 Open Journal of Stomatology, 2013, 3, 440-446 OJST http://dx.doi.org/10.4236/ojst.2013.38073 Published Online November 2013 (http://www.scirp.org/journal/ojst/) Evaluation of an oral moisture-checking device for screening dry mouth* Yosuke Fukushima1#, Tetsuya Yoda1, Shoichiro Kokabu1, Ryuichiro Araki2, Tsubasa Murata3, Yoshimasa Kitagawa3, Ken Omura4, Shuji Toya5, Kayoko Ito6, Saori Funayama6, Hiroshi Iwabuchi7, Kazuhiro Asano8, Yutaka Imai8, Akihide Negishi9, Satoshi Yokoo9, Goichi Matsumoto10, Eiro Kubota10, Hideki Watanabe11, Mikio Kusama11, Kojiro Onizawa12, Takuya Goto12, Seiji Nakamura13, Ryuichi Nakazawa14, Kiyoshi Harada14, Takashi Fujibayashi10 1Department of Oral and Maxillofacial Surgery, Faculty of Medicine, Saitama Medical University, Saitama, Japan 2Community Health Science Center, Saitama Medical University, Saitama, Japan 3Oral Diagnosis and Medicine, Department of Oral Pathobiological Science, Graduate School of Dental Medicine, Hokkaido Univer- sity, Sapporo, Japan 4Oral Surgery, Department of Oral Restitution, Division of Oral Health Sciences, Graduate School, Tokyo Medical and Dental Uni- versity, Tokyo, Japan 5Oral and Maxillofacial Surgery, Dry Mouth Clinic, The Nippon Dental University Niigata Hospital, Niigata, Japan 6Division of Gereatric Dentistry, Niigata University Medical & Dental Hospital, Niigata, Japan 7Department of Dentistry and Oral Surgery, Tochigi National Hospital, Tochigi, Japan 8Department of Oral and Maxillofacial Surgery, Dokkyo Medical University School of Medicine, Tochigi, Japan 9Department of Stomatology and Oral Surgery, Gunma University Graduate School of Medicine, Maebashi, Japan 10Department of Oral and Maxillofacial Surgery, Kanagawa Dental College, Yokosuka, Japan 11Department of Oral and Maxillofacial Surgery, Jichi Medical University, Tochigi, Japan 12Department of Oral and Maxillofacial Surgery, Institute of Clinical Medicine, University of Tsukuba, Tsukuba, Japan 13Section of Oral and Maxillofacial Oncology, Division of Maxillofacial Diagnostic and Surgical Sciences, Faculty of Dental Science, Kyushu University, Fukuoka, Japan 14Department of Oral and Maxillofacial Surgery, Division of Medicine, Interdisciplinary Graduate School of Medicine and Engi- neering, University of Yamanashi, Kofu and Tamaho, Japan Email: #yf37@saitama-med.ac.jp Received 18 August 2013; revised 20 September 2013; accepted 2 October 2013 Copyright © 2013 Yosuke Fukushima et al. This is an open access article distributed under the Creative Commons Attribution Li- cense, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Objective: This multicenter clinical study was to assess the clinical usability of an oral moisture- checking device in detecting the dry mouth patients and evaluating the optimal measurement site. Materials and Methods: The study group comprised 250 patients with dry mouth and 241 healthy volunteer subjects at 13 medical centers. This device was used to measure the moisture degrees of the lingual mucosa and the buccal mucosa. Subjective oral dryness, objective oral dryness, and saliva flow rates were also compared between the two groups. For statistical analysis, receiver-operating chara- cteristic analysis was performed to calculate the area under the curve (AUC). Results: The moisture degree of the lingual mucosa was significantly lower in the dry mouth group (27.2 ± 4.9) than that in the healthy group (29.5 ± 3.1, AUC = 0.653). When a lingual mucosa moisture degree of 31.0 or higher was defined as normal, less than 27.0 as dry mouth, and 27.0 to less than 31.0 as borderline zone of dry mouth, both the sensitivity and the specificity for the diagnosis of dry mouth were close to 80%. Conclusion: These results suggest