Health
Vol.5 No.1(2013), Article ID:26976,13 pages DOI:10.4236/health.2013.51017
The “Brain Drain”: Factors influencing physician migration to Canada
![]()
1Department of Family and Community Medicine, University of Toronto, Toronto, Canada; *Corresponding Author: LoftersA@smh.ca
2Department of Family and Community Medicine, St. Michael’s Hospital, Toronto, Cnada
3Centre for Research on Inner City Health, The Keenan Research Centre, The Li Ka Shing Knowledge Institute, St. Michael’s Hospital, Toronto, Canada
4Canadian Institutes of Health Research Strategic Training Fellowship, Transdisciplinary Understanding and Training on Research— Primary Health Care Program, London, Canada
5Lawrence S. Bloomberg Faculty of Nursing, University of Toronto, Toronto, Canada
Received 19 November 2012; revised 20 December 2012; accepted 30 December 2012
Keywords: Brain Drain; International Medical Graduates; Migration
ABSTRACT
Context: Higher income countries have an average physician density of 300 physicians per 100,000 people. In stark contrast, lower income countries have an average physician density of 17 physicians per 100,000 people. A major cause of this discrepancy is the migration of healthcare professionals from lower income to higher income countries, a phenomenon colloquially known as the “brain drain”. Objective: To explore factors that led International Medical Graduate (IMG) physicians to leave their home countries and migrate to Canada. Methods: An anonymous questionnaire with a mix of openand close-ended questions was sent to 500 randomly selected IMG physicians practicing in Ontario, Canada. Results were analyzed using a mixed-method design utilizing both descriptive statistics and a thematic analysis approach. Results: 39 physicians met inclusion criteria and completed the survey. The majority were 50 years or older, and over 60% were male. The most common reason for emigration from their home country was the socioeconomic and/or political situation, and the most common reason for selecting Canada was family issues. Suggestions for how brain drain could be stemmed fell into three broad categories: 1) more accurate information about lack of opportunities in Canada, 2) more continuing medical education opportunities in home countries, and 3) address issues such as safety and quality of life in home countries. Conclusions: This survey provides insights into the reasons for emigration and immigration for international medical graduates. The results of this survey can assist stakeholders in working toward appropriate and acceptable solutions to the brain drain.
1. INTRODUCTION
In many resource-poor nations around the world, shortages of health care professionals exist at levels that limit the ability to provide even basic health care in a consistent manner and resultantly have a direct and meaningful impact on citizens’ health and wellbeing [1]. The World Health Organization has estimated the global health worker shortfall to be over 4.2 million [1]. This statistic is unsurprising considering lower-income countries have average physician densities of 17 per 100,000 population as compared to an average of 300 per 100,000 in highincome countries [2].
While there are several causes for these striking differences in physician supply, one important contributor has been the substantial migration of physicians and other health care workers from lower-income to higher-income countries, a phenomenon colloquially known as “brain drain”. The International Organization for Migration estimates that lower-income countries pay $500 million (USD) per year to train health care workers who then migrate to higher-income nations [3].
Methods of slowing this mass migration are clearly needed. Health workers who have already migrated may best be able to provide valuable insight as to why the brain drain has reached its current proportions and how both lowand high-income nations could address this issue. In this study, a random sample of International Medical Graduate (IMG) physicians in Ontario, Canada were surveyed regarding the factors that led them to immigrate and their opinions about how to best stem the brain drain in low-income countries.
2. METHODS
Using the College of Physicians and Surgeons of Ontario (CPSO) registration database, 500 physicians were randomly selected for potential inclusion in the study. Approximately 70% of practicing physicians in Ontario have agreed to the release of their information through the CPSO for study purposes [4]. Criteria for being included in the random selection pool were having an active, independent practice license, having a primary practice address in Ontario, and having graduated from a non-Canadian medical school.
The survey (Appendix 1) consisted of questions in three broad categories: 1) demographics, including the world region in which the respondent was born and attended medical school, 2) factors that led the physician to emigrate from their home country (“push” factors), and 3) factors that led the physicians to immigrate to Canada (“pull” factors). Most questions were closeended, but open-ended questions allowed participants to describe any recruitment methods they may have encountered, describe influential push and pull factors, and make suggestions for how lowand middle-income countries could retain physicians and other health professionals. The survey was created based on the existing literature regarding causes of physician migration. It was pretested for clarity, relevance of questions and survey length with staff physicians in the St. Michael’s Hospital Department of Family and Community Medicine in Toronto, Ontario who had global health expertise and/or were foreign-trained. It was approximated to take ten minutes or less to complete. The study received approval from the St. Michael’s Hospital Research Ethics Board.
