Paper Menu >>
Journal Menu >>
 Open Journal of Ophthalmology, 2013, 3, 13-15 http://dx.doi.org/10.4236/ojoph.2013.31004 Published Online February 2013 (http://www.scirp.org/journal/ojoph) 13 A Case of Secondary Iris Cyst AfterPupilloplasty* Ja Young Lee1, Sun Woong Kim2, Eun Suk Koh3, Jee Ho Chang1# 1Department of Ophthalmology, College of Medicine, Soonchunhyang University, Bucheon, Korea; 2Department of Ophthalmology, Hando Hospital, Ansan, Korea; 3Department of Pathology, College of Medicine, Soonchunhyang University, Bucheon, Korea. Email: #jhchang@schbc.ac.kr Received November 23rd, 2012; revised December 24th, 2012; accepted January 3rd, 2012 ABSTRACT Purpose: To investigate the pathogenesis of a secondary iris cyst with an immunohistochemical method. Methods: Single observational case report. A pathologic specimen was obtained from a 5-year-old girl who was found to have a secondary iris cyst. She had a history of previous penetrating ocular trauma and subsequent cataract surgery and pupil- loplasty. Immunohistochemical staining with cytokeratin (CK) 19 and CK3 was used. Results: After immunohisto- chemical staining, the inner wall showed positiv e staining for CK19, which is sp ecific for limbal, peripheral cornea and conjunctival epithelium, and negative staining for CK3, which is specific for corneal epithelium. Conclusions: With the aid of immunohistochemical analysis, a conjunctival epithelial origin was indicated, and pupilloplasty was identified as the causal event of the iris cyst while the possibility of primary iris cyst was ruled out. Keywords: Immunohistochemistry; Pupilloplasty; Secondary Iris Cyst 1. Introduction Iris cysts can be classified as primary or secondary. Pri- mary cysts are thought to be of neuroepithelial origin, whereas secondary cysts may result from implantation, metastasis, par asites, or miotic therapy. Secondary iris cy- sts are usually associated with surgery or penetrating ocu- lar injuries [1]. Although secondary cysts are generally considered to be dr iv en b y ep ith elial do wngro w th [2 ], the specific origin of the cyst in our case was difficult to dif- ferentiate on the basis of light and electron microscopic characteristics. Here, we present a secondary iris cyst whose origin was presumed to be associated with pupilloplasty by pa- thologic examination and an immunohistochemical stu- dy. 2. Case Report A 5-year-old girl was scheduled for detailed examination under general anesthesia for a suspected solid iris mass in her right eye. She had a corneoscleral laceration with a prolapsed iris from the 8- to 10-o’clock positions 3 years ago. Two years after the primary repair, extracapsular cataract extraction with intraocular lens implantation an d pupilloplasty was performed with 10 - 0 polypropylene sutures. After 8 months, her corrected visual acuity drop- ped from 20/32 to 20/63, her intraocular pressure was 20 mmHg, and she had severe photophobia. On slit-lamp examination, wh ich was not thor ough due to p oor coope- ration, an iris mass nearly obstructing the visual axis was noted; the patient was then scheduled