that the oral moisture-checking device is a usable screening device for dry mouth. Keywords: Dry Mouth; Oral Moisture-Checking Device; ROC Analysis 1. INTRODUCTION *On June 2, 2010, Mucus® received manufacturing and marketing ap- roval as a body composition analyzer, a class II controlled medical device (medical device approval number: 22200BZX00640000) by Ministry of Health, Labour and Welfare, Japan. We have no financial conflict of interest. #Corresponding author. In general, oral dryness is objectively evaluated by ex- aminations of salivary flow rates by techniques of stimu- lated whole salivary collection (SWSC) such as the OPEN ACCESS  Y. Fukushima et al. / Open Journal of Stomatology 3 (2013) 440-446 441 chewing gum test and the Saxon test or unstimulated whole salivary collection (UWSC) such as spitting me- thod, or by assessing salivary gland secretory function by salivary gland scintigraphy. These methods indirectly estimate oral dryness on the basis of the salivary flow rate and salivary gland function, but do not evaluate oral mucosal dryness (moisture degree) directly. An oral moisture-checking device has been developed recently by adapting a skin moisture sensor suitable for oral mucosa. This device measures the moisture content of the surface of oral mucosa on the basis of electrostatic capacity. In 2002, a prototype model was developed, and possibilities for clinical use have been reported [1-3]. Subsequently, several improvements were made, in- cluding the use of smaller device sensors, the introduc- tion of a spring to ensure that pressure is uniformly ap- plied, and changing the shape of the handle and labeling. The improved oral moisture-checking devices in third- generation are now available. Measurements can now be obtained in about 2 seconds, causing minimal stress and discomfort to subjects in examinee [4,5]. However, the physiological borderline value classifying patients with dry mouth from normal subjects has not been established yet. In addition, although the moisture contents of the tongue and buccal mucosa are usually measured, the op- timal site for measurement remains unclear. The purpose of this multicenter clinical study is to assess the clinical usability of an oral moisture-checking device in detecting the dry mouth patients and evaluating the optimal meas- urement site. 2. SUBJECTS AND METHODS The study group comprised subjects with dry mouth (dry mouth group) and those without dry mouth (healthy group) who were enrolled at the following 13 participat- ing medical centers: Hokkaido University Hospital, Jichi Medical University Hospital, Dokkyo Medical Univer- sity Hospital, Tochigi National Hospital, Gunma Univer- sity Hospital, Tsukuba University Hospital, Saitama Medical University Hospital, Tokyo Medical and Dental University Hospital, Kanagawa Dental College Hospital, Niigata University Medical and Dental Hospital, Nippon Dental University Niigata Hospital, Yamanashi Univer- sity Hospital, and Kyushu University Hospital. 2.1. Inclusion Criteria for Dry Mouth Group Subjects in the dry mouth group were adults who were subjectively aware of mouth dryness and had a diagnosis of dry mouth according to the criteria proposed by the Japanese Society for Oral Mucous Membrane [6] (i.e., subjects who have objective symptom of dry mouth with decreased salivary flow rates in SWSC ≤10 mL/10 min- utes on the chewing gum test or ≤2 g/2 minutes on the Saxon test, or UWSC ≤1.5 mL/15 minutes, or subjects with decreased salivary gland function on salivary gland scintigraphy). These examinations were performed at the day or within 1 week before or after the measurement of oral moisture degree with an oral moisture-checking de- vice. During