Efficacy Theory, contributed to an increase in the mothers’ breastfeeding self-efficacy that was sustained over time, and increased breastfeeding duration. Breastfeeding mothers who received the intervention felt more confident in their ability to breastfeed than mothers who did not receive the intervention program. The intervention provided in this study was different from other interventions reported in the literature in that it used specific and consistent information on technique and physical practice of breastfeeding skills.
There was a positive relationship between self-efficacy and health behavior maintenance, as evidenced by high breastfeeding self-efficacy posttest scores and high breastfeeding continuation rate, which in turn supports the usefulness of breastfeeding self-efficacy as a manipulatable factor, which can be precisely measured in task and action.
Findings suggest that a one-hour intervention during the prenatal period, including all the components to enhance mother’s self-efficacy, and support from the researcher during the postpartum period, may make a difference in a sample of low income women who intend to breastfeed. This study supports literature findings that prenatal education and postpartum support are important to the outcome of breastfeeding.
6. LIMITATIONS
This study has a number of limitations. The use of a non-probability convenience sample did not reflect a diverse population, limiting the extent of generalizability of the findings to other breastfeeding mothers of different backgrounds. This study also used a small sample. It was difficult to recruit subjects to this study; most of the women in the two clinics did not intend to breastfeed and therefore, did not meet the inclusion criteria. The possibility of the response bias was considered as participants completed questionnaires related to their caregiving abilities in relation to infant breastfeeding. It was recognized that participants may tend to give favorable responses so that they will be perceived as competent mothers. The intervention in this study was done individually for each woman, a technique that is probably not feasible in a busy clinical setting for staff nurses.
![]()
![]()
REFERENCES
- American Academy of Pediatrics Work Group on Breastfeeding (2005) Breastfeeding and the use of human milk. Pediatrics, 115, 496-506. doi:10.1542/peds.2004-2491
- US Department of Health and Human Services (200) Healthy people 2010. US Department of Health and Human Services, Washington DC.
- Arlotti, J.P., Cottrell, B.H., Lee, S.L. and Curtin, J.J. (1998) Breastfeeding among low-income women with and without peer support. Journal of Community Health Nursing, 15, 163-178. doi:10.1207/s15327655jchn1503_4
- Donath, S.M., Amir, L.H. and the ALSPAC Study Team (2003) Relationship between prenatal infant feeding intention and initiation and duration of breast-feeding: A cohort study. Acta Paediatrica, 92, 352-356. doi:10.1111/j.1651-2227.2003.tb00558.x
- Vogel, A.M. (2003) Intended plans for breast-feeding duration: A simple tool to predict breast-feeding outcome. Acta Paediatrica, 92, 270-271. doi:10.1111/j.1651-2227.2003.tb00543.x
- Janke, J. (1994) Development of the breastfeeding attrition prediction tool. Nursing Research, 43, 100-104. doi:10.1097/00006199-199403000-00008
- O’Campo, P., Faden, R.R., Gielen, A.C. and Wang, M.C. (1992) Prenatal factors associated with breastfeeding duration: Recommendations for prenatal interventions. Birth, 19, 195-201. doi:10.1111/j.1523-536X.1992.tb00402.x
- Riordan, J. (2005) Breastfeeding and human lactation. Jones and Bartlett Publishers, Sudbury.
- Riordan, J., Gill-Hopple, K. and Angeron, J. (2005) Indicators of effective breastfeeding and estimates of breast milk intake. Journal of Human Lactation, 21, 406-412. doi:10.1177/0890334405281032
- Anderson, E. and Gaden, E. (1991) Nurses’ knowledge of breastfeeding. Journal of Obstetrical, Gynecological, and Neonatal Nursing, 20, 58-64. doi:10.1111/j.1552-6909.1991.tb01677.x
- Blyth, R., Creedy, D., Dennis, C., Moyle, W., Pratt, J. and De Vries, S. (2002) Effect of maternal confidence on breastfeeding duration: An application of breastfeeding self-efficacy theory. Birth: Issues in Perinatal Care, 29, 278-274. doi:10.1046/j.1523-536X.2002.00202.x
- Blyth, R., Creedy, D., Dennis, C., Moyle, W., Pratt, J. and De Vries, S. (2004) Breastfeeding duration in an Australian population: The influence of modifiable antenatal factors. Journal of Human Lactation, 20, 30-38. doi:10.1177/0890334403261109
- Pincombe, J., Baghurst, P., Antoniou, G., Peat, B., Henderson, A. and Reddin, E. (2008) Baby friendly hospital initiative practices and breast feeding duration in a cohort of first-time mothers in Adelaide, Australia. Midwifery, 24, 55-61.
- Dennis, C.L. (1999) Theoretical underpinnings of breastfeeding confidence: A self-efficacy framework. Journal of Human Lactation, 15, 195-201. doi:10.1177/089033449901500303
- Dennis, C. (2006) Identifying predictors of breastfeeding self-efficacy in the immediate postpartum period. Research in Nursing & Health, 29, 256-268. doi:10.1002/nur.20140
- Field, P.A. and Renfrew, M. (1991) Teaching and support nursing: In the postpartum period. International Journal of Nursing Studies, 28, 131-144. doi:10.1016/0020-7489(91)90003-L
- Dennis, C.L., Hodnett, E., Gallop, R. and Chalmers, B. (2002) A randomized controlled trial evaluation of the effect of peer support on breastfeeding on breastfeeding duration among primiparous women. Canadian Medical Association Journal, 166, 21-28.
- Dennis, C.-L. and Faux, S. (1999) Development and psychometric testing of the breastfeeding self-efficacy scale. Research in Nursing and Health, 22, 399-409. doi:10.1002/(SICI)1098-240X(199910)22:5<399::AID-NUR6>3.0.CO;2-4
- Creedy K., Dennis, C.-L., Blyth, R., Moyle, W., Pratt, J. and De Vries, S. (2003) Psychometric Characteristics of the breastfeeding self-efficacy scale: Data from an Australian sample. Research in Nursing and Health, 26, 143- 152. doi:10.1002/nur.10073
- Dai, X. and Dennis, C. (2003) Translation and validation of the breastfeeding self-efficacy scale into Chinese. Journal of Midwifery & Women’s Health, 48, 350-356. doi:10.1016/S1526-9523(03)00283-6
- Gulick, E.F. (1989) Informational correlates of successful breastfeeding. American Journal of Maternal Child Nursing, 7, 370-375.
- Houston, C.R. and Field, P.A. (1988) Practices and policies in the initiation of breastfeeding. Journal of Obstetrical, Gynecological, and Neonatal Nursing, 17, 418-425. doi:10.1111/j.1552-6909.1988.tb00468.x
- Hill, P., Wilhelm, P., Aldag, J. and Chatterton, R. Jr. (2004) Breast augmentation & lactation outcome: A case report. MCN: The American Journal of Maternal Child Nursing, 29, 238-242. doi:10.1097/00005721-200407000-00008