Data collection occurred over a three-month period (August 2012 through October 2012). Initial contact with the five hundred physicians consisted of a mailed information sheet including the link to the anonymous online survey housed by Survey Monkey (www.surveymonkey.com). Each letter was personally addressed to the physician to whom it was mailed and was signed by two of the co-investigators (AL and NT). One month after this initial contact, a personally addressed reminder letter was sent to all physicians. Responses were not tracked as this has been shown to negatively affect physician response rate [5].
Canadian respondents (both those born in Canada and those born elsewhere but raised in Canada) who went abroad for their medical training were excluded from the analysis. We analyzed responses for closed-ended questions using the SAS version 9.3 software package (SAS Institute, Cary, NC). We performed a thematic analysis whereby free text answers were manually coded using line-by-line coding and grouped into common themes. Investigator triangulation was achieved by allowing each of the three co-authors to independently review and interpret the qualitative data prior to a robust discussion regarding emerging themes.
3. RESULTS
Of 500 mailed surveys, 18 were returned with an incorrect address. We were unable to attain correct addresses in these cases. Of the remaining 482 physicians, 45 (9.3%) completed the survey. Of these, six were excluded because they were either Canadian-born or attended high school in Canada, leaving 39 respondents whose responses were analyzed.
Table 1 describes the demographics of our study participants. Confidence intervals are not provided, as we cannot say with confidence that we have a representative sample. The majority were 50 years or older and over 60% were male. While all world regions are represented in the study population, many physicians were born, raised and/or medically trained in Sub-Saharan Africa, South Asia and the Middle East and North Africa. Respondents had graduated from medical school an average of 31 years prior, had been in Canada an average of 23 years, and had been practicing medicine independently in Canada for 18 years. An average of five years (standard deviation 4.2) passed between the time of arriving in Canada and beginning to practice medicine independently.
A diversity of specialties was represented by the survey respondents, with 23.1% working as family or general practitioners (data not shown). Just over 25% of respondents reported that their current specialty was not the same as the specialty in which they had either been trained or practiced before coming to Canada, but only 20% of this group would prefer to practice in their previous specialty.
Only two survey respondents reported that they were likely to return to their home country to practice medicine, and only five were likely to return to their home country at any point in the future to live (Table 2). The minority of respondents (18.0%) had friends or family to whom they send or had sent remittances (data not shown). Four respondents reported experiencing recruitment methods from Canada, the USA, New Zealand and South Africa in their migration process (data not shown).
When questioned about their reasons for emigration, the majority of respondents indicated they left their home countries because of the socioeconomic and/or political situation (Figure 1(a)). When asked about reasons for immigration to Canada, 39% stated they chose Canada
Table 1. Demographics of study participants (n = 39).

Missing data included in analyses.
Table 2. Likelihood of return to home country at any point in the future, n (%).
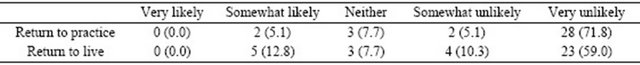
Missing data included in analyses.
for family-related issues e.g. marriage to a Canadian (Figure 1(b)). Just under 44% of respondents indicated some level of agreement with wanting to emigrate from their home country (push factors), with 28.2% strongly agreeing, while 51.3% agreed that they wanted to immigrate to Canada (pull factors), with 10.3% strongly agreeing (Table 3). Small sample size precluded any meaningful cross-tabulation analyses or subgroup comparisons.
Suggestions from respondents on how lower-income countries could stem brain drain fell into three broad themes: 1) provide more accurate information about the opportunities (or lack thereof) in Canada; 2) offer more continuing medical education opportunities in home countries; and 3) address issues around safety, quality of life, low-quality medical systems and political strife in home countries. One respondent noted that the Canadian consulate often stated that Canada needed doctors but never
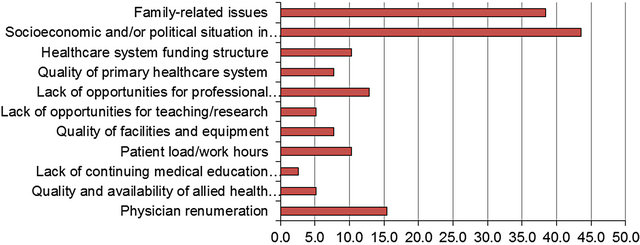 (a)
(a) (b)
(b)
Figure 1. (a) Reasons for emigration; (b) Reasons for immigration.