this period, no changes were allowed in factors with potential effects on mouth dryness, such as modifications of treatments, drugs, or environmental factors. However, if patients were receiving saliva-sti- mulating agents such as cevimeline hydrochloride hy- drate, pilocarpine hydrochloride or some other treatments such as salivary gland massage, the aforementioned ex- aminations were obtained on the same day as measure- ment with an oral moisture-checking device. Persons who routinely used oral moisturizers and those who were considered unsuitable for the study by the investigator were excluded. 2.2. Inclusion Criteria for Healthy Group Subjects in the healthy group were adult volunteers with no subjective awareness of mouth dryness who had SWSC rate of >10 mL/10 minutes on the chewing gum test. Persons who had a diagnosis of dry mouth or Sjögren’s syndrome, abnormalities of the oral mucosa, or burning mouth syndrome, and those who were considered un- suitable for the study by the investigator were excluded. The enrollment period was from October 2009 through May 2010. The target sample size determined with pre- liminary power analysis was 250 for both dry-mouth and healthy groups. Subjects were consecutively assigned to two groups according to the above mentioned criteria. The following variables were evaluated: subjective oral dryness, objective oral dryness, SWSC rates on the chewing gum test, UWSC rates on the spitting method, and oral moisture degree as measured with the testing oral moisture-checking device. A self-administered ques- tionnaire was used to assess subjective oral dryness. Each patient was requested to grade oral dryness at the time of measuring oral moisture degree as follows: no sensation of mouth dryness (0 points), mild mouth dry- ness (1 point), moderate mouth dryness (2 points), and severe mouth dryness (3 points). Objective oral dryness was evaluated by the examiner who measured mois- ture-checking device as follows: none (0 points), mild (1 point), moderate (2 points), and severe (3 points). Mu- cus®, oral moisture-checking devices* (serial numbers, 301722 to 301726, 301731, 301733 to 301736, 301741, 301744 to 301754, 301756 to 301758, and 301760; Life Co., Ltd., Saitama, Japan) were used to measure oral moisture degree (Figure 1). To eliminate the effects of stimulants such as food, water, speech, and stress on the measurements, the subjects in examinee were requested to physically rest and mentally relax for about 5 minutes Copyright © 2013 SciRes. OPEN ACCESS  Y. Fukushima et al. / Open Journal of Stomatology 3 (2013) 440-446 442 Figure 1. Oral moisture-checjing device. before measurement [5]. A disposable cover which was made by polyethylene was applied to the sensor for each subject. This coverage of the sensor has been proven not to disturb the calibration of the device. The measurement sites were the center of the lingual mucosa about 10 mm from the tip of the tongue and the right buccal mucosa about 10 mm from the corner of the mouth (Figures 2(a) and 2(b)). The sensor was manually applied to the meas- urement sites at a pressure of about 200 g, as practiced beforehand with a manometer. To eliminate outliers, oral mucosal wetness was measured continuously 3 consecu- tive times. The median was used as a representative value [4]. We examined the following variables: oral moisture degree according to measurement site, partici- pating medical centers, cut-off values according to measurement sites, correlations of oral mucosal dryness with other measured variables, and the presence or ab- sence of adverse events at the time of measurement of oral moisture degree. Receiver-operating characteristic (ROC) analysis, un- paired t-tests, Pearson