for detailed ex- amination under general anesthesia. Under the operating microscope, an iris cyst was found stemming from the previous pupilloplasty site and extending superiorly to the 12 o’clock position and inferiorly to the 6 o’clock position, apposing at the center of the pupil (Figure 1). To secure the visual axis, we performed partial excision of the wall along the border of anterior and posterior pigment epithelium and obtained a histopathologic spe- cimen. The well positioned intraocular lens and flat reti- na were noticed at the end of surgery. At postoperative 2 months, her uncorrected visual acuity was 20/32, and there was no recurrence of iris cyst up to 3 years. With hematoxylin and eosin staining, the outer wall of the cyst was seen to consist of iris pigment epithelium containing melanin pigment granules and the inner wall was found to be stratified squamous epithelial cells (Fig- ure 2(A)). On immunohistochemical staining, the inner wall showed positive staining for cytokeratin (CK) 19 (monoclonal, 1:100; Dako, Glostrup, Denmark), which is specific for limbal, peripheral corneal and conjunctival epithelium (Figure 2(B)), negative staining for CK3 (monoclonal, 1:100; Biotechnology, Santa Cruz, Calif.), which is specific for corneal epithelium (Figure 2(C)), and vimentin (monoclonal, predilution; Dako, Glostrup, *Conflicts of Interest and Source of Funding: No conflicts of interest are declared. #Corresponding author. Copyright © 2013 SciRes. OJOph 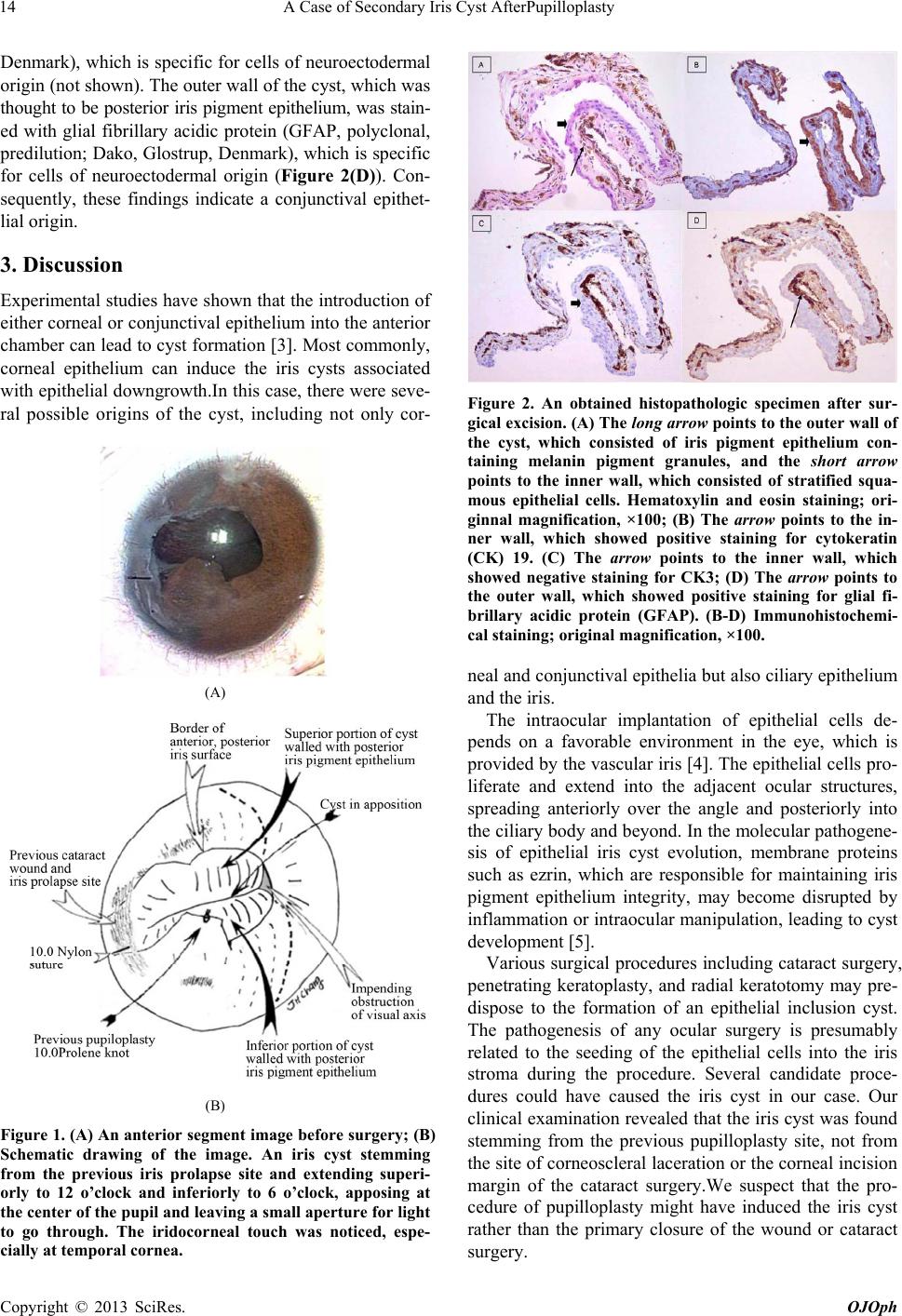 A Case of Secondary Iris Cyst AfterPupilloplasty 14 Denmark), which is specific for cells of neuroectodermal origin (no t shown). The ou ter wall of the cyst, wh ich was thought to be posterior iris pigment epithelium, was stain- ed with glial fibrillary acidic protein (GFAP, polyclonal, predilution; Dako, Glostrup, Denmark), which is specific for cells of neuroectodermal origin (Figure 2(D)). Con- sequently, these findings indicate a conjunctival epithet- lial origin. 3. Discussion Experimental studies have shown that the introduction of either corneal or conjun ctival epithelium into the anterior chamber can lead to cyst formation [3]. Most common ly, corneal epithelium can induce the iris cysts associated with epithelial downgrowth.In th is case, there were seve- ral possible origins of the cyst, including not only cor- (A) (B) Figure 1. (A) An anterior segment image before surgery; (B) Schematic drawing of the image. An iris cyst stemming from the previous iris prolapse site and extending superi- orly to 12 o’clock and inferiorly to 6 o’clock, apposing at the center of the pupil and leaving a small aperture for light to go through. The iridocorneal touch was noticed, espe- cially at temporal cornea. Figure 2. An obtained histopathologic specimen after sur- gical excision. (A) The long arrow points to the outer wall of the cyst, which consisted of iris pigment epithelium con- taining melanin pigment granules, and the short arrow points to the inner wall, which consisted of stratified squa- mous epithelial cells. Hematoxylin and eosin staining; ori- ginnal