World Journal of AIDS
Vol.07 No.02(2017), Article ID:76230,15 pages
10.4236/wja.2017.72008
Knowledge, Attitude and the Prevalence of HIV Counselling and Testing among Secondary In-School Adolescents in Orlu Local Government Area, Imo State, Nigeria
Anthony C. Iwu1*, Henry N. Chineke2, Kevin C. Diwe3, Chukwuma B. Duru3, Kenechi A. Uwakwe3, Emmanuel C. Azuike4, Ugochukwu C. Madubueze5, Chukwuyem Abejegah6, Emmanuel U. Ndukwu1, Ikechi Ohale1
1Department of Community Medicine, Imo State University Teaching Hospital, Orlu, Nigeria
2Department of Family Medicine, Imo State University Teaching Hospital, Orlu, Nigeria
3Department of Community Medicine, Imo State University, Owerri, Nigeria
4Department of Community Medicine, Chukwuemeka Odumegwu Ojukwu University, Anambra, Nigeria
5Department of Community Medicine, Federal Teaching Hospital, Abakaliki, Nigeria
6Department of Community Medicine, Irrua Specialist Teaching Hospital, Irrua, Nigeria

Copyright © 2017 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY 4.0).
http://creativecommons.org/licenses/by/4.0/



Received: April 22, 2017; Accepted: May 15, 2017; Published: May 18, 2017
ABSTRACT
Background: Adolescence is a period of vulnerability with the onset of multiple risky behaviour which exposes them to HIV and other sexually transmitted diseases and as such, the timely introduction and uptake of strategies like HIV Counselling and Testing will reduce transmission and provide access to preventive services. Objective: To assess the knowledge, attitude and prevalence of HIV Counselling and Testing among secondary in-school adolescents in Orlu Local Government Area, Imo State, Nigeria. Methods: A cross sectional analytical study design was used that selected students aged 13 - 19 years in senior classes SS1 to SS3 attending secondary schools. Data was collected using a pretested, semi-structured questionnaire. Descriptive analyses were done with frequencies and summary statistics. Chi square statistic was computed and p value was set at 0.05 significant level. Results: Though most of the respondents were aware of HIV/AIDS (99%) and HIV Counselling and Testing (92%), the majority of the respondents had a poor level of overall knowledge (61%) and attitude (70%) towards HIV Counselling and Testing. The prevalence of HIV Counselling and Testing amongst the respondents was very low (7%). Furthermore, there was a statistically significant relationship between the level of overall knowledge and level of overall attitude towards HIV Counselling and Testing (p < 0.000). Conclusion: Identifying and closing the gaps in their knowledge and attitude towards HIV Counselling and Testing, will form the basis for the introduction of adolescent-tailored strategies that will further encourage and improve voluntary and confidential uptake of HIV Counselling and Testing among the adolescents.
Keywords:
HCT, Knowledge, Attitude, Prevalence, Adolescents, Nigeria

1. Introduction
Human Immunodeficiency virus (HIV) infection produces a potentially devastating and transmissible disease of the immune system but with the introduction and strict adherence to antiretroviral therapy, it has become a chronic manageable disease, with people infected with HIV now living a long, healthy and productive life [1] [2] .
In 2012, an estimated 2.1 million adolescents worldwide were living with HIV, with about 33% of all new infections occurring in young people aged 15 - 24 years, out of which, 39% occurred in adolescents aged 15 - 19 years [3] .
In 2015, Western and Central Africa had an estimated 6.5 million people living with HIV, out of which, 500,000 were children (0 - 14 years) and 650,000 were young people (15 - 24 years). Also in that year, newly acquired infections were estimated to be 410,000 out of which, 66,000 were children, 110,000 were young people and 36,000 were adolescents (15 - 19 years) with an estimated 60% of these new infections occurring in Nigeria [4] .
Adolescence is a period of vulnerability with the onset of multiple risky behaviour such as smoking, inappropriate alcohol consumption and drug use, with the consequences of an increased risk of engaging in unprotected, multiple sexual experiences [3] [5] . This further exposes the adolescent to HIV/AIDS and other sexually transmitted diseases, and as such, they are central to the prevention and control of the HIV/AIDS epidemic with respect to the degree of their vulnerability, transmission and potential for behavioral change [6] .