correlation coefficients, and Spearman correlation coefficients (Medcalc version 11.3 for Windows) were used for statistical analysis. As for ROC analysis, the area under the ROC curve (AUC) was calculated, and the value providing the best balance be- tween sensitivity and specificity was used as a cut-off point. P values of less than 5% were considered to indi- cate significant differences. In this study, all subjects received thorough explana- tions about the contents of examinations, methods in- cluding the measurement, the need for examinations and the measurement, associated risks, freedom to give or withdraw consent, protection of privacy and personal information, anticipated benefits, and alternative exami- nations that were available. All subjects signed informed consent forms. The ethical approval of this study was obtained by the Institutional Review Board of Saitama Medical University (approval number: 09-015-1), as well as by the institutional review boards of each participating medical center. 3. RESULTS 1) Demographic characteristics of subjects The study group comprised 250 subjects with dry mouth (35 men and 215 women) and 241 healthy sub- jects with no evidence of dry mouth (117 men and 124 (a) (b) Figure 2. Measurement of oral moisture degree of the lingual mucosa and buccal mucosa; (a) Lingual mucosa; (b) Buccal mucosa. women) who were enrolled at 13 medical centers (A to M) (Table 1). Mean age was 65.0 years in the dry mouth group and 50.5 years in the healthy group. 2) Oral moisture degree according to the measurement site and medical center Oral moisture degree of the lingual mucosa was sig- nificantly lower in the dry mouth group (27.2 ± 4.9 [mean ± standard deviation]) than in the healthy group (29.5 ± 3.1, p < 0.001). Oral moisture degree of the buc- cal mucosa did not differ significantly between the dry mouth group (31.2 ± 3.7) and the healthy group (31.3 ± 2.6). In both groups, oral moisture degree of the buccal mucosa was significantly higher than that of the lingual mucosa (p < 0.001 in the both groups) (Table 2). The data from 9 centers (A to I) had enough sample sizes needed for statistical comparison between the 2 Copyright © 2013 SciRes. OPEN ACCESS 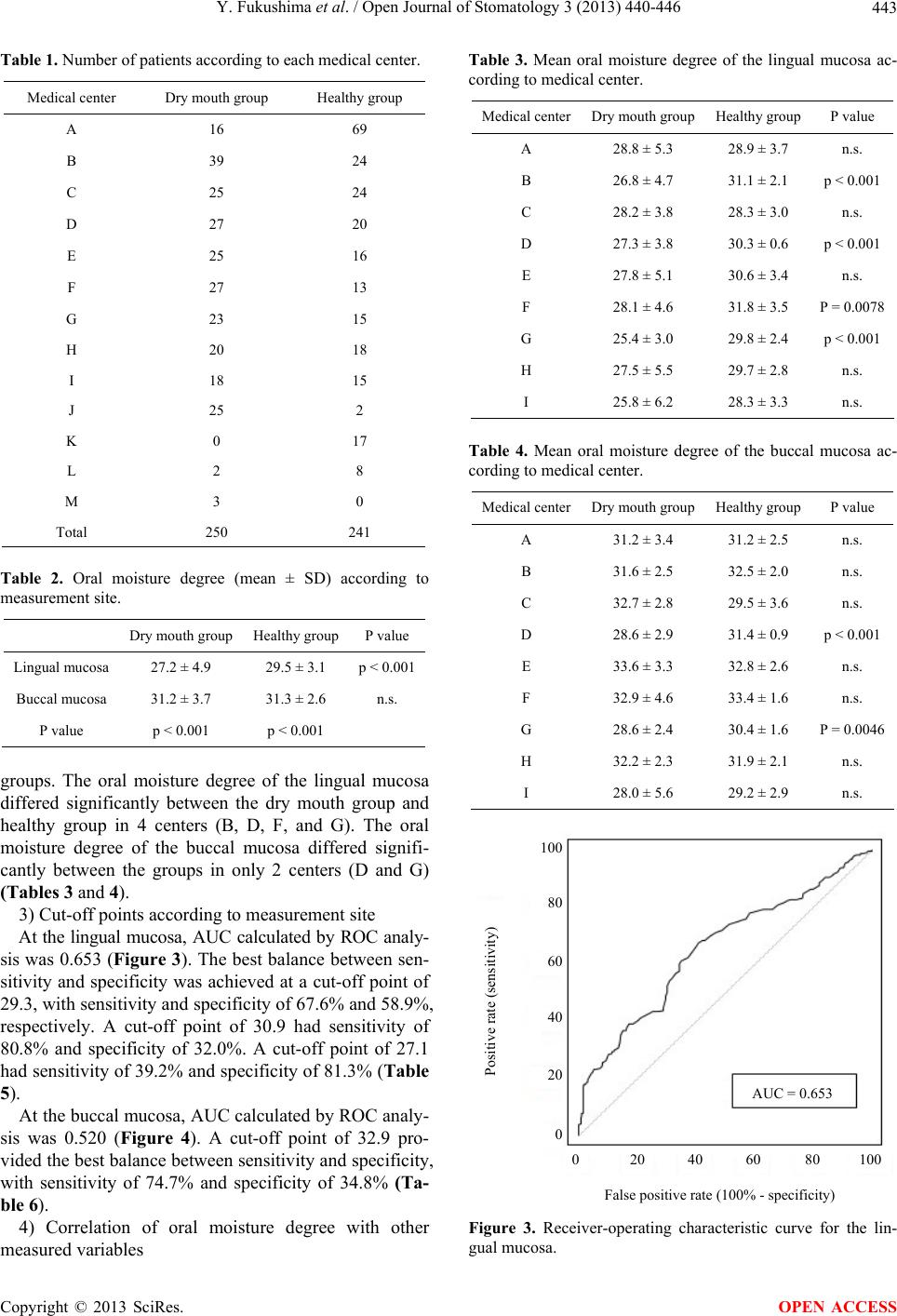 Y. Fukushima et al. / Open Journal of Stomatology 3 (2013) 440-446 443 Table 1. Number of patients according to each medical center. Medical center Dry mouth group Healthy group A 16 69 B 39 24 C 25 24 D 27 20 E 25 16 F 27 13 G 23 15 H 20 18 I 18 15 J 25 2 K 0 17 L 2 8 M 3 0 Total 250 241 Table 2. Oral moisture degree (mean ± SD) according to measurement site. Dry mouth groupHealthy group P value Lingual mucosa 27.2 ± 4.9 29.5 ± 3.1 p < 0.001 Buccal mucosa 31.2 ± 3.7 31.3 ± 2.6 n.s. P value p < 0.001 p < 0.001 groups. The oral moisture degree of the lingual mucosa differed significantly between the dry mouth group and healthy group in 4 centers (B, D, F, and G). The oral moisture degree of the buccal mucosa differed signifi- cantly between the groups in only 2 centers (D and G) (Tables 3 and 4). 3) Cut-off points according to measurement site At the lingual mucosa, AUC calculated by ROC analy- sis was 0.653 (Figure 3). The best balance between sen- sitivity and specificity was achieved at a cut-off point of 29.3, with sensitivity and specificity of 67.6% and 58.9%, respectively. A cut-off point of 30.9 had sensitivity of 80.8% and specificity of 32.0%. A cut-off point of 27.1 had sensitivity of 39.2% and specificity of 81.3% (Table 5). At the buccal mucosa, AUC calculated by ROC analy- sis was 0.520 (Figure 4). A cut-off point of 32.9 pro- vided the best balance between sensitivity and specificity, with sensitivity of 74.7% and specificity of 34.8% (Ta- ble 6). 