Table 3. Agreement with wanting to emigrate from home country and wanting to immigrate to Canada, n (%).

Missing data included in analyses.
explained that, “many of the doctors that were coming to Canada would not be able to work here, and would be here selling pizza, credit cards, driving taxi...”. Another suggested that low-income countries need to “remove the feeling of isolation” by encouraging visiting physicians from high-income countries to provide education on the latest medical advances. As one physician stated:
It’s all about quality of life. There will always be a small, dedicated percentage of physicians will work their whole lives under terrible conditions because they feel they have a calling to dedicate their lives to the sick. There is also a small non-dedicated percentage who feel that medicine simply gives them a licence to get rich. Between these two extremes, there is (in my opinion) a majority of physicians who enjoy practicing their profession but whose primary concern in life is still their own family and the betterment of their family circumstances. Physicians will stay in a low-income country if they feel appreciated and rewarded for what they do, and if they and their family feel safe.
4. DISCUSSION
Through a survey of a random sample of foreigntrained physicians in independent practice in Ontario, we have highlighted some key issues for consideration by health care policy planners whose aim is to stem mass physician migration. Our results suggest that foreign-born and foreign-trained physicians in Ontario are more strongly pushed than pulled into migrating, often settling in Canada as opposed to other countries for family reasons, but leaving their home countries due to unfavorable socioeconomic and political climates. Addressing these issues will require governmental support from the highest levels to make the practice of medicine more appealing for physicians considering migration. Our results indicate that high-income countries like Canada can do their part by contributing to continuing medical education opportunities in resource-poor nations and clearly communicating the limited opportunities for employment within the healthcare sector that exist within their borders.
Interestingly, the modal response as to where our respondents were from was Sub-Saharan Africa. Although our small sample size precludes any extrapolation to the demographics of all foreign-born physicians in Ontario, this finding is consistent with the literature that indicates that Sub-Saharan Africa is one of the areas hit hardest by health worker migration [6-9]. For example, South Africa’s estimated loss of returns from investment for physicians who have migrated is US$1.41 billion [10] and the World Health Organization estimates that 25% of doctors trained in Africa are working in high-income countries [11]. Unfortunately, Sub-Saharan Africa is also the area with the highest HIV prevalence in the world and arguably in greatest need of health care workers [12, 13].
Defendants of mass migration have argued that the home country benefits from the departures as health care workers send large amounts of money back home [7,14]. Although remittances from all migrant workers are the second-largest source of external funds for low-income countries [15], we did not find a high level of remittances within our study population. This might reflect that the family and friends of IMGs may be in a relatively higher socioeonomic bracket in the home country than the general populace. The literature argues that knowledge acquired abroad can be brought back home [9,16]; however, our results suggest that physicians rarely intend to return home, especially to practice medicine.
A review of the literature found three recent studies that explored physician brain drain. Syed et al. found that medical students in Pakistan considered moving abroad because of poor remuneration and poor quality of training (i.e. push factors) [17]. Kaushik et al. collected data on graduates of a medical school in India and found that better quality graduates (as defined by the number of awards they received) were more likely to migrate [18]. The number of physicians who returned was miniscule. Hagander et al. surveyed 66 surgeons practicing in the USA (denominator unknown) who were from lowand middle-income countries and, in contrast to our results, the most influential factors for migration were related to professional reasons as opposed to socioeconomic factors [19]. In addition, 56% of respondents had returned to their home countries at some point to contribute to clinical work, research and education. The difference in findings is not clear but may be related to specifics around the specialty of surgery.