In spite of the fact that in-school adolescents are still under some form of guidance from parents, caregivers or school authorities, they appear to be influenced mostly by their peers and the environment; and as a consequence, they are involved in experimenting in sexuality, sexual orientation and other new experiences [3] [7] . In Central and West African region, it has been reported that up to 16% of adolescent girls had sex before the age of 15 years and as such, it has been recognized that adolescence is a period when sexual activity begins [7] [8] . This early commencement of sex, fueled by the lack of adequate information within the context of social, cultural and economic factors, provides more opportunities over time for an increased risk of exposure to HIV [7] [8] .
Even with the knowledge of HIV/AIDS, adolescents still have several misconceptions about transmission and they do not perceive themselves to be at risk of being infected, as this could encourage the practice of unsafe sexual behavioral habits [3] [9] [10] [11] . This lack of appropriate health information coupled with limited access to reproductive health services, economic and sexual exploitation, early coerced sex and participation in other risky behaviour will also predispose the adolescent to increased risk of HIV infections [12] [13] .
The adolescents, not only have an increased risk of HIV/AIDS from behavioral transmission but also from vertical transmission (mother to child). The infection from vertical transmission could be slow, progressing from infancy into adolescence without treatment; as up to 33% of HIV infected infants not commenced on treatment, become slow progressors with a median survival of more than 10 years [14] . Vertical transmission is as significant as behavioral transmission in the spread of HIV/AIDS within the general population, as a substantial epidemic of perinatally infected adolescents appear to be emerging because their mothers were missed or not covered by prevention of maternal to child transmission (PMTCT) programmes or they were lost to follow-up. Hence, there is an increasing proportion of perinatally infected HIV children who are entering adolescence undiagnosed. Furthermore, in high prevalent areas, HIV is becoming a common cause of acute hospital admissions and death among adolescents [13] [15] [16] . Therefore, instituting the practice of adolescent HIV counselling and testing (HCT) is critical to the prevention and control of HIV/AIDS.
HCT uptake among adolescents has been low, due to factors such as perception of staff judgmental attitude, confidentiality of the process and result, stigmatization and more especially the policy regarding age of consent to testing [9] [13] . The age of consent serves as a barrier which further limits certain groups of adolescents from accessing HCT because of the requirement to inform and get consent from their parents or guardians; as adolescents are often reluctant to seek services that require parental consent [4] .
In Nigeria, the adolescents’ rights are limited, as there are several issues surrounding the age of consent especially for HCT among adolescents, as this has hampered progress in adolescent management and research of HIV/AIDS and other sexual reproductive health issues. In 2014, the Nigerian Federal Ministry of Health issued guidelines for age of consent in therapeutic and non-therapeutic research; as any person aged 16 and 13 years and above respectively [17] . Notwithstanding, this still poses an additional barrier to addressing the sexual reproductive issues of adolescents especially within the ages of 13 - 16 years who are now increasingly experimenting and engaging in unsafe sexual activities with the risk of being infected [3] [8] . So the assessment of the knowledge, attitude and prevalence of HCT among senior secondary in-school adolescents, will enable the identification of gaps in their knowledge, attitude and uptake of HCT and therefore, form the basis for the introduction of adolescent-tailored strategies which will also include, the advocacy of policies to remove age restrictions and other adolescent barriers.
2. Methodology
2.1. Study Area
The study was conducted in Orlu Local Government Area (LGA), one of the 27 LGA’s of Imo State which is in South Eastern part of Nigeria. Orlu LGA occupies an area of 132.9 sq. km with a population density of about 1074 persons per sq. km [18] .
2.2. Study Population
The study population comprised, students aged 13-19 years in senior classes SS1 to SS3 attending public secondary schools in Orlu LGA.
2.3. Inclusion/Exclusion Criteria
Inclusion criteria; students in the senior classes SS1 to SS3, aged 13 to 19 years in the school register of selected secondary schools as at June 2016. Exclusion criteria; selected students from the register that were absent from school during the study.
2.4. Sample Size Estimation
The minimum sample size was estimated using Cochran formula [19]
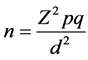
when n = minimum sample size, Z = Standard normal deviate corresponding to the probability of type I error is 1.96, p = prevalence of HCT among adolescents from Nigeria Demographic and Health Survey 2013 [20] is 7.7% q = 1 − 0.077, d = tolerable error of margin set at 0.05. The minimum sample size calculated was 109 but the researchers increased the sample size to 300 participants to accommodate the possibility of incomplete or non-response.