4) Correlation of oral moisture degree with other measured variables Table 3. Mean oral moisture degree of the lingual mucosa ac- cording to medical center. Medical centerDry mouth group Healthy group P value A 28.8 ± 5.3 28.9 ± 3.7 n.s. B 26.8 ± 4.7 31.1 ± 2.1 p < 0.001 C 28.2 ± 3.8 28.3 ± 3.0 n.s. D 27.3 ± 3.8 30.3 ± 0.6 p < 0.001 E 27.8 ± 5.1 30.6 ± 3.4 n.s. F 28.1 ± 4.6 31.8 ± 3.5 P = 0.0078 G 25.4 ± 3.0 29.8 ± 2.4 p < 0.001 H 27.5 ± 5.5 29.7 ± 2.8 n.s. I 25.8 ± 6.2 28.3 ± 3.3 n.s. Table 4. Mean oral moisture degree of the buccal mucosa ac- cording to medical center. Medical centerDry mouth group Healthy group P value A 31.2 ± 3.4 31.2 ± 2.5 n.s. B 31.6 ± 2.5 32.5 ± 2.0 n.s. C 32.7 ± 2.8 29.5 ± 3.6 n.s. D 28.6 ± 2.9 31.4 ± 0.9 p < 0.001 E 33.6 ± 3.3 32.8 ± 2.6 n.s. F 32.9 ± 4.6 33.4 ± 1.6 n.s. G 28.6 ± 2.4 30.4 ± 1.6 P = 0.0046 H 32.2 ± 2.3 31.9 ± 2.1 n.s. I 28.0 ± 5.6 29.2 ± 2.9 n.s. 02040 60 80100 False positive rate (100% - specificity) AUC = 0.653 0 20 40 60 80 100 Positive rate (sensitivity) Figure 3. Receiver-operating characteristic curve for the lin- ual mucosa. g Copyright © 2013 SciRes. OPEN ACCESS  Y. Fukushima et al. / Open Journal of Stomatology 3 (2013) 440-446 Copyright © 2013 SciRes. 444 Table 5. Cut-off values for the lingual mucosa. Cut-off value Sensitivity 95%CI Specificity 95%CI Positive likelihood ratio Negative likelihood ratio 30.9 80.8 75.4 - 85.5 32 26.1 - 38.2 1.19 0.6 29.3 67.6 61.4 - 73.4 58.9 52.4 - 65.2 1.65 0.55 27.1 39.2 33.1 - 45.6 81.3 75.8 - 86.0 2.1 0.75 0 20 4060 80 100 False positive rate (100% - specificity) AUC = 0.520 0 20 40 60 80 100 Positive rate (sensitibity) OPEN ACCESS Figure 4. Receiver-operating characteristic curve for the lbuc- cal mucosa. Subjective oral dryness and objective oral dryness were measured in all 491 participating subjects. At the lingual mucosa, the correlation coefficients of oral mois- ture degree with subjective oral dryness and objective oral dryness were −0.320 and −0.350, respectively, indi- cating weak negative correlations (p < 0.05). At the buc- cal mucosa, oral moisture degree did not correlate with either subjective oral dryness or objective oral dryness. Among the 491 subjects, salivary flow rates were measured by SWSC of the chewing gum test in 472 sub- jects, and UWSC in 211. At the lingual mucosa, the cor- relation coefficients of the oral moisture degree with SWSC and UWSC were 0.25 and 0.34, respectively, indicating weak positive correlations (p < 0.05). At the buccal mucosa, however, oral moisture degree did not correlate with saliva flow rates (Table 7). 5. Presence or absence of adverse events at the time of measuring oral moisture degree During the study period, there were no adverse events caused by the use of the oral moisture-checking device. 4. DISCUSSION This oral moisture-checking device measures electro- static capacity on the basis of impedance generated by connecting high-frequency waves supplied by a 5-volt battery to plus and minus comb-shaped electrodes de- picted on the surface of a 7.2 mm2 sensor. The electro- static capacity reflects not only the water content of the oral mucosal surface, but also the intramucosal water content to a depth of about 50 µm. The numerical data are expressed as 3-digit numbers, ranging from 0.00 to 99.8. The value strongly correlates positively with the actual gravimetric moisture percentage, with a correla- tion coefficient of 0.99, and is a relative measure of wa- ter content, rather than the actual moisture percentage. Even if technical difficulties occur, such as damage to an insulator, only a limited site is exposed to a maximum electric current of 8.9 µA and the effect on the human body is nearly