Journal of Biosciences and Medicines
Vol.05 No.11(2017), Article ID:80437,7 pages
10.4236/jbm.2017.511002
Importance of Primary Health Care in Medicine: Simultaneous Analysis of Two Colleges, under the Vision of Teachers and Students
Sebastião Célio Horta Coelho Filho1, Thiago Sande Miguel1, Nayrton Kalys Cruz dos Anjos1, Mateus de Oliveira Reis1, Bruna Sande Miguel2, Vinicius Sande Miguel2, Aline Gabriela Santos Costa1, Lilian Costa Brito1, Bruno Fonseca dos Santos1, Verônica Clemente Villar Martini1, Daniel Almeida da Costa1
1The Medical School at the Center of Higher Education of Valença, Valença, Brazil
2Unigranrio Medical School, Rio de Janeiro, Brazil
Copyright © 2017 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY 4.0).
http://creativecommons.org/licenses/by/4.0/



Received: August 15, 2017; Accepted: November 17, 2017; Published: November 20, 2017
ABSTRACT
Introduction: The involvement of undergraduate student at the beginning of their training in activities based on Primary Health Care (PHC), provides preventive and health promoting actions, and ensures the evaluation of the vulnerability of communities and people. Objectives: To analyze the opinion of students and teachers of two medicine higher education institutions on the relevance of Primary Health Care in this course. METHODS: Students and teachers should be effectively enrolled in order for the study to be conducted, being chosen in a random manner and without interferences on the part of the researchers so that the work was as reliable as possible. A cross-sectional study was conducted with interviews structured in questionnaires about what they thought about PHC. To some students and teachers of the medical course of Valença and Grande Rio University (UNIGRANRIO). Before receiving the questionnaire, all interviewed signed a Free and Informed Consent Term, which included the objectives and methodology of the work. Results: 310 students and 51 teachers participated in the study, where 91.43% of the students and 100% of the teachers affirmed that primary care plays a fundamental role in medical education. 94.86% of students and 97.91% of teachers, claimed that the discipline allows a greater contact between undergraduates and community. When questioned about the encouragement that teachers give to students to pursue a career in PHC, 57.87% of the students and 70.83% of the professors said they lacked in such a stimulus. Conclusion: PHC is still very neglected by governmental policies, educational institutions and by the own teachers, that often, turn they attention only to tertiary medicine and, as a consequence, a discouragement of this area occur. Therefore, a higher PHC value is necessary, allowing a more humane look at the patient, valuing their feelings, anguishes and their pathological framework.
Keywords:
Primary Health Care, Graduation, Medicine

1. Introduction
Primary Care is one of the most important health components, since it is the organizational strategy of care, defined by principles and guidelines of generalized care, presenting no restrictions on age groups, gender, or health problems, being person centered, not disease centered, keeping track of the users in other attentions, always focusing on the psychosocial well-being of those who provide services [1] [2] [3] [4] .
An idea of health care focused on individual curative care, molded in sophisticated diagnostic methods and advanced treatment forms has been observed in the health area. However, the population needs and demands are not fully effective. In the process of medical training, more specialties are arriving, making a great impact on their practice organization, fragmenting health care. At under graduation, these specialties are in the curriculum, multiplying in contents and disciplines, losing the general understanding of health actions, with the progressive modification of the subjectivism between doctor-patient relations for a technological complementary diagnosis complementary objectivism [5] [6] [7] .
Despite the expansion of PHC in undergraduate studies, there is an increasing tendency for technology-oriented medicine, fragmented into subspecialties and disease centered, in detriment of subjectivism and generalist knowledge, that often enables correct data collection and obtain essential diagnosis information, without requiring other complement methods for patient’s approach [1] [8] .
Learning fragmentation, often influenced by educational institutions and teachers, encourages the emergence of interest in different areas, in order to create a hierarchy and disarticulate a combined knowledge structure, which differs from the reality lived in the medical practice, where integration of different sectors is required in a patient approach [1] [9] [10] .
After graduating in medicine, when the professional becomes a general doctor, he ends up being undervalued, because of the numerous specialties that have being appearing, impacting and fragmenting the approaches and interventions that leaded to a high disinterest in the common knowledge formation to every doctor [1] [11] [12] [13] .
In the academic context, the PHC allows a bigger contact between the student and the reality lived by the majority of the Brazilian population, since the beginning of its graduation [13] [14] [15] .