2.5. Study Design and Sampling Technique
The study was a cross sectional analytical design that used simple random sampling techniques to select four secondary schools and enroll 300 students after permission from the selected school authorities and verbal consent from the participating students were given. Firstly, from the sampling frame of 18 public secondary schools in Orlu LGA, four secondary schools were selected by simple random sampling using ballots. Secondly, within each secondary school, from each of the arms of the senior classes SS1, SS2 and SS3, twenty-five students were selected irrespective of gender from their respective school registers by simple random sampling using table of random numbers. The selected students that did not consent or were absent during the conduct of the study were excluded and replaced through further random selection from the school register.
2.6. Data Collection and Analysis
In each of the selected schools, 75 students were enrolled and assembled in two classrooms where data was collected from them using a pretested semi-struc- tured self-administered questionnaire. The questionnaire was pretested in a secondary school located in another LGA, outside the study area, that established content validity and a reliability coefficient (alpha) of 0.83.
The questionnaire comprised 4 sections; section one: the socio-demographic characteristics, section two: knowledge of HIV/AIDS, section three: knowledge of HCT and section four: Attitude towards HCT. The level of knowledge of HCT was determined by scoring the questions that assessed knowledge. For a single response question, a correct answer was scored 2; an incorrect answer was scored 0. For a multiple response question, up to five answers, every correct answer was scored 1 and incorrect answer was scored 0. In assessing the level of attitude towards HCT, for a single response question, an answer connoting a positive attitude was scored 2 and a negative or not sure attitude was scored 0. For a multiple response question, up to five answers, every answer connoting a positive attitude was scored 1 and for any answer connoting a negative or not sure attitude was scored 0. The aggregate scores for each respondent according to the level of knowledge and attitude towards HCT were translated to a percentage and assessed against a scale of less than 60% for poor and greater than 60% for good.
Data was cleaned and validated manually then analyzed using Software Package for Social Sciences (IBM-SPSS) version 22. Descriptive statistics (frequency tables and summary indices) were generated. Chi Square was used to test and determine any significant association between knowledge and attitude towards HCT and p value was set at 0.05 significance level.
2.7. Ethical Considerations
Ethical approval was obtained from the Ethics Committee of Imo State University Teaching Hospital Orlu. Permission from the selected school authorities and informed consents were obtained. All authors hereby declare that the study has therefore been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki.
3. Results
Three hundred copies of the questionnaire were administered and were completely and correctly filled giving a response rate of 100%.
3.1. Sociodemographic Characteristics of Respondents
Majority of the respondents were female (55.3%) and within the ages of 16-18 years (67.7%) with most belonging to the Christian faith (93.3%) of Igbo ethnic extraction (96.7%) (Table 1).
3.2. Respondents’ Knowledge of HIV/AIDS
Almost all of the respondents were aware of HIV/AIDS (99%). All and most of the respondents that were aware of HIV/AIDS respectively, indicated that the school (100%) and television (95%) were amongst their sources of information. Only about 23% of those aware, indicated that friends and relatives were sources of awareness.
More than three quarters of the respondents aware of HIV/AIDS, knew that
Table 1. Sociodemographic characteristics.
the mode of transmission were sexual intercourse (87%) and sharing injections (82%) while as many as 7 to 18% of those aware, indicated that sharing toilet (7%), eating with infected person (8%), sharing towels/handkerchief (17%) and mosquito bites (18%) were also modes of transmission. Close to one quarter of the respondents aware of HIV/AIDS, were not aware of the associated high risks behaviour (23%). Of those aware of the associated high risks, a majority indicated that unprotected sex (72%) was high risk but only 7% indicated that intravenous drug use was. More than half of the respondents (54.6%) either did not know or indicated that condom use cannot prevent HIV infection. Also, only about half and close to half of the respondents respectively, indicated that HIV can be treated (50%) but not cured (47%) (Table 2).
3.3. Respondents’ Knowledge of HIV Counselling and Testing (HCT)
Most of the respondents were aware of HCT (92%). Of those aware, all and most of the respondents respectively indicated that the school (100%) and the media (94%) were their sources of information. A majority of the respondents aware of HCT did not know any location for HCT services (65%) but, most knew that HCT is provided by health clinics (94%). Though a majority of the respondents aware of HCT indicated that, you seek HCT services at any time (67%), about 8 to 12% also indicated that, you seek HCT services for medical fitness certification and only when, one is feeling sick. A majority of the respondents aware of HCT, interpreted a positive HIV test to mean that the person definitely has AIDS (42%) while the interpretation of about 18% was that, the person will definitely die of the disease (Table 3).