negligible. The sensor has a square surface. Accurate measure- ments cannot be obtained unless the surface of this sen- sor comes in close contact with the mucosal surface. Therefore, a flat surface of an adequate size is needed at the measurement site of the oral mucosa. The lingual mucosa and the buccal mucosa have been used as meas- urement sites [1-4]. These sites were also used for meas- urement in the present study. The moisture degree of the buccal mucosa was significantly higher than that of the lingual mucosa in both the dry mouth group and healthy group. Disabato-Mordarski et al. reported that the thick- ness of the moisture coating of the oral mucosa is site- specific, strongly suggesting that the moisture degree differs depending on the site of measurement [7]. Taka- hashi et al. similarly reported that the moisture degree of the buccal mucosa tended to be higher than that of the lingual mucosa in patients with subjective oral dryness [2]. One of the reasons for this difference is that the measurement site of the buccal mucosa is near the pa- rotid papilla. Secreted saliva may thus be directly meas- ured. Takahashi et al. found that the moisture degrees differed significantly between patients with dry mouth and healthy subjects in both the lingual mucosa and the buccal mucosa [2]. In our study, however, the moisture degree of the buccal mucosa did not differ between the groups. Moreover, the moisture degrees of the buccal mucosa were nearly the same in the dry mouth group (31.2 ± 3.7) and the healthy group (31.3 ± 2.6). When the results were analyzed according to medical centers, the moisture degree of the tongue was lower in the dry mouth group at all centers, whereas the moisture degree of the buccal mucosa was higher in the dry mouth group than in the healthy group at 3 centers. In addition, the moisture degree of the buccal mucosa did not signifi- cantly correlate with subjectve oral dryness, objective i  Y. Fukushima et al. / Open Journal of Stomatology 3 (2013) 440-446 445 Table 6. Cut-off values for the buccal mucosa. Cut-off value Sensitivity 95%CI Specificity 95%CI Positive likelihood ratio Negative likelihood ratio 33.7 81.7 76.3 - 86.4 26.4 21.0 - 32.3 1.11 0.69 32.9 74.7 68.7 - 80.1 34.8 28.9 - 41.1 1.15 0.73 28.3 12.5 8.6 - 17.3 80.4 74.9 - 85.1 0.64 1.09 Table 7. Relation between oral moisture degree and measured variables. Subjective oral dryness (N = 491) Objective oral dryness (N = 491) SWSC (N = 472) UWSC (N = 211) Correlation coefficient −0.32* −0.35* 0.25* 0.34* Lingual mucosa 95%CI −0.38 to 0.22 −0.43 to -0.27 0.16 to 0.33 0.21 to 0.45 Correlation coefficient 0.01 −0.02 −0.03 0.11 Buccal mucosa 95%CI −0.08 to 0.10 −0.10 to 0.07 −0.12 to 0.06 −0.03 to 0.24 oral dryness, the results of SWSC and UWSC. These findings suggest that the lingual mucosa is better suited than the buccal mucosa for the measurement of moisture degree by the oral moisture-checking device. Overall, the mean moisture degree of the lingual mu- cosa differed significantly between the dry mouth group and healthy group, but when the results were analyzed according to centers, significant differences were found at only 4 of the 9 centers. These results may have been caused by problems such as measurement bias of the device itself, technical bias of using the device and selec- tion bias in subject enrollment among the centers. As for measurement conditions, oral moisture degree (dryness) might be influenced by factors immediately before measurement, such as drinking water, prolonged conver- sation during interviews, and extreme tension. To elimi- nate these factors, subjects should physically rest and mentally relax for about 5 minutes before measurement [5]. Our study