This fact already inserts the doctor to be in a theoretical-practical context, based on a scientific literary knowledge and in the possibility of realizing it, where there is greater concern with resources management, for both: the possible patient iatrogenic and their availability. As opposed to some forms of learning, where theory and practice can be quickly experienced, PHC requires a real approximation between student and community over time, that enables a better structure in the process of Construction of knowledge, through coexistence [1] [11] [12] [13] .
Training students in the health area requires a structure based on a greater flow of theoretical information associated with a constant practice. This teaching way allows the student to position himself and to have a critical sense of the context around him, expressing his opinions and inquiries based on a scientific technical knowledge directed by his preceptors [11] [14] [15] .
The need for changes in the health courses curriculum with a global focus on concepts involving prevention and health promotion, planning effective measures in the treatment and control of pathologies, combining efficient technologies and forms of learning that transcend spaces and reach the population reality [11] [16] [17] .
Involving the graduate since the beginning of their degree, in practical activities, based on PHC, provides a necessary and potential area, because it enables the graduate to have real daily experiences when faced with unusual clinical situations, where both, experience and humane look on the patient, make him a more competent professional, with an evaluation of the vulnerability of people and communities [17] [18] .
2. Objectives
To carry out a survey of data that show the opinion of students and professors of the medicine course of Valência Medical School and the Grande Rio University (UNIGRANRIO) on the importance of PHC in the graduation, making a comparison of the opinion of teachers and students on the subject.
3. Material and Methods
A cross-sectional study was conducted with interviews structured as a questionnaire to students and teachers of basic and professional cycle of the medical course of the Valença Medical School and Grande Rio University-Rio de Janeiro. A total of 310 students were duly enrolled in medicine, and 51 medicine professors from both colleges, were selected. Before receiving the questionnaire, all interviewed signed a Free and Informed Consent Term, which included the objectives and methodology of the study.
All questionnaires addressed to students were composed of twelve questions, and the teachers of eleven questions, respectively, with questions about their opinion about the importance of PHC in medical training. All information collected was coded, scanned and processed in an Excel®2010 worksheet. The results were analyzed through descriptive statistical data and presented as graphs (Graph 1 and Graph 2).
The work was submitted and approved by the Brazil Platform (CAAE N˚ 47757415.9.0000.5246).
4. Results
An amount of 267 students (91.43%) and 48 teachers (100%) stated that PHC plays a fundamental role in medical education.
In addition, the opinion of 277 students (94.86%) and 47 teachers (97.91%) confirmed that the discipline allows a greater contact between undergraduates and the community. When asked about teachers’ encouraging students to pursue careers in primary care, 169 students (57.87%) and 34 teachers (70.83%) said that there was a lack of encouragement from teachers.
Regarding the role of colleges in students’ participation in PHC activities, 187 students (64.04%) and 22 teachers (45.83%) said that institutions insert academics in an appropriate way. The main reasons given by the students when asked why so few professionals decided to pursue a career in PHC were: lack of adequate infrastructure, little public policy stimulation and inadequate remuneration.
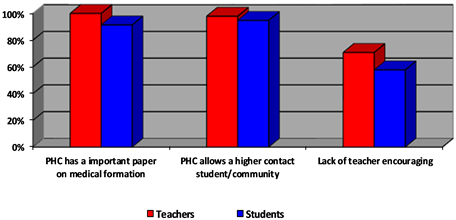
Graph 1. Students and teachers about PHC.
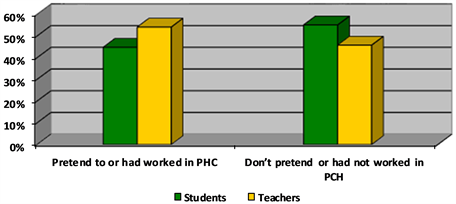
Graph 2. Students that pretend or not to work in PHC and professionals that worked or.
Among the teachers these were: lack of adequate infrastructure, lack of career prominence and inadequate remuneration. As a result, 131 undergraduates (44.86%) intend to work at some point in their lives in primary care, opposed by 161 (55.14%) who do not want to focus on primary care. Nevertheless, 26 teachers (54.16%) have already exercised activities in basic health care at some point in their lives, against a total of 22 (45.84%) that didn’t. Among the reasons that led the teachers to not pursue a career in primary care are: choosing another area of work, admission to medical residency, few working conditions and lower than expected compensation.