Most of the respondents (93%) reported that, they had not been counselled and tested for HIV infection (Figure 1).
A majority of the respondents had a poor level of the overall knowledge of HCT services (61%) (Figure 2).
Table 2. Knowledge of HIV/AIDS.
*Multiple responses.
Figure 1. Prevalence of HIV counselling and testing.
Table 3. Knowledge of HIV counselling and testing.
*Multiple responses.
Figure 2. Level of overall knowledge of HCT.
3.4. Respondents’ Attitude towards HIV Counselling and Testing (HCT)
Most of the respondents aware of HCT felt that everyone should perform HCT (94%) and the majority of the respondents’ reason was to know their HIV status (59%). The majority of those aware of HIV/AIDS felt that, the most important reason that will make them not test for HIV, is the likelihood that they are not exposed to HIV (37%) while about 12% felt, it was the fear of testing positive. The majority of respondents aware of HCT either felt that, they would not change or were not sure that, they would change their lifestyle after receiving HCT (67%). A majority of the respondents aware of HIV/AIDS felt that, if they were tested positive, they would seek medical treatment and avoid infecting others, while about 17% felt that they would seek spiritual care (Table 4).
A majority of the respondents had a poor level of overall attitude towards HCT services (70%) (Figure 3).
3.5. Association between Respondents’ Knowledge and Attitude towards HIV Counselling and Testing
The level of overall knowledge of HCT was significantly associated with the level of overall attitude towards HCT among the respondents (p < 0.000). (Table 5)
4. Discussion
This study assessed the Knowledge, Attitude and the Prevalence of HIV Counselling and Testing among senior secondary in-school adolescents and it revealed that the majority of the respondents had a poor level of overall knowledge and attitude towards HCT with a very low prevalence of HCT uptake. It further revealed that the overall level of knowledge among the respondents was significantly associated with the overall level of attitude towards HCT.
In the present study, the awareness of HIV/AIDS among the respondents was high and it was observed that the school was the most important source of information followed by the media, specifically the television. This was similar to a Cameroonian study by Haddison et al. [21] among high school students, where it was observed that there was high awareness of HIV/AIDS and their source of
Figure 3. Level of overall attitude towards HCT.
Table 4. Attitude towards HIV counselling and testing.
*Multiple responses.
Table 5. Association between knowledge and attitude towards HCT.
*Significant.
information was mainly from the school followed by the media. Other studies also reported a high level of HIV/AIDS awareness [9] [11] [22] [23] [24] but Nubed et al. [9] a Cameroonian study, reported that, while the school was the main source of information, the television was the least source for the students. This was contrary to a Nigerian study by Bamise et al. [23] who reported that, the media specifically television was the major source of information for secondary school adolescents. Also, an Indian study by Kameshore et al. [24] , reported that books, teachers and media in that order were the main sources of information. Though, it was observed commonly across these studies that there is a high awareness of HIV/AIDS among adolescents, it was also observed that, their main sources of information varied. Hence, in order to continue to improve knowledge and maintain the high level of HIV/AIDS awareness among successive cohorts of adolescents, it is important that the multi-channel approach to information dissemination be strengthened; and continue to remain a part of the strategy in addressing adolescent health issues.
In spite of the high level of awareness observed in the present study, there is a need to improve the comprehensive knowledge of HIV among the adolescents, as a relatively sizeable proportion of the respondents still had misconceptions of HIV/AIDS transmission; for example, where some respondents reported that sharing toilet, eating with infected persons, sharing towels/ handkerchiefs and mosquito bites were the modes of HIV transmission and also, where only a small proportion of the respondents were aware of intravenous drug use as a high risk behaviour, with more than half of the respondents either not knowing or having reported that, condom use cannot prevent HIV infection. These misconceptions about HIV transmission among the respondents were also observed in other studies [9] [11] [24] [25] . Furthermore, in Nigeria, Aomreore et al. [26] also reported that, knowledge about the transmission of HIV was poor in senior high school students and this, further highlighted the existing concerns of misconception as a source that could perpetuate HIV transmission and discriminatory attitudes. Hence, it is important that the information being disseminated about HIV/AIDS is comprehensive, and it continues to emphasize on condom use as a preventive measure and also, on the various modes of transmission, as this may further help reduce transmission, stigmatization and discrimination of people living with HIV/AIDS.