was conducted in accordance with this recommendation. However, some bias may have still existed. The optimal measurement pressure of the sensor of an oral moisture-checking device is 200 g. If the sen- sor is applied to the lingual mucosa at a pressure of 300 g, the value measured by the moisture-checking device would increase by 1.1 times on average [4]. In our study, we measured the moisture degree after practicing appli- cation of the sensor at a pressure of 200 g. However, we do not have exact evidence whether oral moisture degree was actually measured at a uniform pressure in all sub- jects. Outliers might occur if the contact angle of the sensor is not vertical to the mucosal surface. To avoid the occurrence of outliers, the median value of 3 or 5 meas- urements should be used [4]. In our study, we used the median of 3 measurements, but all outlying values may not have been eliminated. Oral moisture degree thus may not have been meas- ured appropriately in some subjects. However, the AUC of the ROC curve for the lingual mucosa was 0.653 in- cluding these values. This value is comparable to that of the diagnostic accuracy of creatine kinase for myocardial infarction [8]. These results indicate that the oral mois- ture-checking device may be a usable tool for the ex- amination of dry mouth. However, when a cut-off point of 29.3, providing the best balance between sensitivity and specificity, was used for diagnosis, the sensitivity and specificity were only 67.6% and 58.9%, respectively. Therefore, a differential diagnosis between dry mouth and non-dry mouth might be difficult by using cut-off point of 29.3. Taken together, the present oral mois- ture-checking devices should be considered as a screen- ing device, and a borderline range between dry mouth and non-dry mouth should be established. In our study, the cut-off value providing a sensitivity of at least 80% was 30.9 (sensitivity, 80.8%), indicating that dry mouth will not be diagnosed in about 2 of 10 patients with this condition. The cut-off value with a specificity value of at least 80% was 27.1 (specificity, 81.3%), indicating that dry mouth is misdiagnosed in less than 2 of 10 healthy subjects. If a moisture degree of 27.0 to 31.0 is defined as borderline zone for diagnosing dry mouth, a value of more than 31.0 as normal, and a value of less than 27.0 as dry mouth, the sensitivity and specificity are close to 80%, making the oral moisture-checking device to be a usable screening tool for dry mouth. Conventionally, dry mouth was diagnosed mainly on the basis of symptoms and salivary flow rates on the chewing gum test and other examinations. Osailan et al. showed that mucosal wetness of the anterior tongue cor- relate with UWSC in dry mouth patients [9]. Won et al. reported that moisture of the oral cavity depends on the USWC, is not always decreased at least in some patients [10]. Copyright © 2013 SciRes. OPEN ACCESS  Y. Fukushima et al. / Open Journal of Stomatology 3 (2013) 440-446 446 In our study, only a weak correlation was obtained at the lingual mucosa. However, saliva flow rates are merely an index of salivary gland function. Needless to say, decreased secretion of saliva may lead to dry mouth. If oral mucosal wetness is preserved, mouth dryness may not necessarily develop. On the other hand, even if saliva flow is enough, xerostomia induced by excessive oral vaporization can occur. Because the oral moisture- checking device measures the amount of moisture not only on the oral mucosal surface, but also in the epithet- lium of the oral mucosa, it provides a more accurate measure of the moisture status (dryness) of the oral mu- cosa than dose saliva flow rate. Therefore, the oral moisture-checking device may be usable as a screening device of the moisture status (dryness) of the oral mu- cosa. The oral moisture-checking device can be used to provide one of standard measures of the moisture status (dryness) of the oral mucosa. With further improvements, such devices are expected to be widely used for the ob- jective assessment of dry mouth. 