Limitations
This study has several limitations. Most notably, our response rate was quite low and our respondents accordingly may not be a representative sample. For example, many of our respondents were males over the age of 50 years and had been in the country for an average of approximately 20 years. Their experience might not reflect that of IMGs who have arrived in Ontario in more recent years. Also, respondents frequently refused to answer certain questions, further decreasing the power of our results. The use of surveys to reach physicians in Canada is known to be problematic [20]. Despite the use of techniques expected to increase response rates, such as a personalized invitation letter [21], an anonymous survey [5], minimal time required for completion, a reminder being sent to all physicians [21], and despite the survey focusing on a topic of relevance to foreign-trained physicians, we achieved a response rate even lower than would be expected from previous studies about survey participation among physicians (14% - 34%) [2,3,22,23]. Our low response rate could reflect the sensitive nature of this issue for many foreign-trained physicians. The low response rate could also suggest that foreign-trained physicians may be less likely to participate in research studies than Canadian-trained physicians, perhaps due to there being less of a culture of research participation in other countries. We could not find any studies in the literature that have addressed response rates among foreign-trained physicians. Incentives might have increased participation rates [21,23-25]; however, due to cost, we were unable to provide monetary incentives. In addition, while the survey was sent via mail, physicians were expected to complete an online survey. Response rates may have been higher with either an emailed invitation combined with an online survey, or a paper survey combined with the mailed invitation. However, it was not possible to obtain physician emails and the use of a paper survey was limited by cost.
While our study has provided some useful data to help understand the issue of physician migration, many questions still remain unanswered. Our results suggest that foreign-trained physicians may be less likely to participate in surveys for research purposes than their Canadian-trained peers. More study is needed to explore if this finding is consistent, and if so, to determine the reasons why. It appears to be difficult to survey large numbers of IMGs; however, with a larger sample size, bivariate and multivariate analyses might provide useful region-specific information. Researchers need to ensure that IMGs are appropriately represented in any physician-relevant study.
Our findings also suggest that future research on physician international migration may benefit from the inclusion of qualitative methods, such as focus groups or interviews. This survey touched upon many personal issues and participants might be more receptive to discussing these issues in person than in a quantitative format. The viewpoints of foreign-trained physicians who have arrived more recently in Ontario and have not yet obtained a residency position will also be important to explore. Other foreign-trained health professionals, such as nurses, who play an equally important role in health care in both lowand high-income countries are also part of the brain drain phenomenon and it is imperative that their experiences be investigated. The perspectives of physicians who continue to practice medicine in their home countries and choose not to migrate could also provide a crucial piece to the brain drain puzzle.
Finally, two Global Forums on Human Resources for Health have occurred since 2008. These forums were held in an attempt to find ways to improve human health resources at the global level and to achieve the healthrelated Millennium Development Goals. A Global Code of Practice was born out of the first forum, calling for ethical recruiting, prioritizing public sector spending on health, and fair treatment of migrant workers. It would be informative to receive feedback from migrant physicians on the perceived utility and impact of this code [3,8, 26,27].
5. CONCLUSION
The global shortage of health care workers is not a problem that will go away on its own: in the past thirty years, the number of foreign-trained doctors in countries that are members of the Organization for Economic Cooperation and Development has tripled [3]. Sustainable solutions can be found, but this will only happen if the global community, including researchers, policymakers and health care workers themselves, come together and takes definitive action toward these solutions. The results of this survey can assist these stakeholders in working toward appropriate and acceptable solutions.
![]()
![]()
REFERENCES
- World Health Organization (2008) Do most countries have enough health workers? WHO. http://www.who.int/features/qa/37/en/index.html