HCT is one of the main strategies for reducing the transmission of HIV, providing access to preventive services and reinforcing preventive messages on HIV. It may, in addition, also reduce risky behavioral tendencies among people who have received a HCT and are HIV negative [2] . In the present study, the prevalence of HCT among the respondents was as low as 7% which appear to be consistent with the NDHS 2013 [20] that reported a prevalence of 7.7% among adolescents within the ages of 15-19 years. Similarly, a previous study by Ibrahim et al. [27] analyzing the Nigerian National HIV/AIDS and Reproductive Health Survey 2007, also reported a prevalence as low as 10% among young people within the ages of 15 - 24 years. On the contrary, some other studies [9] [21] [28] [29] appear not to be consistent, as they reported higher prevalence rates of HCT among young people as ranging from 19% - 41%.
Generally, the prevalence of HCT uptake among young people in a community or region seems to be dependent on the impact of HIV disease, public policies and the degree of public health efforts. This may explain to some extent, why there are varying degrees of HCT uptake amongst them, across regions. Nevertheless, any strategy that improves knowledge and a positive attitude towards HCT among the young people especially the adolescents within a youth friendly, non-judgmental and confidential environment, will also be fundamentally important and beneficial in improving uptake; because, any increase in HCT knowledge and positive attitude during the adolescents’ period, will definitely be facilitated by the effect of peer influence.
Furthermore, the study by Haddison et al. reported that, the uptake of HCT was significantly associated with knowledge and attitude towards HCT. Though the present study found that, the level of overall knowledge was significantly associated with the level of overall attitude, there were observed knowledge and attitudinal gaps. These gaps were further highlighted in the present study, where it was observed that, a majority of the respondents had a poor level of overall knowledge and attitude, which could also, have contributed to the low uptake of HCT observed among the respondents.
In spite of the fact that most of the respondents in the present study were aware of HCT, the gaps were obvious, for example, where a majority of the respondents did not know of any HCT location, with up to one quarter of them, having reported that HCT should be sought only before marriage and also, when more than one third of the respondents felt that, being tested for HIV is not needed since they are unlikely to be exposed. A similar attitude was observed in a study among secondary school students by Tarkang et al. [10] who reported that a majority of them did not perceive themselves to be at risk of being infected with HIV. Similar gaps in knowledge and attitude, in spite of high level of HCT awareness, were also observed in other studies which for example, reported that, up to one third to half of the respondents either did not know where to go for HCT services or did not feel that HCT was meant for students or necessary for them [21] [28] [29] . Finally, this study emphasizes on the need to improve HCT knowledge and attitude amongst in-school adolescents; because, an adequate and appropriate knowledge and attitude towards HCT is fundamentally required, in order for adolescent tailored strategies for HCT uptake to be effective.
5. Conclusion
In-school adolescents, a subgroup of different developmental levels and behavioral risks, have in common some form of parental or guardian supervision. In spite of this, they are exposed to risky behavioral tendencies within the context of inadequate knowledge and poor social values which further exposes them to the risk of HIV and other sexually transmitted diseases. The in-school adolescents are poorly equipped to handle these situations, not only because they are faced with socio-political and environmental challenges of uptake of preventive and treatment measures such as HCT, they lack comprehensive knowledge and the appropriate attitude towards these measures. So improving knowledge and attitude of adolescents towards HCT will close the knowledge and attitudinal gaps and form the basis for the implementation of adolescent tailored strategies that address their socio-political and environmental challenges and consequently encourage and improve the voluntary and confidential uptake of HCT.
Acknowledgements
We thank all the participants in this study and the research assistants who helped during the data collection.
Authors’ Contributions
All the authors participated in the study.
Competing Interest
The authors hereby declare that there are no competing interests.
Source of Funding
There was no external source of funding.