5. CONCLUSION The oral moisture degree in patients with dry mouth group and normal subjects group was measured and sta- tistically analyzed. The moisture degree of the lingual mucosa showed significant differences between the groups, whereas that of the buccal mucosa did not. On ROC analysis, the AUC is 0.653 for the lingual mucosa and 0.520 for the buccal mucosa. For the lingual mucosa, when a moisture degree of more than 31.0 is defined as normal, less than 27.0 as dry mouth and 27.0 to 31.0 as borderline zone of dry mouth, both the sensitivity and the specificity are close to 80%. These results suggest that this moisture-checking device is usable as a screening device for dry mouth. 6. ACKNOWLEDGEMENTS We are grateful to Life Co., Ltd. for kindly providing us with the oral moisture-cheking devices. REFERENCES [1] Yamada, H., Nakagawa, Y., Nomura, Y., Yamamoto, K., Suzuki, M., Watanabe, N.Y., Saito, I. and Seto, K. (2005) Preliminary results of moisture checker for mucus in di- agnosing dry mouth. Oral Diseases, 11, 405-407. http://dx.doi.org/10.1111/j.1601-0825.2005.01136.x [2] Takahashi, F., Koji, T. and Morita, O. (2006) Oral dry- ness examination: Use of an oral moisture checking de- vice and modified cotton method. Prosthodontic Reserch and Practice, 5, 26-30. http://dx.doi.org/10.2186/prp.5.26 [3] Murakami, M., Nishi, Y., Kamashita, Y. and Nagaoka, E. (2009) Relationship between medical treatment and oral dryness diagnosed by oral moisture-checking device in patients with maxillofacial prostheses. Journal of Prost- hodontic Research, 53, 67-71. http://dx.doi.org/10.1016/j.jpor.2008.08.010 [4] Fukushima, Y., Kokabu, S., Kanaya, A., Hori, N., Tateyama, T., Sato, T., Sakata, Y., Kobayashi, A., Araki, R., Yanagisawa, H. and Yoda, T. (2007) Experimental examination of appropriate measurement method of oral moisture checking device. Japanese Society for Oral Mucous Membrane, 13, 16-25. [5] Fukushima, Y., Yoda, T., Araki, R., Hori, N., Kokabu, S., Yakata, Y. and Kobayashi, A. (2009) Experimental ex- amination of temporal variations of the moisture degree of the oral mucosa in ordinary persons. Japanese Society for Oral Mucous Membrane, 15, 15-21. http://dx.doi.org/10.6014/jjomm.15.15 [6] Committee for the Classification on Terminology of Japa- nese Society for Oral Mucous Membrane (2008) Classi- fication of xerostomia (dry mouth). Japanese Society for Oral Mucous Membrane, 14, 86-88. [7] Disabato-Mordarski, T. and Kleinberg, I. (1996) Meas- urement and comparison of the residual saliva on various oral mucosal and dentition surfaces in humans. Archives of Oral Biology, 41, 655-665. http://dx.doi.org/10.1016/S0003-9969(96)00055-6 [8] Peirce, J.C. and Cornell, R.G. (1993) Integrating stratum- specific likelihood ratios with the analysis of ROC curves. Medical Decision Making, 13, 141-151. http://dx.doi.org/10.1177/0272989X9301300208 [9] Osailan, S., Pramanik, R., Shirodaria, S., Challacombe, S.J. andProctor, G.B. (2011) Investigating the relation- ship between hyposalivation and mucosal wetness. Oral Diseases, 17, 109-114. http://dx.doi.org/10.1111/j.1601-0825.2010.01715.x [10] Won, S., Kho, H., Kim, Y., Chung, S. and Lee, S. (2001) Analysis of residual saliva and minor salivary gland se- cretions. Archives of Oral Biology, 46, 619-624. http://dx.doi.org/10.1016/S0003-9969(01)00018-8 Copyright © 2013 SciRes. OPEN ACCESS
|