The exclusion criteria consisted in incorrect and/or incomplete completion of any alternatives, leading to 18 students and three teacher’s questionnaires being discarded.
5. Discussion
PHC must present a resolution between 85% and 90% in order to attend patients who would seek help at a reference center and/or in an emergency, reducing hospitalization rates for various morbidity groups. In view of this, the importance of such a subject in the academic framework, is evident, because, not only keep the student updated in literary terms, but also it allows an extended and particular approach of each patient [13] [18] . This corroborates with the data obtained in the collection of Data from this study, where 267 individuals (91.43%) and 48 teachers (100%) stated that PHC plays a fundamental role in medical education.
Teaching PHC allows the student to know how to deal with collective and individual simultaneously, adopting measures that benefit whole population, but also respect the particularity of each case in its clinical and cultural scope. Integrality, with a holistic focus on the individual, from prevention to healing and rehabilitation, associated with teamwork based on interdisciplinarity, contributes to a medical education aimed to a higher resolution when faced with everyday clinical problems, since that, knowing other areas of health, such as nursing, physiotherapy and odontology, contribute to a more fulfilled approach on the individual, enriching the case and solving it whenever possible. Therefore, it allows a greater experience of academics in their future reality, experienced after graduation [8] [9] [18] . In view of this, it is noticeable that great majority, evidenced by 277 students (94.86%) and 47 teachers (97.91%) corroborate that the discipline allows a greater contact between undergraduates and the community, a situation that will be experienced by the academics in their professional future.
Not only the students require a learning structure that allows a rapid flow of information and facilities to this, but also that teachers play a fundamental role of filtering information, horizontalizing access to knowledge and being one of the responsible of a foundation of brain that are relevant in a context where the amount of information may be lost or not be assimilated consistently. In addition, the stages longitudinality in PHC should be a longer period of follow-up so that academics and teachers can establish better links with the public, moving closer to each case [1] [7] [11] . It can be interfered that teachers’ encouraging to students to pursue careers in primary care is precarious. This is evidenced according to 169 students (57.87%) and 34 teachers (70.83%) opinions, which has negative repercussions on the medical education of these students, since they may be harmed by the lack of proper preceptory in their training, regarding theoretical aspects associated to a more humanistic view of each case. As a result of this situation, 131 undergraduates (44.86%) intend to work at some point in their lives in primary care, as opposed to 161 (55.14%) who do not focus on primary care. As can be seen, a greater stimulation of the students to seek this specialization is necessary, from a more solid base in the PHC faculties, since there are a lot of students who claim that they will be carrying out activities in the PHC, but that don’t intend to pursue that career.
There is a need that the medical training process, should pursue actively a wide range of settings for its teaching, as well as an early academic insertion into theoretical-practical activities since the earliest stages of the course. A large part of the Brazilian population lives in unfavorable contexts, highlighting the need for medical schools to stimulate competent vocational training capable of intervening in such a scenario. A practical and theoretical part of medicine with a focus on PHC can be applied since the first year, based on illustrated learning forms in home visits, management policies and educational measures in preventive and curative health [9] [18] . However, it was not the opinion of students and teachers interviewed, about students’ insertion at an early stage into a context of PHC, since there are few incentives and conditions for such practice, according to 187 students (64.04%) and 22 professors (45.83%).
6. Conclusion
Although it is part of fundamental training of all health professionals, especially medical students, PHC is still very neglected, by the institutions their teachers and students. Thus, it is necessary to break up isolated sector practices and strengthen the integrality of health actions, seeking a maximum interaction between efficient government policies, education, social action, environment protection and income generation, as a way to promote sustainable development.
Cite this paper
Filho, S.C.H.C., Miguel, T.S., dos Anjos, N.K.C., de Oliveira Reis, M., Miguel, B.S., Miguel, V.S., Costa, A.G.S., Brito, L.C., dos Santos, B.F., Martini, V.C.V. and da Costa, D.A. (2017) Importance of Primary Health Care in Medicine: Simultaneous Analysis of Two Colleges, under the Vision of Teachers and Students. Journal of Biosciences and Medicines, 5, 6-12. https://doi.org/10.4236/jbm.2017.511002
References
- 1. Ministério da Saúde (2001) Departamento de Atenção Básica. Guia prático do programa de saúde da família. Ministério da Saúde, Brasília.