Cite this paper
Iwu, A.C., Chineke, H.N., Diwe, K.C., Duru, C.B., Uwakwe, K.A., Azuike, E.C., Madubueze, U.C., Abejegah, C., Ndukwu, E.U. and Ohale, I. (2017) Knowledge, Attitude and the Prevalence of HIV Counselling and Testing among Secondary In-School Adolescents in Orlu Local Government Area, Imo State, Nigeria. World Journal of AIDS, 7, 77-91. https://doi.org/10.4236/wja.2017.72008
References
- 1. May, M.T., Ingle, S.M., Costagliola, D., Justice, A.C., de Wolf, F., Cavassini, M., et al. (2014) Cohort Profile: Antiretroviral Therapy Cohort Collaboration (ART-CC). International Journal of Epidemiology, 43, 691-702.
https://doi.org/10.1093/ije/dyt010 - 2. Uwakwe, K.A., Uwakwe, G.C., Iwu, A.C., Duru, C.B., Nnebue, C.N. and IIika, A.L (2016) Knowledge, Attitude and Uptake of HIV Voluntary Counselling and Testing among Undergraduates in a Tertiary Institution in Owerri, Imo State. European Journal of Pharmaceutical and Medical Research, 3, 326-333.
- 3. United Nations Children’s Fund (UNICEF) (2013) Towards an AIDS-Free Generation—Children and AIDS: Sixth Stocktaking Report. UNICEF, New York.
aids_en_0.pdf>http://www.unaids.org/sites/default/files/media_asset/20131129_stocktaking_report_children_
aids_en_0.pdf - 4. Joint United Nations Programme on HIV/AIDS (UNAIDS) (2016) Prevention Gap Report.
http://www.unaids.org/sites/default/files/media_asset/2016-prevention-gap-report_en.pdf - 5. DuRant, R.H., Smith, J.A., Kreiter, S.R. and Krowchuk, D.P. (1999) The Relationship between Early Age of Onset of Initial Substance Use and Engaging in Multiple Health Risk Behaviors among Young Adolescents. Archives of Pediatrics and Adolescent Medicine, 153, 286-291.
https://doi.org/10.1001/archpedi.153.3.286 - 6. UNAIDS Inter-Agency Task Team on Young People (2004) At the Crossroads: Accelerating Youth Access to HIV/AIDS Interventions. Joint United Nations Program on HIV/AIDS.
www.un.org/esa/socdev/unyin/documents/aidsunfpa.pdf - 7. Idele, P., Gillespie, A., Porth, T., Suzuki, C., Mahy, M., Kasedde, S. and Luo, C. (2014) Epidemiology of HIV and AIDS among Adolescents: Current Status, Inequities, and Data Gaps. Journal of Acquired Immune Deficiency Syndromes, 66, 144-153.
- 8. United Nations Children’s Fund (UNICEF) (2013) Global Databases 2008-2012. Based on DHS, MICS and Other National Surveys. UNICEF, New York.
- 9. Nubed, C.K. and Akoachere, J.T.K. (2016) Knowledge, Attitudes and Practices Regarding HIV/AIDS among Senior Secondary School Students in Fako Division, South West Region, Cameroon. BMC Public Health, 16, 847.
https://doi.org/10.1186/s12889-016-3516-9 - 10. Tarkang, E.E. (2014) Factors Associated with Perception of Risk of Contracting HIV among Secondary School Female Learner in Mbonge Subdivision of Rural Cameroon. The Pan African Medical Journal, 17, 259.
https://doi.org/10.11604/pamj.2014.17.259.2772 - 11. Thanavanh, B., Rashid, H.O., Kasuya, H. and Sakamoto, J. (2013) Knowledge, Attitudes and Practices Regarding HIV/AIDS among Male High School Students in Lao People’s Democratic Republic. Journal of the International AIDS Society, 16, Article ID: 17387.
https://doi.org/10.7448/IAS.16.1.17387>http://www.jiasociety.org/index.php/jias/article/view/17387
https://doi.org/10.7448/IAS.16.1.17387 - 12. Chen, F.P. (2008) HIV/AIDS Prevention among Young People in East and South-East Asia in the Context of Reproductive and Sexual Health. Asia-Pacific Population Journal, 23, 7-28.