- Dovlo, D. (2005) Taking more than a fair share? The migration of health professionals from poor to rich countries. PLOS Medicine, 2, e109. doi:10.1371/journal.pmed.0020109
- Lopes, C. (2008) Restrictions on health worker migration proving problematic. Canadian Medical Association Journal, 178, 269-270. doi:10.1503/cmaj.071818
- College of Physicians and Surgeons of Ontario (2010) Request for Information Form. http://cpso.on.ca/uploadedFiles/policies/policies/policyitems/batch_information_request.pdf
- Akl, E.A., Gaddam, S., Mustafa, R., Wilson, M.C., Symons, A., Grifasi, A., et al. (2011) The effects of tracking responses and the day of mailing on physician survey response rate: Three randomized trials. PloS One, 6, e16942. doi:10.1371/journal.pone.0016942
- World Health Organization (2008) 10 facts on health workforce crisis. WHO. http://www.who.int/features/factfiles/health_workforce/en/index.html
- World Health Organization (2010) Migration of health workers: Fact sheet No. 301. WHO. http://www.who.int/mediacentre/factsheets/fs301/en/index.html
- Connell, J., Zurn, P., Stilwell, B., Awases, M. and Braichet, J.M. (2007) Sub-Saharan Africa: Beyond the health worker migration crisis? Social Science & Medicine, 64, 1876-1891. doi:10.1016/j.socscimed.2006.12.013
- Mullan, F. (2005) The metrics of the physician brain drain. The New England Journal of Medicine, 353, 1810-1818. doi:10.1056/NEJMsa050004
- Mills, E.J., Kanters, S., Hagopian, A., Bansback, N., Nachega, J., Alberton, M., et al. (2011) The financial cost of doctors emigrating from sub-Saharan Africa: Human capital analysis. BMJ, 343, d7031. doi:10.1136/bmj.d7031
- Hooper, C.R. (2008) Adding insult to injury: The healthcare brain drain. Journal of Medical Ethics, 34, 684-687. doi:10.1136/jme.2007.023143
- Morison, L. (2001) The global epidemiology of HIV/ AIDS. British Medical Bulletin, 58, 7-18. doi:10.1093/bmb/58.1.7
- Fortson, J.G. (2011) Mortality risk and human capital investment: The impact of HIV/AIDS in Sub-Saharan Africa. The Review of Economics and Statistics, 93, 1-15. doi:10.1162/REST_a_00067
- Schuchman, M. (2008) Economist challenges recruiting hyperbole. Canadian Medical Association Journal, 178, 379-380.
- Scott, M.L., Whelan, A. and Dewdney, J. (2004) “Brain drain” or ethical recruitment? Solving health workforce shortages with professionals from developing countries. Medical Journal of Australia, 180, 174-176.
- Aly, Z. and Taj, F. (2008) Why Pakistani medical graduates must remain free to emigrate. PLOS Medicine, 5, e2. doi:10.1371/journal.pmed.0050002
- Syed, N.A., Khimani, F., Andrades, M., Ali, S.K. and Paul, R. (2008) Reasons for migration among medical students from Karachi. Medical Education, 42, 61-68. doi:10.1111/j.1365-2923.2007.02904.x
- Kaushik, M., Roy, A., Bang, A.A. and Mahal, A. (2008) Quality of medical training and emigration of physicians from India. BMC Health Services Research, 8, 279. doi:10.1186/1472-6963-8-279
- Hagander, L.E., Hughes, C.D., Nash, K., Ganjawalla, K., Linden, A., Martins, Y., et al. (2012) Surgeon migration between developing countries and the United States: Train, retain, and gain from Brain Drain. World Journal of Surgery, 37, 14-23. doi:10.1007/s00268-012-1795-6
- Grava-Gubins, I. and Scott, S. (2008) Effects of various methodologic strategies: Survey response rates among Canadian physicians and physicians-in-training. Canadian Family Physician, 54, 1424-1430.
- Field, T.S., Cadoret, C.A., Brown, M.L., Ford, M., Greene, S.M., Hill, D., et al. (2002) Surveying physicians: Do components of the “Total Design Approach” to optimizing survey response rates apply to physicians? Medical Care, 40, 596-605. doi:10.1097/00005650-200207000-00006
- Viera, A.J. and Edwards, T. (2012) Does an offer for a free on-line continuing medical education (CME) activity increase physician survey response rate? A randomized trial. BMC Research Notes, 5, 129. doi:10.1186/1756-0500-5-129
- James, K.M., Ziegenfuss, J.Y., Tilburt, J.C., Harris, A.M. and Beebe, T.J. (2011) Getting physicians to respond: The impact of incentive type and timing on physician survey response rates. Health Services Research, 46, 232-242. doi:10.1111/j.1475-6773.2010.01181.x
- Hawley, K.M., Cook, J.R. and Jensen-Doss, A. (2009) Do noncontingent incentives increase survey response rates among mental health providers? Administration & Policy in Mental Health, 36, 343-348. doi:10.1007/s10488-009-0225-z
- Camunas, C., Alward, R.R. and Vecchione, E. (1990) Survey response rates to a professional association mail questionnaire. Journal of the New York State Nurses Association, 21, 7-9.
- No authors list (2008) A global dialogue on a global crisis. Lancet, 371, 1138.
- Pagett, C. and Padarath, A. (2007) A review of codes and protocols for the migration of healt workers. The Regional Network for Equity in Health in East and Southern Africa (EQUINET) with the Health Systems Trust.
Appendix 1