- 2. Andrade, M.M. (2003) Proposal for the Recovery of Historiographic Data: SESP/ FSESP Souruces in the Study of Immunization Campaigns in Brazil. History, Science and Health, Manguinhos, 10.
- 3. Brasil. M S. Secretaria de Atenção à Saúde (2006) Departamento de Atenção Básica. Política Nacional de Atenção Básica. Ministério da Saúde, Brasília.
- 4. Giovanella, L. and Mendonça, M.H. (2008) Manual de Atenção Primária à saúde. Políticas e sistema de saúde no Brasil. Fiocruz, Rio de Janeiro.
- 5. Machado, M.F.A.S., Monteiro, E.M.L.M., Queiroz, D.T., Vieira, N.F.C. and Barroso, M.G.T. (2007) Integration of Health Surveillance and Women’s Health Care: A Study on Comprehensiveness in the Unified National Health System. Ciência Saude Coletiva, 12, 335-342. https://doi.org/10.1590/S1413-81232007000200009
- 6. Campos, M.A.F. and Forster, A.C. (2008) The Importance of the Family Medicine Experience from the Viewpoint of Students of a Public Medical School. Revista Brasileira de Educação Médica, 32, 83-89. http://www.scielo.br/pdf/rbem/v32n1/11.pdf
- 7. Bollela, V.R., Germani, A.C.C.G., Campos, H.H. and Amaral, E. (2014) Educação Baseada na Comunidade para as Profissoes da Saúde: Aprendendo com a Experiência Brasileira. FUNPEC, Ribeirao Preto.
- 8. Brasil. Ministério da Saúde. Secretaria de Atenção à Saúde. Departamento de Atenção Básica. (2012) PNAB—Política nacional de atenção básica. Ministério da Saúde, Brasília.
- 9. Ferreira, R.C., Da Silva, R.F. and Aguer, C.B. (2007) Formação do profissional médico: A aprendizagem na atenção básica de saúde. Revista Brasileira de Educação Médica, 31, 52-55. https://doi.org/10.1590/S0100-55022007000100008
- 10. Brasil. Ministério da Saúde. Ministério da Educação. Organização Panamericana da Saúde. (2002) PROMED: Programa de incentivo a mudanças curriculares nos cursos de medicina. Secretaria de Políticas da Saúde, Brasília.
- 11. Campos, G.W.S. (2005) Papel da rede de atenção básica em saúde na formação médica: diretrizes: documento preliminar. ABEM, Rio de Janeiro.
- 12. Anderson, M.I.P., Demarzo, M.M.P. and Rodrigues, R.D. (2007) Family and Community Medicine, Primary Careand Undergraduate Medical Education: Recommendations and Potentialities. Rev Bras Med Fam e Com, 3, 157-172.http://www.rbmfc.org.br/index.php/rbmfc/article/viewFile/334/222
- 13. Franco, T.B. and Magalhães Jr., H.M. (2007) Integralidade na assistência a saúde: a organização das linhas do cuidado. In: Merhy, E.E., Magalhães Jr., H.M., Rimoli, J. and Franco, T.B., Eds., O trabalho em saúde: Olhando e experienciando o SUS no cotidiano, Hucitec, São Paulo, 125-133.
- 14. Oliveira, N.A. (2007) Ensino Médico no Brasil: Desafios e prioridades, no contexto do SUS—Um estudo a partir de seis estados brasileiros. Instituto Oswaldo Cruz, Rio de Janeiro.
- 15. Costa, N.M.S.C. (2007) Medical Teaching: Why Is It So Difficult to Change? Revista Brasileira de Educação Médica, 31, 21-30. https://doi.org/10.1590/S0100-55022007000100004
- 16. Gomes, A.P. and Rego, S. (2011) Transformation of Medical Education: Can a New Physician be Trained Based on CHANGES in the Teaching-Learning Method? Revista Brasileira de Educação Médica, 35, 557-566. https://doi.org/10.1590/S0100-55022011000400016
- 17. Rego, S., Gomes, A.P. and Siqueira-Batista, R. (2008) Bioethics and Humanization Across the Curriculum in Medical Education. Revista Brasileira de Educação Médica, 32, 482-491. https://doi.org/10.1590/S0100-55022008000400011
- 18. Piancastelli, C.H. (2001) Saúde da família e formação de profissionais de saúde. In: Arruda, B.K.G., Org., A educação profissional em saúde e a realidade social, Instituto Materno Infantil de Pernambuco: MS, Recife, 121-140.