- 13. World Health Organization (WHO) (2013) HIV and Adolescents: Guidance for HIV Testing and Counselling and Care for Adolescents Living with HIV: Recommendations for a Public Health Approach and Considerations for Policy-Makers and Managers.
http://apps.who.int/iris/bitstream/10665/94334/1/9789241506168_eng.pdf?ua=1 - 14. Bygrave, H., Mtangirwa, J., Ncube, K., Ford, N., Kranzer, K. and Munyaradzi, D. (2012) Antiretroviral Therapy Outcomes among Adolescents and Youth in Rural Zimbabwe. PLoS ONE, 7, e52856.
https://doi.org/10.1371/journal.pone.0052856 - 15. Ferrand, R.A., Bandason, T., Musvaire, P., Larke, N., Nathoo, K., Mujuru, H., et al. (2010) Causes of Acute Hospitalization in Adolescence: Burden and Spectrum of HIV-Related Morbidity in a Country with an Early-Onset and Severe HIV Epidemic: A Prospective Survey. PLoS Medicine, 7, e1000178.
https://doi.org/10.1371/journal.pmed.1000178 - 16. Ferrand, R., Lowe, S., Whande, B. and Corbett, E. (2010) Survey of Children Accessing HIV Services in a High Prevalence Setting: Time for Adolescents to Count? Bulletin of the World Health Organization, 88, 428-434.
https://doi.org/10.2471/BLT.09.066126 - 17. Federal Ministry of Health (FMoH) (2014) Guidelines for Young Persons’ Participation in Research and Access to Sexual and Reproductive Health Services in Nigeria.
http://www.popcouncil.org/uploads/pdfs/2014HIV_YoungPersonsSRH-Nigeria.pdf - 18. National Population Commission (NPC) (2006) Federal Republic of Nigeria 2006 Population and Housing Census: Priority Table Volume III.
http://www.population.gov.ng/index.php/censuses - 19. Cochran, W.G. (1963) Sampling Technique. 2nd Edition, John Wiley and Sons Inc., New York.
- 20. National Population Commission (NPC) [Nigeria] and ICF International (2014) Nigeria Demographic and Health Survey 2013. NPC and ICF International, Abuja, Nigeria, and Rockville, Maryland, USA.
- 21. Haddison, E.C., Nguefack-Tsague, G., Noubom, M., Mbacham, W., Ndumbe, P.M. and Mbopi-Keou, F.X. (2012) Voluntary Counselling and Testing for HIV among High School Students in Tiko Health District, Cameroon. The Pan African Medical Journal, 13, 18.
- 22. Tarkang, E. (2009) Knowledge, Attitudes and Perceptions Regarding HIV/AIDS and Sexual Behaviours among Senior Secondary School Learners in Kumba, Cameroon. PhD Thesis, University of South Africa, Pretoria.
- 23. Bamise, O.F., Bamise, C.T. and Adedigba, M.A. (2011) Knowledge of HIV/AIDS among Secondary School Adolescents in Osun State, Nigeria. Nigerian Journal of Clinical Practice, 14, 338-344.
https://doi.org/10.4103/1119-3077.86780 - 24. Kameshore, N., Singh, K.B., Minita, N. and Avinash, K. (2014) Knowledge and Attitude on HIV/AIDS among Students of Higher Secondary Schools in Imphal: A Cross Sectional Study. Journal of Evolution of Medical and Dental Sciences, 3, 11922-11928.
https://doi.org/10.14260/jemds/2014/3573 - 25. Tavoosi, A., Zaferani, A., Enzevaei, A., Tajik, P. and Ahmadinezhad, Z. (2004) Knowledge and Attitude towards HIV/AIDS among Iranian Students. BMC Public Health, 4, 17.
https://doi.org/10.1186/1471-2458-4-17 - 26. Aomreore, A.A., Alikor, E.A. and Nkanginieme, K.E. (2004) Survey of Knowledge of HIV Infection among Senior Secondary School 3 (SSS3) Students in Port Harcourt. Nigerian Journal of Medicine, 13, 398-404.
- 27. Ibrahim, M., Ipadeola, O., Adebayo, S. and Fatusi, A. (2013) Socio-Demographic Determinants of HIV Counseling and Testing Uptake among Young People in Nigeria. International Journal of Prevention and Treatment, 2, 23-31.
- 28. Omary, S. (2008) Barriers and Attitudes towards HIV Voluntary Counselling and Testing among Secondary School Pupils in Sengerema in Mwaza. Tanzania Medical Students Association.
https://www.ajol.info/index.php/dmsj/article/viewFile/49596/35924 - 29. Abebe, A. and Mitikie, G. (2009) Perception of High School Students towards Voluntary HIV Counselling and Testing, Using Health Belief Model in Butajira, SNNPR. Ethiopian Journal of Health Development, 23, 148-153.