magnification, ×100; (B) The arrow points to the in- ner wall, which showed positive staining for cytokeratin (CK) 19. (C) The arrow points to the inner wall, which showed negative staining for CK3; (D) The arrow points to the outer wall, which showed positive staining for glial fi- brillary acidic protein (GFAP). (B-D) Immunohistochemi- cal staining; original magnification, ×100. neal and conjunctival ep ithelia but also ciliary epith elium and the iris. The intraocular implantation of epithelial cells de- pends on a favorable environment in the eye, which is provided by the vascu lar iris [4]. The epithelial cells pro- liferate and extend into the adjacent ocular structures, spreading anteriorly over the angle and posteriorly into the ciliary body and beyond. In the molecular pathogene- sis of epithelial iris cyst evolution, membrane proteins such as ezrin, which are responsible for maintaining iris pigment epithelium integrity, may become disrupted by inflammation or intrao cular manipulation, leading to cyst development [5]. Various surgical procedures including cataract surgery, penetrating keratoplasty, and radial keratotomy may pre- dispose to the formation of an epithelial inclusion cyst. The pathogenesis of any ocular surgery is presumably related to the seeding of the epithelial cells into the iris stroma during the procedure. Several candidate proce- dures could have caused the iris cyst in our case. Our clinical examination revealed that the iris cyst was found stemming from the previous pupilloplasty site, not from the site of corneoscleral laceration or the corneal incision margin of the cataract surgery.We suspect that the pro- cedure of pupilloplasty might have induced the iris cyst rather than the primary closure of the wound or cataract surgery. Copyright © 2013 SciRes. OJOph  A Case of Secondary Iris Cyst AfterPupilloplasty Copyright © 2013 SciRes. OJOph 15 Therefore, ophthalmic surgeons should attempt to care- fully manipulate the iris, even wh en performing a simple procedure like pupilloplasty, to prevent secondary iris cyst formation. REFERENCES [1] F. A. Marigo and P. T. Finger, “Anterior Segment Tu- mors: Current Concepts and Innovations,” Survey of Oph- thalmology, Vol. 48, No. 6, 2003, pp. 569-593. doi:10.1016/j.survophthal.2003.08.001 [2] M. Küchle and W. R. Green, “Epithelial Ingrowth: A Stu- dy of 207 Histopathologically Proven Cases,” German Journal of Ophthalmology, Vol. 5, No. 4, 1996, pp. 211- 223. [3] D. C. Cogan, “Experimental Implants of Conjunctiva into the Anterior Chamber,” American Journal of Ophthalmo- logy, Vol. 39, No. 4, 1955, pp. 165-172. [4] J. V. Jester, R. A. Villase nor and J. Miyashiro, “Epithelial Inclusion Cysts Following Radial Keratotomy,” Archives of Ophthalmology, Vol. 101, No. 4, 1983, pp. 611-615. doi:10.1001/archopht.1983.01040010611018 [5] T. Kivela, J. Jaaskelainen, A. Vaheri and O. Carpen, “Ez- rin, a Membrane-Organizing Protein, as a Polarization Marker of the Retinal Pigment Epithelium in Vertebra- tes,” Cell and Tissue Researc h, Vol. 301, No. 2, 2000, pp. 217-223. doi:10.1007/s004410000225 |

